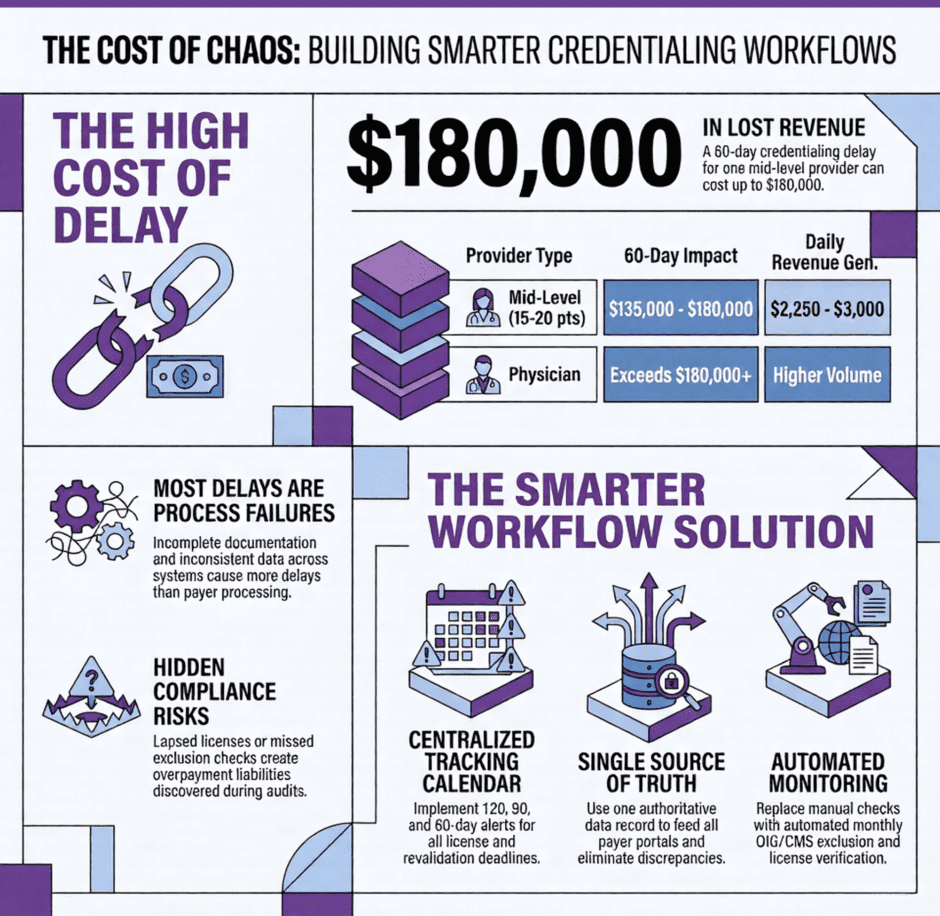
A disorganized credentialing workflow costs the average medical practice between $2,250 and $3,000 per provider per day in unbillable revenue while applications are pending. For a physician with higher visit volume or specialty reimbursement rates, that number climbs higher. Most of that lost revenue is preventable.
 The most common credentialing delays are not caused by payers moving slowly. They are caused by missing documents, inconsistent data across applications, and no one tracking revalidation deadlines until billing stops. Those are process problems, and they have process solutions.
The most common credentialing delays are not caused by payers moving slowly. They are caused by missing documents, inconsistent data across applications, and no one tracking revalidation deadlines until billing stops. Those are process problems, and they have process solutions.
We cover where credentialing workflows break down most often, what a functional workflow looks like at a practical level, and how to stop losing revenue to delays your team could have caught earlier.
What Credentialing Delays Cost Providers
Before getting into the solutions, it is worth being direct about what is at stake financially. When a provider cannot bill because their credentialing is not complete, the practice is not just inconvenienced. It is losing money every single day that provider sees patients.
A mid-level provider seeing 15 to 20 patients per day at an average reimbursement of $150 per visit generates somewhere between $2,250 and $3,000 in daily revenue. A credentialing delay of 60 days for that single provider can cost the practice $135,000 to $180,000 in lost or deferred revenue. For a physician with higher visit volume or a higher reimbursement rate, the numbers are worse.
That math is not hypothetical. It plays out in practices every month across the country, and in most cases, a meaningful portion of that delay was preventable with a more organized credentialing process.
Beyond the direct revenue impact, credentialing delays create compliance risk that most practices do not think about until something goes wrong. A provider whose license quietly expired during the credentialing window, an exclusion check that was never run at onboarding, a revalidation deadline that was missed because no one was tracking it. Each of those is a compliance problem that can surface months later in an audit or a payer review.
