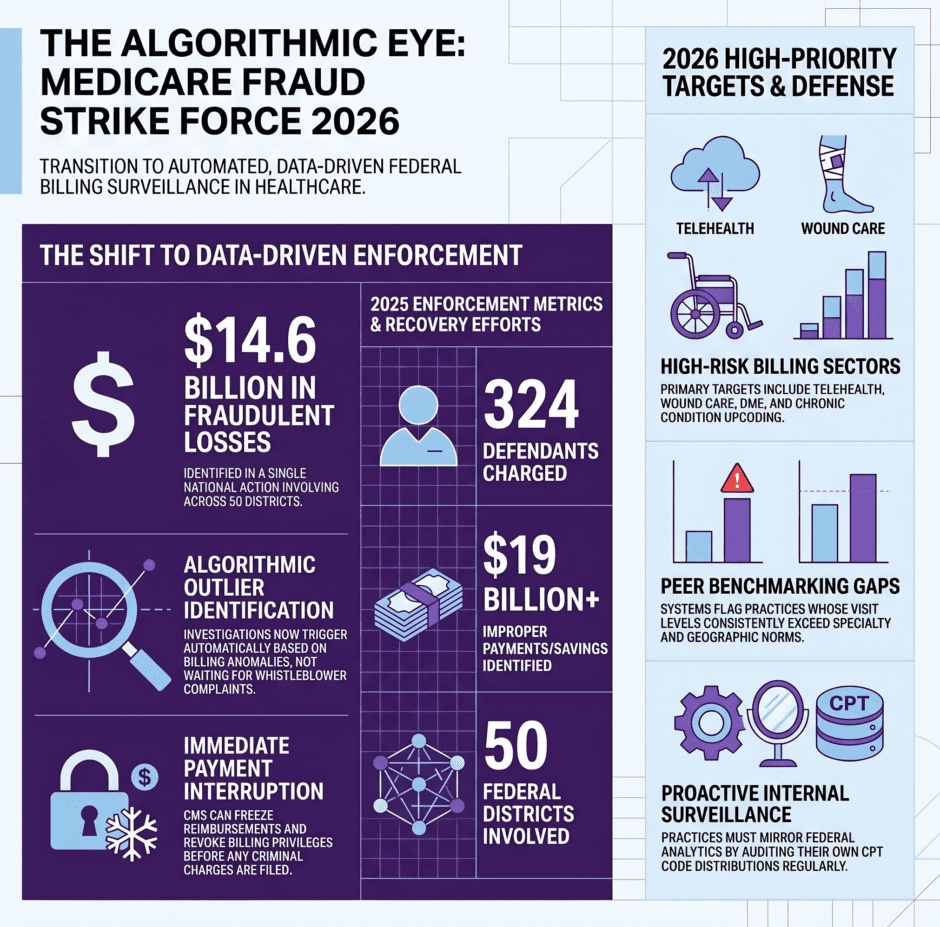
The Medicare Fraud Strike Force has changed. It’s no longer primarily a criminal prosecution team hunting obvious bad actors. In 2025, it delivered the largest single enforcement action in U.S. healthcare history. 324 defendants charged across 50 federal districts, 96 licensed medical professionals implicated, and over $14.6 billion in alleged fraudulent losses identified in a single national takedown.

Those numbers are not the whole story. The deeper story is how those providers were identified in the first place. The Strike Force did not find most of them through whistleblowers or patient complaints. It found them through a federal analytics system that flagged billing pattern anomalies before any human investigator reviewed a single chart. That process is now the operational reality for every legitimate practice billing Medicare today.
At Medwave, we pay close attention to enforcement trends that affect how our clients operate. Below, we explain what the Strike Force is, how it finds providers, what billing patterns it is targeting in 2026, and what steps practices need to take now.
TL;DR
- The Medicare Fraud Strike Force is now a federal data analytics operation, not just a law enforcement team.
- In 2025, it charged 324 defendants and identified over $14.6 billion in alleged fraudulent losses in a single national action.
- Legitimate providers with billing anomalies can enter the federal enforcement process without any criminal intent.
- The Strike Force can interrupt a practice’s payments and freeze billing privileges before any criminal charge is filed.
- High-priority enforcement targets in 2026 include telehealth, DME, wound care, home health, and diagnosis upcoding.
- Building an internal billing surveillance process now is far less costly than responding to a federal investigation later.
