Physician compensation varies by specialty, geography, practice setting, and payer mix, but the ranking at the top of the earnings chart has been remarkably stable over the past five years. Certain specialties consistently outperform others not just because of clinical demand, but because of how their services are structured, reimbursed, and billed.

What the annual data reveals is a clear pattern. Procedure-heavy specialties dominate the top tier. High procedure volume means higher CPT code density per encounter, stronger leverage in payer contract negotiations, and greater sensitivity to billing accuracy. A coding error or a weak payer contract in orthopedics or cardiology costs more than the same mistake in a lower-volume specialty.
The five-year view below draws from Medscape’s annual Physician Compensation Reports and covers the ten specialties that have consistently ranked highest. The data is followed by analysis of what is driving the trends and what it means for revenue cycle management in each specialty.
TL;DR
- Orthopedic surgery has been the highest-paying physician specialty every year from 2021 through 2025, with average compensation rising from $511,000 to $611,000 over that period.
- Plastic surgery has held the number two spot in most years, with 2025 compensation averaging $554,000.
- Cardiology, radiology, anesthesiology, gastroenterology, and urology consistently rank in the top ten across all five years.
- Compensation growth across the top specialties has outpaced inflation in most years, but so has the administrative complexity of billing for those services.
- High-paying specialties tend to have the most to gain from strong billing, credentialing, and payer contracting support.
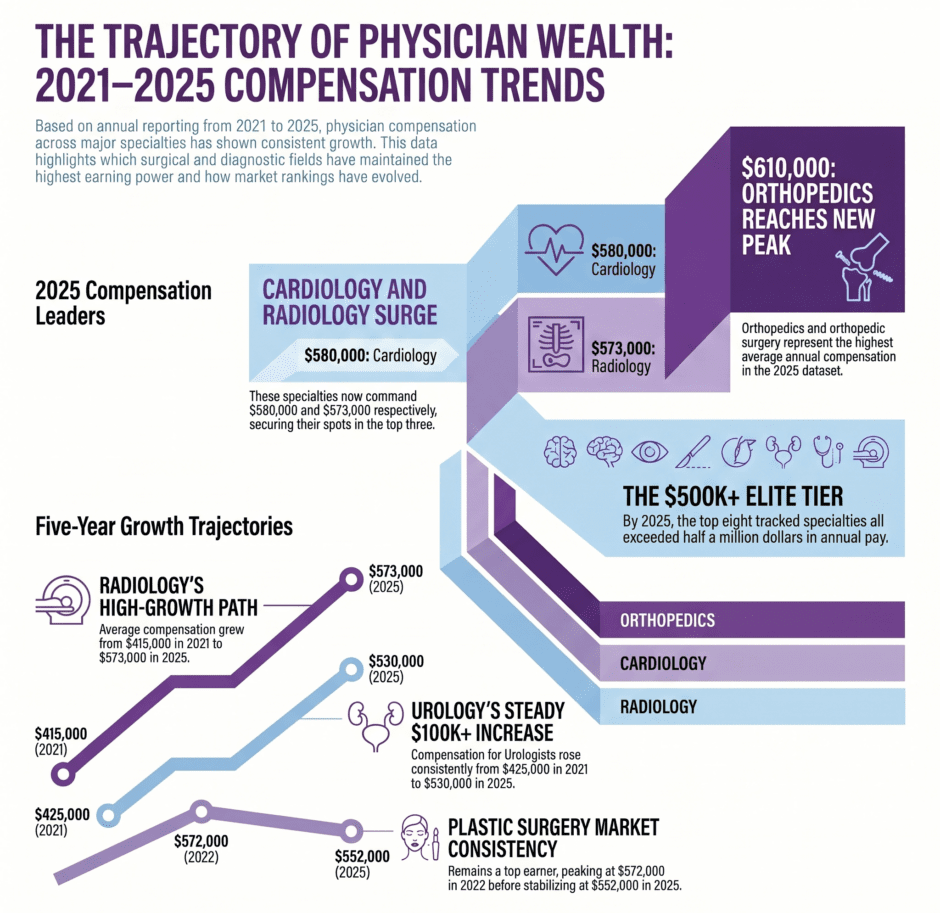
Five Years of Physician Compensation Data
Before getting into analysis, here’s the full picture from Medscape’s annual reporting across the five most recent years. The numbers represent average annual physician compensation by specialty.
