
Neurology is one of the most documentation-intensive specialties in medicine. Every visit, every procedure, and every consultation requires a level of clinical specificity in the chart that directly determines how much the practice gets paid. When that documentation is strong, billing works. When it isn’t, revenue leaks out through undercoded visits, denied claims, and procedures that should have been billed separately but weren’t.
 The stakes are high. A neurology practice managing a full schedule of outpatient visits, inpatient consultations, EEGs, EMGs, and infusion services is operating across multiple distinct code sets simultaneously. Each one has its own documentation rules, its own payer coverage policies, and its own audit risk profile. A general billing team without neurology-specific experience tends to underperform across most of them.
The stakes are high. A neurology practice managing a full schedule of outpatient visits, inpatient consultations, EEGs, EMGs, and infusion services is operating across multiple distinct code sets simultaneously. Each one has its own documentation rules, its own payer coverage policies, and its own audit risk profile. A general billing team without neurology-specific experience tends to underperform across most of them.
Add credentialing timelines that can stretch to four months or more, payer contracts that haven’t been renegotiated in years, and a prior authorization burden that consumes significant staff time every week, and you have an administrative environment that demands focused, specialty-trained support.
We cover what neurology billing involves, which CPT codes matter most and where errors occur, what the credentialing process looks like for neurologists, how payer contracting works in this specialty, and what denial management requires. At Medwave, we help neurology practices across the country, and everything here reflects what actually makes a difference.
TL;DR
- Neurology billing spans multiple service types including outpatient E/M visits, EEG, EMG, infusion therapy, and inpatient consultations, each with its own coding and documentation requirements.
- E/M level selection under the 2021 AMA guidelines is driven by medical decision-making or total time, and many neurology practices are still undercoding because their documentation protocols haven’t been updated.
- Neurologist credentialing involves both hospital privileging and payer enrollment, with timelines typically running 60 to 120 days or longer depending on the institution and payer.
- Payer contracting in neurology is an area where many practices are significantly underpaid, often because contracts haven’t been reviewed since they were first signed.
- Prior authorization is a major operational burden for neurology practices managing infusion patients and patients on high-cost disease-modifying therapies.
- Medwave provides billing, credentialing, and payer contracting services for neurology practices and groups nationwide.
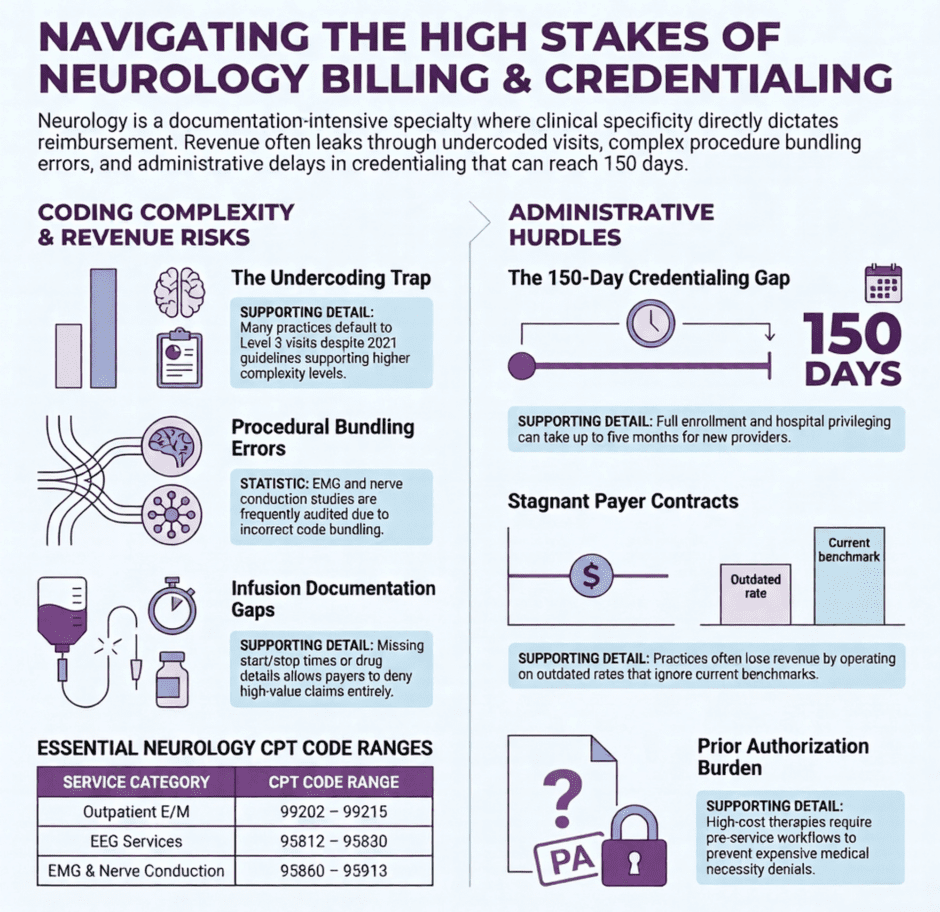
What Makes Neurology Billing Different
 Neurology is not a single-service specialty. On any given day, a neurologist might see an outpatient with epilepsy, perform and interpret an EEG, consult on a hospitalized stroke patient, supervise an infusion for a multiple sclerosis patient, and review nerve conduction study results. Each of those services is billed differently, documented differently, and covered differently by payers. That variety is what makes neurology billing both demanding and, when handled correctly, a strong revenue generator.