What’s the Medicare Fraud Strike Force
 The Medicare Fraud Strike Force was launched in 2007 as a joint initiative between the HHS Office of Inspector General, the U.S. Department of Justice, the FBI, U.S. Attorneys’ Offices, CMS program integrity units, state Medicaid fraud control entities, and local law enforcement partners. It was designed to concentrate federal enforcement resources in the highest-risk Medicare billing corridors in the country.
The Medicare Fraud Strike Force was launched in 2007 as a joint initiative between the HHS Office of Inspector General, the U.S. Department of Justice, the FBI, U.S. Attorneys’ Offices, CMS program integrity units, state Medicaid fraud control entities, and local law enforcement partners. It was designed to concentrate federal enforcement resources in the highest-risk Medicare billing corridors in the country.
Today, Strike Force teams operate in Florida, Texas, California, New York, Illinois, Louisiana, New Jersey, Pennsylvania, New England, Washington D.C., and the Appalachian region. That coverage is not arbitrary. Those are the markets where Medicare billing anomalies have historically been most concentrated, and where the return on enforcement investment is highest.
What separates the Strike Force from a standard payer audit, a RAC review, or a UPIC documentation request is the scope of what they can see and the speed at which they can act. A private payer sees its own claims data. The Strike Force sees across programs simultaneously, including Medicare Part B, DMEPOS, telehealth utilization, wound care reimbursement, pharmacy prescribing, home health billing, Medicaid overlaps, and ordering and referring patterns. That cross-program visibility lets investigators identify patterns that no single payer could detect on its own.
The other piece that most providers don’t fully appreciate is the payment interruption capacity. When the OIG deems allegations credible, CMS can suspend reimbursements, revoke billing privileges, freeze provider enrollments, or require prepayment review before any criminal liability is ever adjudicated. For many practices, that administrative intervention alone is financially devastating. A practice doesn’t need to be convicted of anything for its cash flow to be severely disrupted.
How the Strike Force Finds Providers
This is the part that changes the conversation for legitimate practices. The Strike Force no longer waits for a whistleblower complaint or a patient report to begin an investigation. Increasingly, federal enforcement starts from algorithmic outlier identification.
The system looks for unusual utilization patterns, diagnosis inflation, geographic concentration of billing, reimbursement spikes, and service combinations that are statistically improbable for a given specialty or patient population. Academic fraud detection research has confirmed that Medicare anomaly models can identify suspicious providers through claims behavior long before formal allegations are ever generated.
That means the process starts not with a moral judgment about the provider’s intentions, but with a billing signature.
A legitimate practice can enter the federal enforcement funnel through:
- Outsourced billing teams that aggressively maximize utilization without adequate documentation support
- Template-driven E/M coding that consistently produces visit levels higher than peer benchmarks without corresponding clinical documentation
- Repeated same-day code stacking that creates reimbursement patterns inconsistent with specialty norms
- Remote patient monitoring or chronic care management enrollment that lacks clear evidence of actual patient engagement
- Referral relationships that statistically resemble inducement patterns regardless of the actual intent behind them
A provider does not need criminal intent to become algorithmically suspicious. What happens after that initial flag is where intent matters. Federal investigators determine whether the anomaly reflects negligence, reckless billing practices, systemic abuse, or intentional fraud. By the time that determination is being made, the provider is already inside the enforcement process.
That is not a hypothetical risk. It is the operational reality of how Strike Force enforcement works in 2026.
What the Strike Force is Targeting Right Now
The areas drawing the most Strike Force attention in 2026 include:
- Telehealth and remote ordering schemes
Phantom virtual visits, medically unnecessary genetic testing ordered remotely, remote DME ordering, RPM documentation gaps, and what investigators describe as physician signature commoditization - Durable medical equipment and supply billing
Urinary catheters, orthotics, diabetic supplies, respiratory equipment, and consumable reorder patterns that don’t reflect actual patient need - Wound care and skin substitute claims
HHS watchdog reporting identified significant Medicare spending anomalies in bioengineered skin substitute reimbursement, prompting billions in projected federal savings actions and direct fraud scrutiny - Home health and hospice
Particularly where beneficiary eligibility documentation is templated or where physician certification patterns are repetitive across large patient populations - Diagnosis upcoding and chronic condition monetization
Not theatrical fake clinics, but ordinary-looking practices with reimbursement patterns that are statistically inconsistent with peer norms for their specialty and geography
 Federal enforcement priorities shift based on where the data shows the most concentrated billing anomalies relative to medical necessity support. The current enforcement wave has a clear pattern. The government is focused on high-margin billing sectors where documentation requirements are specific and where reimbursement inflation is possible without obvious clinical red flags.