2025
- Orthopedics and orthopedic surgery: $610,000
- Cardiology: $580,000
- Radiology: $573,000
- Plastic surgery: $552,000
- Anesthesiology: $541,000
- Urology: $530,000
- Gastroenterology: $532,000
- Otolaryngology: $510,000
- Oncology and hematology: $465,000
- Dermatology: $451,000
2024
- Orthopedics and orthopedic surgery: $540,000
- Radiology: $522,000
- Plastic surgery: $515,000
- Cardiology: $508,000
- Anesthesiology: $498,000
- Gastroenterology: $495,000
- Urology: $486,000
- Otolaryngology: $472,000
- Oncology and hematology: $451,000
- Dermatology: $423,000
2023
- Orthopedics and orthopedic surgery: $550,000
- Plastic surgery: $535,000
- Cardiology: $524,000
- Urology: $514,000
- Gastroenterology: $513,000
- Radiology: $497,000
- Dermatology: $478,000
- Anesthesiology: $471,000
- Oncology and hematology: $463,000
2022
- Plastic surgery: $572,000
- Orthopedics and orthopedic surgery: $556,000
- Cardiology: $489,000
- Otolaryngology: $468,000
- Urology: $460,000
- Gastroenterology: $452,000
- Dermatology: $437,000
- Radiology: $436,000
- Ophthalmology: $416,000
2021
- Plastic surgery: $525,000
- Orthopedics and orthopedic surgery: $510,000
- Cardiology: $458,000
- Urology: $425,000
- Otolaryngology: $416,000
- Radiology: $415,000
- Gastroenterology: $404,000
- Oncology: $402,000
- Dermatology: $393,000
- Ophthalmology: $377,000
Orthopedic Surgery: Five Years at the Top
 Orthopedic surgery is the clearest compensation story of the past five years. It held the top spot in 2021, dropped to second behind plastic surgery in 2022, and then reclaimed the number one position in 2023 and has stayed there through 2025. More significantly, orthopedic compensation has climbed from $510,000 in 2021 to $610,000 in 2025. That’s a $100,000 increase over five years, a roughly 20% gain that exceeds most other specialties in both absolute and percentage terms.
Orthopedic surgery is the clearest compensation story of the past five years. It held the top spot in 2021, dropped to second behind plastic surgery in 2022, and then reclaimed the number one position in 2023 and has stayed there through 2025. More significantly, orthopedic compensation has climbed from $510,000 in 2021 to $610,000 in 2025. That’s a $100,000 increase over five years, a roughly 20% gain that exceeds most other specialties in both absolute and percentage terms.
What’s driving that growth? Procedure volume and site of care are two big factors. Orthopedic surgery has seen a significant shift toward ambulatory surgery centers over the past several years, with total joint replacements leading that movement. ASCs typically generate stronger margins for physician-owned practices than hospital operating rooms, and as more procedures have moved to the outpatient setting, orthopedic compensation has reflected that shift. The coding and billing demands in orthopedics are substantial. Implant billing, modifier usage, and global period rules require specific expertise, and practices that manage those elements well protect a larger share of their generated revenue.
There’s also a straightforward supply and demand story. Orthopedic surgeons complete a demanding residency and frequently pursue fellowship training. The pipeline is long. Demand for orthopedic care has been rising as the population ages and as patients pursue active lifestyles later in life. That combination keeps compensation competitive.
Plastic Surgery: Consistently Near the Top
Plastic surgery actually held the number one spot in both 2021 and 2022, with compensation reaching $572,000 in 2022, the highest single-year figure for plastic surgery in that stretch. It dropped to second in 2023 and has held around that position since, with 2025 compensation at $552,000.
Plastic surgery has an unusual payer mix compared to other high-earning specialties. A meaningful share of plastic surgery revenue comes from elective, self-pay procedures, particularly cosmetic services. That self-pay component insulates plastic surgery practices from some of the payer contract pressures that affect other surgical specialties, but it also means those practices need strong patient collections processes and pricing structures that reflect the market.