Neurology is not a single-service specialty. On any given day, a neurologist might see an outpatient with epilepsy, perform and interpret an EEG, consult on a hospitalized stroke patient, supervise an infusion for a multiple sclerosis patient, and review nerve conduction study results. Each of those services is billed differently, documented differently, and covered differently by payers. That variety is what makes neurology billing both demanding and, when handled correctly, a strong revenue generator.
The 2021 AMA changes to outpatient E/M documentation guidelines were a significant shift for neurology. Level selection moved away from counting elements in the history and physical exam and toward medical decision-making or total time as the two valid pathways. For neurologists who routinely manage high-complexity chronic conditions, those changes should have moved their billing distribution toward higher E/M levels. Practices that didn’t update their documentation protocols after 2021 are likely still billing at levels that don’t reflect the clinical work being done.
Beyond E/M visits, the procedure side of neurology billing adds another layer of specificity. EEG coding requires distinguishing between routine, prolonged, and ambulatory studies and between the professional and technical components of the service. EMG and nerve conduction study codes have bundling rules that are actively audited by payers. Infusion therapy requires documentation of start and stop times, drug administration details, and nursing supervision. Missing any of those details doesn’t just reduce revenue on individual claims. It creates a pattern that attracts payer scrutiny.
Neurology CPT Codes: What Every Practice Needs to Know
Outpatient E/M Codes
Outpatient E/M visits in neurology are billed under CPT codes 99202 through 99215, with new patient visits running from 99202 to 99205 and established patient visits from 99211 to 99215. Level selection should be driven by either medical decision-making or total physician time, whichever supports the higher level for the encounter.
Neurology visits are frequently high-complexity encounters. Patients managing epilepsy, Parkinson’s disease, multiple sclerosis, or dementia often present with multiple active problems, require review of extensive data, and involve treatment decisions that carry meaningful risk. Those encounters routinely support level 4 or level 5 billing. Practices that show a billing distribution weighted heavily toward level 3 visits should take a hard look at whether their documentation is capturing what’s actually happening in the exam room.
Inpatient Consultations and Hospital E/M Codes
Medicare eliminated inpatient consultation codes 99241 through 99255 for Medicare patients years ago. Many neurology practices still handle this incorrectly. When a neurologist is called to consult on a hospitalized Medicare patient, the appropriate codes are the initial hospital care codes (99221 through 99223) for the first visit and subsequent hospital care codes (99231 through 99233) for follow-up visits. Billing under the old consultation code set for Medicare patients results in denials that are entirely avoidable.