Where Credentialing Workflows Break Down Most Often
The path from a new provider’s first day to their first billable date involves a lot of moving parts, and each part is a potential failure point. Here is where things go wrong most consistently.
The Document Collection Bottleneck
Document collection is the single most common source of credentialing delays, and it is almost entirely a process problem. When a practice starts collecting documents informally, chasing down diplomas, malpractice certificates, DEA registrations, board certifications, and state licenses on an ad hoc basis, the timeline becomes entirely dependent on how quickly the provider responds and how persistent the credentialing staff is willing to be.
The fix is a structured onboarding document checklist that goes to every new provider on day one of employment with clear deadlines and a defined follow-up schedule. When providers know exactly what is needed, when it is needed, and that someone will follow up if it is not received, document collection moves significantly faster.
Data Inconsistencies Across Systems
One of the most common reasons payer applications get kicked back or delayed is that the provider’s information does not match across the documents submitted. A name formatted differently on a license versus a diploma, an address that differs between PECOS and CAQH, a specialty designation that does not match the payer’s taxonomy code. These discrepancies look minor, but they create review flags that slow applications down.
This problem is almost always caused by entering provider data manually in multiple systems rather than maintaining a single accurate source that feeds everything else. Centralizing provider data and making it the authoritative record for every application reduces inconsistency errors significantly.
No Centralized Tracking or Clear Ownership
Credentialing tasks that are distributed across multiple staff members with no single source of truth are credentialing tasks waiting to be dropped. When everyone is responsible, no one is accountable. Applications that need follow-up do not get it. Revalidation deadlines that are approaching do not get flagged. License expirations that are coming up in three months do not get noticed until two weeks before the date.
The solution is not more staff. It is better process design. Assign a named owner to every open credentialing application. Build a centralized tracking system that shows the current status of every provider across every payer and facility. Make it someone’s specific job to review that tracking system on a weekly basis and move every open item forward.
Payer Portal Variations and Response Delays
Every payer has its own portal, its own document requirements, its own processing timelines, and its own method for communicating application status. Managing credentialing across a large provider roster with multiple payers means navigating a different set of rules for every combination. Without a documented payer-specific matrix that captures what each payer requires, how to submit, and how long responses typically take, the process depends entirely on whoever handled that payer last time remembering the details.
What a Smarter Credentialing Workflow Looks Like
The practices that consistently get new providers credentialed and billing faster are not necessarily larger or better staffed. They have built a process that removes guesswork and keeps every application moving forward without waiting for someone to notice it has stalled.
A smarter credentialing workflow has a few consistent element:
- Standardization comes first. Every provider goes through the same onboarding document checklist. Every application follows the same submission workflow. Every payer gets handled according to the same documented steps. Standardization does not mean ignoring payer-specific differences. It means building those differences into a documented process rather than relying on institutional memory.
- A credentialing calendar drives proactive action. This is one of the highest-impact changes a practice can make. A centralized calendar that tracks application submission dates, expected response timelines, license expiration dates, malpractice certificate renewals, DEA registration expirations, and revalidation deadlines gives your team visibility into what is coming rather than what has already been missed. Alerts at 120 days, 90 days, and 60 days before critical deadlines give staff enough lead time to act before a problem develops.
- Ownership is assigned at every stage. Each open application should have a specific person responsible for its status. Not a department, not a team, a named individual who is accountable for moving that application forward and escalating if it stalls.
- A payer-specific credentialing matrix is maintained and kept current. This document captures each payer’s submission requirements, portal access information, typical processing timeline, contact information for follow-up, and any known quirks in their process. It takes time to build but eliminates the re-learning that happens every time someone works with a payer they have not dealt with recently.
How Technology Supports Smarter Credentialing
Technology does not fix a broken credentialing process on its own, but it dramatically amplifies a well-designed one. The right tools eliminate the manual steps that consume the most time and create the most errors.
- CAQH ProView is the central credentialing data repository used by most major payers to verify provider information. Keeping a provider’s CAQH profile complete, current, and attested on schedule is one of the most time-efficient things a practice can do because it feeds into multiple payer applications automatically. CAQH profiles that are outdated or unattested create delays across every payer that pulls from that profile simultaneously.
- Automated license verification is available through credentialing platforms that connect directly to state licensing board databases. Rather than manually visiting each state board’s website to confirm license status, automated verification pulls current license data on demand. For practices with providers licensed in multiple states, this is a significant time saver and a meaningful compliance protection.