For reconstructive procedures billed to insurance, plastic surgery has its own set of coding specifics around wound closure, flap reconstruction, and post-mastectomy work. Those services carry real reimbursement value and require documentation and coding practices that capture the full scope of work performed.
Cardiology: A Consistent Top-Three Performer
 Cardiology has ranked in the top three specialties every single year from 2021 through 2025, reaching $580,000 in 2025 after sitting at $458,000 in 2021. That’s a $122,000 increase over five years, making it one of the strongest compensation growth stories in the top ten.
Cardiology has ranked in the top three specialties every single year from 2021 through 2025, reaching $580,000 in 2025 after sitting at $458,000 in 2021. That’s a $122,000 increase over five years, making it one of the strongest compensation growth stories in the top ten.
The drivers here are familiar ones. An aging population means more patients with cardiovascular disease, more diagnostic workups, more interventional procedures, and more chronic disease management. Medicare is typically the dominant payer for cardiology practices, which means Medicare reimbursement rates, Medicare Advantage payer contracting, and CMS policy decisions all have an outsized effect on cardiology practice revenue compared to specialties with younger patient populations.
Cardiology has a wide range of service types, from office E/M visits and stress testing to cardiac catheterization, device implantation, and electrophysiology procedures. Each of those service categories has its own billing requirements, and practices that do interventional work have significant revenue tied to procedure coding accuracy. Prior authorization burden in cardiology is also substantial, particularly for imaging and high-cost interventional services.
Radiology: A Strong Rebound
Radiology’s compensation picture over the five-year period is one of the more interesting stories in the dataset. It ranked sixth in 2021 at $413,000, climbed significantly to second place in 2024 at $522,000, and held the third position in 2025 at $573,000. That trajectory reflects several factors, including the growth of teleradiology, the expansion of imaging volume, and AI-assisted reading workflows that have changed how radiologists operate.
Radiology billing is built on the professional and technical component distinction, and practices that own their imaging equipment or work in outpatient imaging centers have different revenue dynamics than hospital-employed radiologists who bill only the professional component. The billing infrastructure for radiology is specialized, and practices that manage both components need clear workflows to avoid the most common errors around component billing.
Anesthesiology: Stable and Strong
 Anesthesiology has appeared in the top five every year from 2021 through 2025, with compensation growing from the low $400,000 range historically to $541,000 in 2025. Anesthesiology billing is unlike any other specialty in medicine. It is built on base units and time units, billed in increments, and governed by rules that vary by payer and by whether the anesthesiologist is personally performing the case or medically directing CRNAs.
Anesthesiology has appeared in the top five every year from 2021 through 2025, with compensation growing from the low $400,000 range historically to $541,000 in 2025. Anesthesiology billing is unlike any other specialty in medicine. It is built on base units and time units, billed in increments, and governed by rules that vary by payer and by whether the anesthesiologist is personally performing the case or medically directing CRNAs.
The medical direction model, the personally performed modifier, and the concurrent procedure rules all affect how anesthesiology cases are billed and how much gets collected. Anesthesiology practices that don’t have specialty-specific billing support tend to leave more revenue uncollected per case than almost any other specialty, simply because the billing rules are so specific.
Gastroenterology and Urology: Reliable Earners
Gastroenterology and urology have both appeared in the top ten every year across the five-year period, with gastroenterology reaching $532,000 in 2025 and urology at $530,000. Both specialties benefit from high procedure volumes, strong diagnostic coding opportunities, and in the case of gastroenterology, a colonoscopy screening mandate that keeps patient demand steady.
Gastroenterology’s shift toward the ambulatory setting has had a similar effect on compensation as orthopedics. Practices that own ASC equity and perform endoscopy procedures in outpatient settings capture more of the facility margin than those working in hospital endoscopy suites. That structural difference in practice setting is often as important to overall compensation as the professional fee schedule itself.
Urology has benefited from the expansion of minimally invasive robotic procedures and from chronic disease management opportunities in areas like overactive bladder, BPH, and prostate cancer treatment. The coding requirements for robotic surgery and for implantable device procedures require specific expertise, and payer prior authorization requirements for many urologic procedures add to the administrative burden.