Federal enforcement priorities shift based on where the data shows the most concentrated billing anomalies relative to medical necessity support. The current enforcement wave has a clear pattern. The government is focused on high-margin billing sectors where documentation requirements are specific and where reimbursement inflation is possible without obvious clinical red flags.
That last category is where legitimate practices most commonly underestimate their exposure. A practice that has drifted toward aggressive chronic condition coding, or whose billing team applies high-acuity codes more frequently than specialty benchmarks would predict, can look like a fraud target to a federal analytics system without anyone in the practice having done anything they believed was wrong.
Fraud Enforcement is Now a Data Science Operation
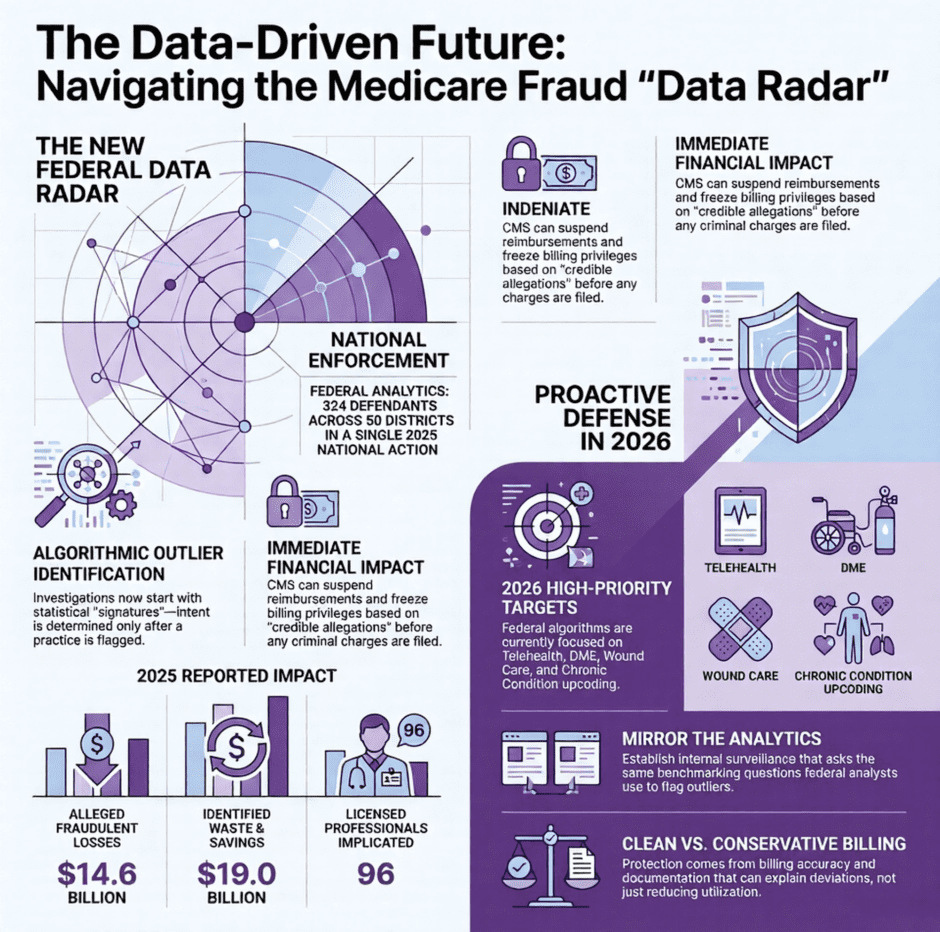
The most important change to internalize about the Medicare Fraud Strike Force in 2026 is this, it is not primarily a law enforcement operation anymore. It is a federal healthcare analytics machine.
The enforcement process now depends far more on claims clustering, provider-peer benchmarking, utilization variance detection, ownership tracing, payment acceleration analysis, beneficiary identity patterns, referral graph mapping, and reimbursement trend deviations than it does on undercover operations or tip-based investigations.
HHS watchdog reports identified more than $16.6 billion in improper payments, fraud findings, and potential savings in a single six-month 2025 review period. Fiscal year 2025 reporting identified over $19 billion in identified waste, fraud, and savings opportunities. These numbers reflect what industrialized federal pattern recognition produces at scale. The government is not investigating providers one at a time. It is running analytics across the entire medicare billing universe and surfacing statistical outliers for further review.