For commercial payers that still recognize consultation codes, the rules are different, and the billing approach needs to reflect that distinction by payer.
EEG Codes
EEG codes run from 95812 through 95830 and cover a range of study types from routine to prolonged to ambulatory monitoring. The code selected must match the type of study performed and the duration of the recording. Many EEG services have separate professional and technical components, and billing both under the same provider when the technical component is actually performed by the facility is a billing error that creates both denial and compliance risk.
EEG interpretation reports must stand alone as clinical documents that clearly describe the study findings, the technical quality of the recording, and the clinical interpretation. A report that is vague, templated, or lacking specific findings doesn’t support the professional component billed.
EMG and Nerve Conduction Study Codes
EMG and nerve conduction studies are billed under CPT codes 95860 through 95913. This is one of the most audited areas in neurology billing, and for good reason. The codes have specific bundling rules, and the combination of EMG and NCS codes billed on the same date must reflect what was actually performed and documented in the study report. Unbundling codes that should be bundled, or billing bilateral studies incorrectly, are two of the most common errors in this code range.
Infusion Therapy Codes
Infusion therapy for neurological conditions is billed under CPT codes 96360 through 96379. The specific code depends on the type of infusion, whether it’s the initial or a subsequent hour of infusion, and whether additional drugs were administered. Documentation must include the start and stop time of the infusion, the drug administered, the dose, and the clinical supervision provided. Missing any of these elements gives the payer grounds to deny the claim regardless of whether the service was medically necessary and properly performed.
Neurology Documentation: Why It Determines Revenue
 Documentation quality in neurology is not just a compliance issue. It is a direct revenue driver. The E/M level that can be supported, the procedure codes that can be billed, and the medical necessity arguments that can be made in an appeal all depend on what is written in the chart.
Documentation quality in neurology is not just a compliance issue. It is a direct revenue driver. The E/M level that can be supported, the procedure codes that can be billed, and the medical necessity arguments that can be made in an appeal all depend on what is written in the chart.
Strong outpatient neurology documentation includes a clearly described presenting problem, a focused neurological examination with specific findings documented by system, and medical decision-making that addresses the number and nature of problems being managed, the data reviewed, and the risk associated with the treatment plan. Vague findings, generic exam templates, and decision-making sections that don’t reflect the actual clinical reasoning of the visit are the most common documentation failures in neurology.
Templated and copy-forward documentation is one of the most persistent problems in neurology practices that use EHR systems. A note that looks identical to the previous three visits for the same patient is an audit flag and often fails to support the E/M level billed because it doesn’t reflect new clinical decision-making. Training physicians to update documentation meaningfully at every visit is one of the highest-return investments a neurology practice can make in its billing performance.
Neurology Credentialing: The Full Process
Credentialing a neurologist involves meeting baseline professional requirements, going through hospital medical staff privileging where applicable, and completing payer enrollment for each payer the practice bills. All three have independent timelines and documentation requirements.
The baseline credentials for a neurologist include completion of a neurology residency, board certification through the American Board of Psychiatry and Neurology, active state medical licensure in every state where the provider practices, and DEA registration where prescribing is involved. Subspecialty fellowship training in areas like epilepsy, movement disorders, neurocritical care, or vascular neurology adds credentials that some hospital systems and payers require for specific privileges or service types.
Hospital privileging for neurologists who provide inpatient consultations follows the standard medical staff process: application, primary source verification of education, training, board certification, and licensure, peer references, department review, medical executive committee approval, and board sign-off. Most facilities complete this in 60 to 120 days. Some run longer. A neurologist sitting in credentialing limbo for three months is not generating revenue, and that cost is real and measurable.
Payer enrollment runs in parallel with hospital credentialing but is a separate administrative track. CAQH ProView handles much of the commercial payer data collection, but each payer has its own enrollment application and timeline. Medicare enrollment through PECOS typically takes 60 to 90 days. Some commercial payers move faster. Medicaid enrollment timelines vary significantly by state, which is relevant for neurology practices with pediatric or underserved patient populations.