Dermatology and Otolaryngology: Consistent Presence
 Dermatology has appeared in the top ten every year of the five-year period, with compensation reaching $423,000 in 2024 and reaching $510,000 in 2025. The specialty benefits from a high volume of outpatient procedures, a mix of medical and cosmetic services, and strong demand across all age groups. Like plastic surgery, the self-pay component of dermatology practice, particularly for cosmetic services, provides revenue diversity that most insurance-dependent specialties don’t have.
Dermatology has appeared in the top ten every year of the five-year period, with compensation reaching $423,000 in 2024 and reaching $510,000 in 2025. The specialty benefits from a high volume of outpatient procedures, a mix of medical and cosmetic services, and strong demand across all age groups. Like plastic surgery, the self-pay component of dermatology practice, particularly for cosmetic services, provides revenue diversity that most insurance-dependent specialties don’t have.
Otolaryngology has appeared in the top ten in most years, reaching $508,000 in 2025. ENT practices span a wide range of service types from office E/M visits and allergy services to complex head and neck surgery, which creates both billing variety and the need for specialty-specific coding knowledge.
What the Five-Year Trend Tells Practices
The most important takeaway from five years of physician compensation data isn’t which specialty is at the top. It’s that compensation in the highest-earning specialties has grown significantly and consistently, and the practices that capture the most of that compensation potential are the ones with strong billing, credentialing, and payer contracting infrastructure behind their clinical operations.
Here are four factors that consistently affect how much of a specialty’s compensation potential actually reaches the physician:
- Payer contracting: Practices with fee schedules that haven’t been renegotiated in years are collecting less per service than their peers in the same specialty and market, regardless of what Medscape’s compensation data shows as an average
- Credentialing delays: A new provider in a high-earning specialty who spends 90 to 120 days in credentialing limbo before billing is a direct and measurable revenue loss for the practice
- Billing accuracy: Specialties with procedure-heavy billing, including orthopedics, anesthesiology, and gastroenterology, have the most to gain from coding accuracy and the most to lose from consistent errors
- Denial management: High-volume specialties generate high-volume denied claims, and practices that don’t have a structured appeals process absorb those losses rather than recovering them
The gap between a specialty’s average reported compensation and what an individual physician actually earns is often explained by these administrative factors. Strong clinical skills don’t guarantee strong collections. The billing infrastructure behind the practice does.
Highest-Paying Physician FAQ
- Which physician specialty has the highest compensation?
According to Medscape’s annual data, orthopedic surgery has been the highest-compensated physician specialty in most years from 2021 through 2025, reaching an average of $611,000 in 2025. Plastic surgery held the top position in 2021 and 2022 and has remained second or third in subsequent years. - How much has physician compensation grown over the last five years?
Growth has varied by specialty, but the overall trend across the top ten has been consistently upward. Orthopedic surgery grew from $510,000 in 2021 to $610,000 in 2025, a clean $100,000 gain over five years. Cardiology had one of the strongest runs in the dataset, climbing from $458,000 in 2021 to $580,000 in 2025, a $122,000 increase that pushed it from third place to second by 2025. Radiology tells a different kind of story: it sat at $415,000 in 2021, outside the top five, and worked its way up to $522,000 and second place overall by 2024 before settling at $573,000 and third in 2025. Plastic surgery remains one of the highest-earning specialties in the dataset despite slight year-over-year variation, holding between $515,000 and $572,000 across the five-year window. Every specialty in the top ten posted higher compensation in 2025 than it did in 2021, and in most cases the gains were substantial enough to meaningfully outpace inflation over the same period. - Does compensation data reflect what physicians actually take home?
The Medscape data reflects average reported physician compensation, which includes salary, bonuses, and profit sharing where applicable. What a physician actually collects depends heavily on practice type, payer mix, billing accuracy, and contract rates. Practices with strong billing and contracting support tend to outperform the average for their specialty, while practices with billing gaps or outdated contracts often fall below it. - Why do surgical specialties consistently earn more than primary care?