For providers, that changes what compliance means. Compliance in 2026 is not just about following the rules. It is about understanding how your billing patterns look to a system designed to detect anomalies, and whether your documentation can explain any outlier patterns that exist.
What Happens When the Strike Force Gets Involved
 Many providers don’t realize how quickly the situation can escalate once a practice enters the enforcement process. The sequence moves faster than most people expect.
Many providers don’t realize how quickly the situation can escalate once a practice enters the enforcement process. The sequence moves faster than most people expect.
Federal interest begins with algorithmic identification. An analyst reviews the flagged provider’s billing data in more detail. If the pattern holds up under manual review, an investigation opens. The provider typically doesn’t know any of this is happening. At some point, OIG refers the matter to CMS for payment intervention. That’s when practices first learn they have a problem, often through a letter notifying them that reimbursements are being suspended or billing privileges are under review.
At that stage, the practice is already managing a financial crisis and a legal exposure simultaneously. Responding effectively requires healthcare attorneys, compliance specialists, and billing documentation that can explain every pattern the government has flagged. Practices that haven’t maintained clean, consistent, well-documented billing records are in a far more difficult position than those that have.
The cost of getting to that point, even if the practice ultimately demonstrates that no fraud occurred, is significant in terms of time, legal fees, revenue interruption, and reputational impact.
What Practices Should Be Doing Right Now
The practical implication of all of this is straightforward. Every Medicare-participating provider needs an internal billing surveillance process that mirrors, to the extent possible, how the Strike Force looks at claims data. Not annual coding education. Not occasional chart audits. A real, recurring process that asks hard questions about billing patterns before the government asks them first.
That process should be looking at specific questions on a regular basis:
- Which CPT code families are growing faster than patient volume or case mix would predict?
- Which providers in the group are billing outside specialty norms relative to published benchmarks?
- Which diagnosis combinations are consistently supporting higher reimbursement, and is the documentation clearly supporting them?
- Where do modifier patterns exceed peer averages, and can those patterns be explained by documented clinical circumstances?
- Are RPM, CCM, and telehealth encounters fully documented with evidence of actual patient engagement?
- Are wound care, DME, infusion, behavioral health, or home visit revenues rising faster than the medical necessity documentation supports?
These are exactly the questions federal analysts are asking about your practice right now. The difference between identifying an issue internally and having the government identify it for you is enormous, both in terms of the outcome and in terms of the options available to address it.
Proactive internal review, clean documentation practices, and a billing operation that prioritizes accuracy over aggressive utilization maximization are the most effective compliance tools available. They’re also the most effective protection against becoming an anomaly in a federal dataset.
Medicare Fraud Strike Force FAQ
- What is the Medicare Fraud Strike Force?
The Medicare Fraud Strike Force is a joint federal initiative involving the HHS Office of Inspector General, the Department of Justice, the FBI, and CMS, among other agencies. It was created in 2007 to concentrate federal enforcement resources in the highest-risk Medicare billing markets. In 2026, it operates as a data-driven surveillance and prosecution program that analyzes billing patterns across multiple federal programs simultaneously to identify providers whose reimbursement activity is statistically inconsistent with peer norms. - Can a legitimate provider be investigated by the Strike Force?
Yes. The Strike Force process begins with billing pattern analysis, not with an assessment of intent. A legitimate practice with unusual billing patterns, whether caused by aggressive coding practices, template-driven documentation, or billing team strategies that maximize utilization without adequate clinical support, can trigger federal interest before any review of the underlying clinical circumstances. Intent becomes relevant after the investigation opens, not before it starts. - What billing patterns are most likely to attract Strike Force attention in 2026?
The current enforcement priorities include telehealth billing anomalies, DME and supply billing, wound care and skin substitute reimbursement, home health and hospice documentation patterns, and diagnosis upcoding in chronic condition management. Practices that show billing distributions significantly above specialty peer benchmarks in any of these areas are at elevated risk of algorithmic identification. - How can the Strike Force affect my practice before any charges are filed?
When the OIG deems allegations credible, CMS can suspend reimbursements, revoke billing privileges, require prepayment review, or freeze provider enrollment before any criminal charge is adjudicated. For many practices, that payment interruption is financially severe on its own, separate from any legal outcome. - What is the difference between a Strike Force investigation and a regular payer audit?