Recredentialing is a recurring cycle that most practices underestimate until something lapses. Medical licenses, DEA registrations, board certifications, and payer enrollment statuses all have expiration dates. Missing a renewal creates gaps that can suspend billing privileges, disqualify claims, or trigger removal from a payer network. Proactive tracking with reminders built well ahead of deadlines is the only reliable way to prevent that.
Payer Contracting for Neurology Practices
 Payer contracting is where a significant amount of neurology revenue is either protected or lost, and most practices don’t pay enough attention to it. Many neurology groups are operating under contracts that were signed when the practice first opened and haven’t been reviewed since. Rates that were reasonable five years ago may now be well below market benchmarks, and the practice is absorbing that difference as a permanent revenue reduction.
Payer contracting is where a significant amount of neurology revenue is either protected or lost, and most practices don’t pay enough attention to it. Many neurology groups are operating under contracts that were signed when the practice first opened and haven’t been reviewed since. Rates that were reasonable five years ago may now be well below market benchmarks, and the practice is absorbing that difference as a permanent revenue reduction.
Most neurology fee schedules are structured as a percentage of Medicare rates. Knowing where your contracts land relative to that benchmark is the starting point for any contract evaluation. A contract at 105% of Medicare is a very different financial situation from one at 150% of Medicare, and practices that don’t know which one they have can’t make informed decisions about which payers to prioritize, renegotiate, or push back on.
Here are four specific contracting areas that neurology practices should review closely:
- EEG and EMG professional and technical component rates, which vary widely by payer and are frequently underpaid relative to the resources required
- Infusion therapy reimbursement rates, which are among the most variable in neurology and worth specific attention during any contract negotiation
- Inpatient consultation rates under Medicare Advantage plans, where reimbursement policies often differ from traditional Medicare in ways that disadvantage providers
- Telehealth neurology rates, which have expanded significantly and should now be a standard item in any commercial payer contract discussion
Contract language review matters as much as rate review. Coverage policies for specific neurology services, prior authorization requirements, timely filing deadlines, and dispute resolution provisions all affect how the contract actually functions in practice. A contract with strong rates but aggressive prior authorization requirements can still underperform if the practice doesn’t have the bandwidth to manage authorizations effectively.
Common Neurology Billing Errors That Cost Practices Money
Most revenue leaks in neurology billing come from a predictable set of recurring errors. Identifying and fixing them doesn’t require new technology. It requires consistent attention to coding accuracy and documentation quality.
- Undercoding outpatient E/M visits by defaulting to level 3 when the documentation supports level 4 or level 5, which is one of the most consistent and most significant revenue leaks in neurology practices
- Billing Medicare inpatient consultations under the old consultation code set rather than the appropriate initial hospital care codes, resulting in denials that are entirely preventable
- Miscoding EEG services by failing to distinguish between study types, billing the wrong duration code, or incorrectly splitting professional and technical components
- Unbundling or incorrectly bundling EMG and nerve conduction study codes in ways that trigger payer edits and denials
- Missing infusion documentation requirements, particularly start and stop times, which invalidates claims regardless of whether the service was clinically appropriate
- Failing to apply modifier 25 when a procedure is performed on the same day as an E/M visit, which results in the procedural revenue being denied as a duplicate
- Using templated or copy-forward documentation that doesn’t support the E/M level billed and creates audit exposure over time
- Missing prior authorization requirements for infusion therapy, advanced imaging, and certain EEG types, generating avoidable denials on high-value services
Denial Management in Neurology
 Denial rates in neurology tend to run higher than the overall specialty average. The documentation intensity, the prior authorization burden, and the procedure-specific coding requirements all create more opportunities for something to go wrong between the service and the payment.
Denial rates in neurology tend to run higher than the overall specialty average. The documentation intensity, the prior authorization burden, and the procedure-specific coding requirements all create more opportunities for something to go wrong between the service and the payment.