- Exclusion and preclusion monitoring needs to be automated and ongoing rather than a one-time check at hire. The OIG exclusion list and the CMS preclusion list are updated regularly, and a provider who was in good standing at hire can appear on an exclusion list at any point afterward. Running monthly automated exclusion checks across your full provider roster is the only reliable protection against billing with an excluded provider, which creates overpayment liability regardless of when the exclusion occurred.
- Document expiration tracking with automated alerts removes the risk of a license or malpractice certificate lapsing without anyone noticing. When your system automatically flags an expiring credential 90 or 120 days out, your team has time to initiate renewal before the expiration creates a billing gap.
Credentialing for Multi-Provider and Multi-Location Practices
The credentialing challenges that are manageable for a small practice become significantly more demanding as provider count and location count increase. A process that works well for five providers does not scale to twenty without intentional design.
Multi-location practices face a specific challenge in that the same provider may need to be credentialed at multiple hospitals, surgery centers, and payers, each on its own timeline. Managing that complexity requires tracking not just provider-level credentialing status but location-level and payer-level status for every provider simultaneously.
Here is a practical framework for managing credentialing at scale:
- Maintain a provider credentialing matrix that shows the status of each provider across each facility and each payer in a single view. The matrix should be updated in real time and reviewed weekly by a designated team member.
- Run hospital privileging and payer credentialing applications simultaneously for every new provider rather than waiting for one to complete before starting the other. Parallel processing reduces total onboarding time by weeks.
- Build a 90-day provider onboarding credentialing plan that starts on the provider’s first day of employment and maps every application, every document request, every expected response date, and every follow-up touchpoint through to billing activation.
When a new service line is added or a new facility is opened, credentialing planning needs to happen before the first patient appointment is scheduled, not after. The assumption that credentialing can be handled quickly when needed is what leads to practices delivering services they cannot bill for.
The Connection Between Credentialing and Revenue Cycle
 Credentialing is often treated as an HR or administrative function, separate from the revenue cycle. That separation is artificial and expensive. Credentialing directly determines whether a claim can be paid, and billing gaps caused by credentialing problems are among the most frustrating because they are entirely unrelated to clinical quality or coding accuracy.
Credentialing is often treated as an HR or administrative function, separate from the revenue cycle. That separation is artificial and expensive. Credentialing directly determines whether a claim can be paid, and billing gaps caused by credentialing problems are among the most frustrating because they are entirely unrelated to clinical quality or coding accuracy.
A claim submitted under an uncredentialed provider is a billing error by definition, and the denial that results from it typically cannot be appealed on clinical grounds because the problem is procedural. In some cases, services delivered during a credentialing gap create retroactive overpayment liability if they were billed and paid before the gap was discovered.
Revalidation is where this connection is most acute for established providers. Medicare requires periodic revalidation of all enrolled providers and organizations, and missing a revalidation deadline results in deactivation of billing privileges with no grace period. Claims submitted after deactivation are not paid until the revalidation is completed and privileges are reinstated. Building revalidation deadline tracking into the same system that manages initial credentialing is not optional for a practice that wants predictable revenue.
Payer contracting adds another dimension. When a new provider joins a group and a new contract or contract amendment is needed with one or more payers, the contracting and credentialing timelines need to be aligned. A contract effective date that precedes credentialing approval does not help anyone. Neither does a credentialing approval for a payer where no contract is in place. These two functions work best when managed in parallel.
Smrter Credentialing Workflows FAQ
- How long should provider credentialing take from start to finish?
For most payers, credentialing takes 60 to 120 days from application submission to approval. Hospital privileging can take a similar amount of time depending on committee schedules. The total timeline from a provider’s first day of employment to billing activation can stretch to four to six months if applications are not started immediately and managed proactively. Practices with structured workflows consistently achieve faster timelines than those managing credentialing informally. - What is the biggest cause of credentialing delays?
Incomplete or missing documentation at the time of application submission is the leading cause of delays. When a payer receives an application with missing credentials, it goes into a pending status until the information is provided, and the clock effectively restarts. Starting with a complete, verified application package for every payer reduces this risk significantly. - What is CAQH and how does it fit into credentialing?
CAQH ProView is a centralized provider data repository used by most major commercial payers to verify provider credentials. Providers enter and attest their information in CAQH, and participating payers pull from that database rather than requiring each provider to submit the same information separately to every payer. Keeping a provider’s CAQH profile current and regularly attested is one of the highest-impact credentialing efficiency measures available. - What is the difference between hospital credentialing and payer credentialing?