A standard payer audit typically reviews documentation for a specific set of claims submitted to that payer. The Strike Force looks across multiple federal programs simultaneously and uses predictive analytics to identify outlier patterns before investigating specific claims. The scope, the speed, and the consequences are all significantly greater than a standard audit. - What should a practice do if it receives a contact from OIG or CMS about its billing?
The first step is to engage a healthcare attorney with experience in federal fraud and abuse matters before responding to any government inquiry. Attempting to respond without legal guidance is a serious mistake. Simultaneously, the practice should gather complete billing records and documentation for the period in question and avoid destroying or altering any records. - How does clean billing protect a practice from Strike Force scrutiny?
Billing that accurately reflects the clinical work performed, supported by documentation that clearly explains the level of service, the medical necessity of procedures, and the clinical decision-making involved, produces a billing signature that is consistent with peer norms and resistant to algorithmic flagging. Clean billing doesn’t guarantee immunity from scrutiny, but it gives the practice a defensible position if questions are raised.
Providers also Ask
- How does the Strike Force decide which providers to investigate?
The process starts with federal claims analytics that compare a provider’s billing patterns against specialty, geographic, and demographic peer groups. Providers whose patterns show statistically significant deviations in utilization, reimbursement levels, diagnosis coding, or service combinations are flagged for manual review. If manual review confirms the anomaly, an investigation opens. The provider typically doesn’t know they’ve been flagged until well into that process. - What does “billing outside specialty norms” actually mean?
It means that a provider’s claims data, when compared against other providers in the same specialty, geographic area, and patient population category, shows patterns that are statistically improbable. Examples include E/M visit distributions heavily weighted toward the highest complexity levels without corresponding patient acuity data, procedure frequencies that far exceed specialty averages, or diagnosis combinations that consistently support higher reimbursement without clear clinical support in documentation. - Can a billing company or vendor create fraud risk for a practice?
Yes. A third-party billing vendor that aggressively maximizes utilization without adequate documentation support can create billing patterns that attract federal scrutiny even when the treating physician had no awareness of the billing strategy being applied. The practice, not the vendor, holds the Medicare billing privileges and bears primary responsibility for claims submitted under its NPI. Practices should regularly review the billing patterns their vendors are producing and understand the strategy being applied on their behalf. - What is the fastest way to reduce Strike Force exposure for a medical practice?
Conducting an internal billing audit that benchmarks your CPT code distribution, modifier usage, and reimbursement patterns against specialty peers is the starting point. Identifying outlier patterns before the government does gives the practice the opportunity to address documentation gaps, retrain staff, or adjust billing protocols proactively. Practices that self-identify and self-correct are in a fundamentally different position than those that first learn about a problem through a government contact. - How does the No Surprises Act or prior authorization relate to Strike Force risk?
They are separate regulatory areas, but they interact in one important way. Billing patterns created by workarounds to prior authorization requirements or out-of-network reimbursement strategies can produce statistical anomalies in claims data that attract algorithmic attention. Practices that have developed billing strategies specifically designed to maximize reimbursement in ways that don’t clearly reflect the clinical activity delivered are at elevated risk regardless of the specific mechanism used.
Summary: Healthcare Providers are Now Practicing Under a Federal Data Radar
 At Medwave, we offer services in billing, credentialing, and payer contracting for medical practices across the country. We don’t function as a compliance firm or a legal defense resource, but we are deeply aware of how federal enforcement trends affect the practices we serve.
At Medwave, we offer services in billing, credentialing, and payer contracting for medical practices across the country. We don’t function as a compliance firm or a legal defense resource, but we are deeply aware of how federal enforcement trends affect the practices we serve.
The billing patterns the Strike Force is targeting are ones that often develop gradually, sometimes through third-party billing vendors pushing aggressive utilization strategies, sometimes through documentation shortcuts that accumulate over time, and sometimes through coding practices that were never revisited after they were first established. We work with practices to build billing operations that are both financially optimized and defensible under scrutiny.
Clean billing is not the same as conservative billing. It means billing accurately for the work performed, documenting that work clearly, and maintaining patterns that reflect the actual clinical activity of the practice. That approach produces strong revenue and a compliance posture that holds up when questions are asked.
If your practice is concerned about its billing patterns, your credentialing standing, or the terms of your payer contracts, we are glad to talk through what we’re seeing in the market and how we can help.
Co-Founder and COO of Medwave, bringing more than 30 years of hands-on experience in healthcare revenue cycle management, payer contracting, and medical credentialing.