Medical necessity denials are the most common challenge in outpatient neurology billing. They happen most often on high-level E/M visits where the documentation doesn’t clearly support the complexity billed. A well-written clinical note that articulates the medical decision-making process, the number and nature of problems managed, and the risk of the treatment plan is the foundation of a winning medical necessity appeal. A vague or templated note gives the payer little reason to reverse the denial.
Prior authorization denials for infusion therapy and high-cost disease-modifying therapies are a significant operational issue for neurology practices managing MS patients and others on specialty medications. These denials require a different response process than standard claim denials, often involving peer-to-peer reviews between the treating neurologist and the payer’s medical director. Tracking prior authorization requirements by payer and by drug, and building a workflow that catches missing authorizations before services are rendered, prevents most of these denials before they happen.
Tracking denial patterns by payer and by denial code is how a practice distinguishes between a systemic problem and an isolated error. A spike in bundling denials from a specific payer may reflect a policy change that requires a billing adjustment. A pattern of medical necessity denials across all payers may reflect a documentation problem that needs to be addressed at the physician level. Without tracking, there’s no way to tell the difference.
Telehealth Billing in Neurology
Telehealth has become a meaningful part of neurology practice, particularly for follow-up visits, medication management consultations, and patients whose conditions limit their mobility or who live far from specialty care. The coding and documentation requirements for telehealth neurology visits follow the same E/M framework as in-person visits, with the addition of appropriate place of service codes and telehealth modifiers.
Payer coverage for telehealth neurology visits varies by payer and by state. Federal telehealth expansions put in place during the public health emergency have been extended in various forms, but commercial payer policies are not uniform. Practices operating in multiple states need to track coverage rules at both the federal and state level, since telehealth parity laws vary significantly across jurisdictions.
Payer contracting for telehealth is an active negotiating area. Some payers reimburse telehealth visits at parity with in-person rates. Others don’t, even in states where parity is technically required. Neurology practices that haven’t specifically addressed telehealth rates in their payer contracts may be getting underpaid on a growing share of their visit volume.
Neurology Billing, Credentialing FAQ
- How long does neurology credentialing take?
The full credentialing process for a neurologist, including hospital privileging and payer enrollment, typically takes 90 to 150 days. Hospital privileging alone runs 60 to 120 days at most institutions. Payer enrollment timelines vary: Medicare generally takes 60 to 90 days, and commercial payers range from 30 to 90 days or longer. Running both processes in parallel rather than sequentially is the most effective way to shorten the total time to billing. - What CPT codes are most commonly used in neurology billing?
The most frequently used code sets in neurology include outpatient E/M codes 99202 through 99215, EEG codes 95812 through 95830, EMG and nerve conduction study codes 95860 through 95913, and infusion therapy codes 96360 through 96379. Inpatient initial and subsequent hospital care codes apply for neurologists providing hospital-based consultations. - Does Medicare cover neurology consultations?
Medicare eliminated inpatient consultation codes for Medicare patients. Neurologists providing inpatient consultations for Medicare beneficiaries should bill under the initial hospital care codes (99221 through 99223) for the first visit and subsequent hospital care codes (99231 through 99233) for follow-up visits. Billing under the old consultation code set results in denials. Commercial payers vary, and some still recognize consultation codes under different rules. - How are EEG professional and technical components billed?
When a neurologist both performs and interprets an EEG in their own facility, the global code can be billed. When the technical component is performed by a hospital or separate facility and the neurologist only provides the professional interpretation, modifier 26 should be applied to bill only the professional component. Billing the global code when the technical component belongs to the facility is a billing error that creates both denial and compliance exposure. - How does prior authorization work for neurology infusion services?
Most commercial payers and Medicare Advantage plans require prior authorization for infusion therapy, particularly for high-cost disease-modifying therapies used in MS and other neurological conditions. The authorization must be obtained before the infusion is administered. A denial for missing prior authorization on a high-cost infusion service is one of the most expensive billing errors a neurology practice can make, and it’s almost entirely preventable with a clear pre-service authorization workflow. - Should neurology practices outsource their billing?