Procedural specialties generate higher per-encounter reimbursement than evaluation and management visits, which are the foundation of primary care billing. A surgical procedure billed at several thousand dollars produces more revenue per hour of physician work than an office visit billed at a few hundred dollars. That reimbursement structure, built into the CPT fee schedule, is the primary driver of the compensation gap between surgical and primary care specialties. - How does practice setting affect physician compensation?
Practice setting has a significant effect. Physicians who work in physician-owned ambulatory surgery centers often capture both the professional fee and a share of the facility revenue, which can substantially increase total compensation compared to hospital-employed physicians who receive only the professional fee. The shift of procedures from hospital to ASC settings has been a major factor in compensation growth for orthopedics, gastroenterology, and other procedural specialties over the past several years. - What role does payer contracting play in physician compensation?
Payer contracts set the rates at which the practice is reimbursed for services. A practice with fee schedules at 130% of Medicare is collecting meaningfully more per service than one at 105% of Medicare, even with identical patient volumes and clinical quality. Many practices, particularly those that have been operating for several years without reviewing their contracts, are collecting significantly less than their peers in the same specialty and market because their rates haven’t kept pace with market benchmarks.
Providers also Ask
- Why has orthopedic surgery compensation grown so much in the last five years?
Several factors have driven orthopedic compensation growth. The shift of total joint replacements and spine procedures to ambulatory surgery centers has expanded the revenue opportunity for physician-owned practices. Sustained demand from an aging population has kept procedure volumes high. Orthopedic billing, when managed correctly, captures significant revenue from implant coding, surgical assistant billing, and procedure-specific modifier usage that adds up across a high-volume surgical practice. - Is the compensation data the same for employed physicians and those in private practice?
Not necessarily. Medscape surveys both employed and self-employed physicians, and the compensation figures represent averages across both groups. Private practice physicians who own equity in surgical facilities or imaging centers often report higher total compensation than employed peers in the same specialty. Employed physicians may have more predictable income but typically don’t share in facility revenue. - What specialties are seeing the fastest compensation growth right now?
Based on the five-year dataset, cardiology and radiology have shown some of the strongest growth trajectories in recent years. Cardiology grew by over $100,000 in average compensation from 2021 to 2025. Radiology climbed from sixth place to second place in the rankings between 2021 and 2024. Orthopedics has shown the most sustained growth in absolute dollar terms over the full five-year period. - How does billing accuracy affect a practice’s actual compensation?
Billing accuracy determines how much of the revenue a physician generates actually gets collected. Undercoded visits, missed procedure codes, denied claims that go unappealed, and outdated payer contracts all reduce collections relative to what the practice should be earning. In high-volume surgical specialties, even small per-encounter billing errors multiply across thousands of annual cases into significant annual revenue gaps. The practices that perform best financially in high-earning specialties are almost always the ones with the tightest billing operations. - Should high-earning specialty practices manage billing in-house or outsource it?
Both models can work, but specialty-specific billing knowledge is the critical variable. A general billing team managing orthopedic or anesthesiology billing without deep specialty expertise will typically underperform a billing partner with specific experience in those code sets. The more procedure-intensive the specialty, the more valuable specialty-specific billing expertise becomes, because the revenue per correctly coded claim is high and the cost of consistent errors compounds quickly across a large claim volume.
Summary: 10 Highest-Paying Physician Specialties
 The specialties that consistently rank at the top of the physician compensation charts are also the ones where administrative execution matters most, because the revenue opportunity is largest and the cost of getting it wrong is highest.
The specialties that consistently rank at the top of the physician compensation charts are also the ones where administrative execution matters most, because the revenue opportunity is largest and the cost of getting it wrong is highest.
An orthopedic group leaving implant billing on the table, a cardiology practice with Medicare Advantage contracts that haven’t been reviewed in three years, or an anesthesia practice where medical direction billing isn’t being applied correctly are all losing meaningful revenue every month. Those aren’t problems that fix themselves.
If your practice is in one of these high-earning specialties and you’re not certain your billing, credentialing, and payer contracting are as strong as your clinical reputation, it’s worth exploring our services.
COO and Co-Founder of Medwave, with over 30 years of experience in healthcare revenue cycle management, payer contracting, and medical credentialing.