Hospital credentialing, also called privileging, is the process by which a hospital or facility verifies a provider’s qualifications and grants permission to provide specific services at that facility. Payer credentialing is the process by which an insurance company verifies a provider’s qualifications and enrolls them in their network. Both are required for a provider to deliver and bill services, but they are separate processes with separate timelines and separate requirements. - How often do providers need to be recredentialed?
Most facilities and payers require recredentialing every two to three years. Medicare revalidation is required every five years for most provider types, though some higher-risk provider types are required to revalidate more frequently. Recredentialing timelines vary by payer and facility, which is why tracking each provider’s renewal schedule across all applicable entities is an ongoing operational requirement. - When should a practice consider outsourcing credentialing?
Most practices benefit from outside credentialing support when their provider count exceeds the capacity of in-house staff to manage applications, renewals, and monitoring without something falling through the cracks. Practices that have experienced billing gaps due to credentialing delays, missed revalidation deadlines, or exclusion screening failures are also good candidates for a credentialing partner who can build and manage a structured process.
Providers also Ask
- What causes most credentialing delays in healthcare practices? The most common causes are incomplete documentation submitted with the initial application, provider data that does not match across multiple systems, applications that are submitted but not actively followed up on, and payer portals that require specific information that was not included in the original submission. Most of these are process problems, not payer problems, and they are preventable with a structured workflow.
- How does credentialing affect a practice’s revenue cycle? Directly and significantly. A provider who is not credentialed with a payer cannot have their services reimbursed by that payer. Services delivered during a credentialing gap may be denied retroactively even if they were previously paid, creating overpayment liability. Missed revalidation deadlines deactivate billing privileges entirely until the revalidation is completed. Every credentialing delay or gap is a revenue cycle problem that billing cannot solve on its own.
- What is primary source verification in credentialing? Primary source verification means confirming a provider’s credentials directly from the institution or organization that issued them, rather than relying on copies provided by the provider. Medical education is verified with the medical school. Board certification is verified with the certification board. Licensure is verified with the state licensing board. Primary source verification is required by NCQA, The Joint Commission, and most payers as part of the credentialing process.
- What is the difference between credentialing and payer enrollment? Credentialing is the broader process of verifying a provider’s qualifications, education, training, licensure, and clinical history. Payer enrollment is the specific process of submitting an application to an insurance company to participate in their network and receive reimbursement for services. Credentialing is typically a prerequisite for payer enrollment, but enrollment also involves contract terms, NPI linkage, billing structure, and reimbursement rate agreements that go beyond credential verification.
- How do you track credentialing deadlines across multiple providers? The most reliable method is a centralized credentialing management system that maintains a single record for each provider with all application dates, approval dates, license expiration dates, malpractice renewal dates, and revalidation deadlines visible in one place. Automated alerts set at 120, 90, and 60 days before critical deadlines give staff enough lead time to act. Spreadsheet-based tracking works for very small practices but breaks down quickly as provider and payer volume increases.
How Medwave Makes Credentialing Easier
 Credentialing does not have to be the part of your operation that keeps administrative staff up at night. When the process is structured, ownership is clear, deadlines are tracked proactively, and applications are managed from submission to approval, credentialing becomes a predictable, manageable function rather than a constant source of stress and revenue interruption.
Credentialing does not have to be the part of your operation that keeps administrative staff up at night. When the process is structured, ownership is clear, deadlines are tracked proactively, and applications are managed from submission to approval, credentialing becomes a predictable, manageable function rather than a constant source of stress and revenue interruption.
Medwave provides medical billing, provider credentialing, and payer contracting services to healthcare practices across the country. Our credentialing team builds and manages the structured workflows that practices need to get providers credentialed faster, keep renewals on schedule, maintain exclusion monitoring across their full roster, and avoid the billing gaps that cost real money. We coordinate hospital privileging, payer enrollment, CAQH management, and revalidation tracking so that your team is not juggling all of it manually. Since we also handle billing and contracting, we align credentialing timelines with contract effective dates and billing activation so that every new provider is revenue-ready as fast as possible.
If your practice is dealing with delays, missed deadlines, or billing gaps you suspect are credentialing-related, the first step is a workflow assessment that identifies exactly where the process is breaking down.
Contact Medwave today to schedule a credentialing workflow assessment.
COO and Co-Founder of Medwave, with over 30 years of experience in healthcare revenue cycle management, payer contracting, and medical credentialing.