For most neurology practices, partnering with a billing service that has specific neurology experience produces better financial results than managing billing internally with a general billing team. The coding specificity required across EEG, EMG, infusion therapy, and E/M services, combined with the denial management and prior authorization demands, is more than most in-house general billing teams are equipped to handle consistently. - What is the most common reason neurology claims get denied?
Medical necessity denials for high-level E/M visits are the most common denial type in outpatient neurology. These occur when the documentation doesn’t clearly support the complexity of the visit billed. Prior authorization denials for infusion therapy and bundling-related denials for EMG and NCS claims are also among the most frequent denial categories in this specialty.
Neurologists also Ask
- What is the difference between a neurology consultation and an E/M visit for billing purposes?
A consultation is a service requested by another physician to evaluate a patient for a specific problem or question. An E/M visit is a service provided by the patient’s treating physician. For Medicare, the distinction no longer affects the coding since consultation codes were eliminated, but for commercial payers that still recognize consultation codes, the requesting physician’s documented referral and the consulting physician’s report back to the requesting provider are both required to support a consultation code. - How do neurology practices get paid for infusion therapy services?
Infusion therapy is billed using the infusion therapy CPT codes under 96360 through 96379, with the specific code depending on the drug type, infusion duration, and whether additional drugs were administered during the session. Payment depends on prior authorization being in place, documentation meeting the payer’s requirements, and the drug being covered under the patient’s pharmacy or medical benefit, depending on the payer’s policy. - Can a neurologist bill for both an EMG and a nerve conduction study on the same day?
Yes, under the right circumstances. EMG and NCS are separate services that can be billed together when both were performed and documented during the same encounter. However, the specific codes billed must reflect exactly what was performed, and the combination must comply with payer-specific bundling rules. This is one of the most audited billing areas in neurology, and the study report must clearly document all components performed to support both services. - What happens when a neurology practice adds a new subspecialist who needs to be credentialed and enrolled?
The new provider needs to go through both hospital privileging, if they will be providing inpatient services, and payer enrollment across all active payers in the practice. Both processes should start as early as possible, ideally before the provider’s start date. During the enrollment period, some practices use locum tenens billing arrangements as a bridge, though those arrangements have specific rules that vary by payer. Revenue generated before enrollment is complete typically cannot be billed retroactively, so minimizing the gap between start date and enrollment completion directly affects how quickly the new provider contributes to practice revenue. - How should neurology practices handle prior authorization denials for MS infusion therapy?
The most effective first step is a peer-to-peer review between the treating neurologist and the payer’s medical director. This gives the neurologist the opportunity to explain the clinical rationale directly and often produces a reversal faster than a written appeal alone. If the peer-to-peer review doesn’t resolve the denial, a formal written appeal with detailed clinical documentation, including the patient’s diagnosis, prior treatment history, and the specific reasons the requested therapy is medically necessary, is the next step. Tracking these denials by payer and building a library of successful appeal language for specific therapies improves outcomes over time.
Summary: Billing, Credentialing in Neurology
 Neurology is a specialty where the difference between good billing and average billing shows up clearly in the revenue numbers. The code sets are specific, the documentation requirements are demanding, the credentialing timelines are long, and the prior authorization burden is real. Managing all of that well requires people who know neurology billing, not just medical billing in general.
Neurology is a specialty where the difference between good billing and average billing shows up clearly in the revenue numbers. The code sets are specific, the documentation requirements are demanding, the credentialing timelines are long, and the prior authorization burden is real. Managing all of that well requires people who know neurology billing, not just medical billing in general.
Practices that are consistently undercoding, carrying high denial rates, or working with contracts that haven’t been reviewed in years are losing money that belongs to them. The good news is that most of these problems are fixable with the right support in place.
At Medwave, we support neurology practices in billing, credentialing, and payer contracting. We work with practices on provider enrollment across all active payers, denial management and appeals, prior authorization support, credentialing maintenance, and payer contract review and renegotiation. We bring neurology-specific knowledge to every engagement, which makes a measurable difference in how practices perform financially. If your practice is ready to stop leaving revenue on the table, contact us.
