
Hospital medicine is one of the fastest-growing specialties in American healthcare. Hospitalists manage the full arc of inpatient care, from the moment a patient is admitted through the day they leave, often juggling multiple active diagnoses, shifting acuity levels, and care coordination demands that change by the hour across an entire patient panel. That clinical intensity is what makes hospital medicine indispensable to how inpatient facilities function. It’s what makes hospital medicine billing genuinely difficult to do well.
The CPT codes used in hospital medicine span initial hospital care, subsequent inpatient visits, discharge management, critical care, observation services, and bedside procedures. Each of those categories has its own coding logic, documentation requirements, and payer rules that do not always align with how clinical care actually gets documented. Layer on the 2023 inpatient E/M guideline updates, time-based critical care rules, and the compliance exposure around level of care assignment, and you end up with a billing environment where gaps in documentation translate quickly and quietly into lost revenue.
Below, we cover how hospital medicine billing works across the major service categories, what credentialing looks like for hospitalists, where compliance risk tends to concentrate, and what your group can do to get claims right the first time.
TL;DR:
- Hospital medicine billing is built around inpatient E/M codes, critical care time, and discharge management services
- Documentation and medical decision making rules governing these services were significantly updated in 2023
- Correct level selection, accurate time capture for critical care, and airtight discharge documentation are where most groups either protect or lose revenue
- Credentialing for hospitalists runs through the American Board of Internal Medicine or the American Board of Family Medicine
- Credentialing requires primary source verification of training, licensure, hospital privileges, and malpractice history
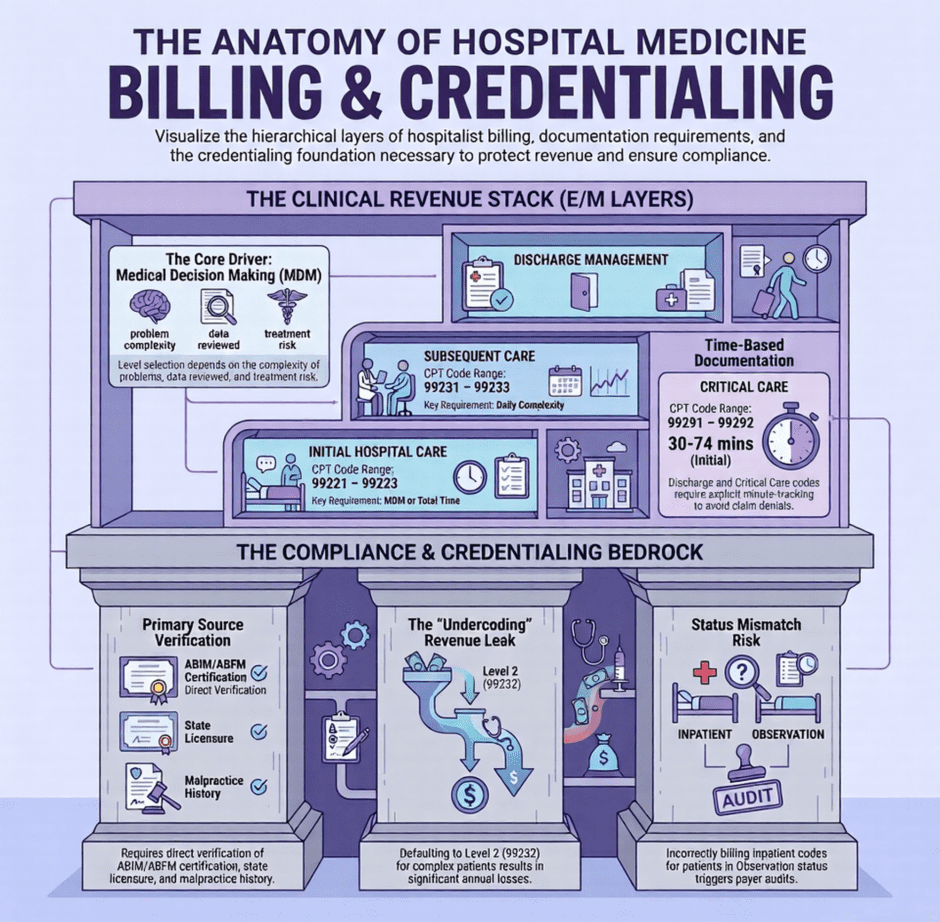
What Differentiates Hospital Medicine Billing?
 Most outpatient specialties operate on a fairly predictable billing rhythm. A patient comes in, a visit happens, a claim goes out. Hospital medicine does not work that way. Hospitalists bill for services that span multiple days, involve rotating coverage across large patient panels, and require documentation that captures not just what was done but the full weight of clinical decision making behind it.
Most outpatient specialties operate on a fairly predictable billing rhythm. A patient comes in, a visit happens, a claim goes out. Hospital medicine does not work that way. Hospitalists bill for services that span multiple days, involve rotating coverage across large patient panels, and require documentation that captures not just what was done but the full weight of clinical decision making behind it.
A hospitalist might see fifteen patients before noon. Some are straightforward. Others involve reviewing extensive records, coordinating with specialists, adjusting complex medication regimens, and having difficult conversations with families about goals of care. All of that work has to be reflected in the documentation for the billing to hold up. If the chart note does not capture the medical decision making, the claim gets coded at a lower level than the care actually warranted, and revenue disappears without anyone noticing.
The other thing that sets hospital medicine apart is the sheer volume of daily claims. Small per-encounter coding errors multiply quickly across a large group. A pattern of undercoding subsequent care visits by even one level across a hundred encounters per day is a significant annual revenue loss, and it often goes undetected for months.
Initial Hospital Care: Getting the Admission Right
Initial hospital care codes, CPT 99221 through 99223, cover the first inpatient encounter with a patient on the day of admission. These are among the highest-value codes hospitalists bill, and they are also among the most frequently miscoded.
Level selection for initial hospital care is based on medical decision making or total time spent. CPT 99221 covers straightforward medical decision making. CPT 99222 covers moderate complexity. CPT 99223, the highest level, requires high complexity medical decision making or significant time. For most hospital admissions, the clinical picture supports a 99222 or 99223, but the documentation has to actually reflect that.
The admission note needs to capture the presenting problem, the relevant history, the findings on examination, data reviewed including labs and imaging, and most importantly, the decision making that went into the plan. A note that says “patient admitted for pneumonia, started on antibiotics” does not support a level 3 admission code even if the clinical work involved was substantial. The documentation has to tell the full story.
One common error is billing an initial hospital care code and a subsequent care code on the same day for the same patient. If the admitting physician sees the patient more than once on the day of admission, only the initial hospital care code is reported. The second visit is not separately billable on that date.
Subsequent Hospital Care: Where Most Revenue Lives

Subsequent inpatient care codes, CPT 99231 through 99233, are the codes hospitalists bill every day for every patient they follow after the admission note. This is where the bulk of hospital medicine revenue comes from, and it is where undercoding tends to be most persistent.
CPT 99231 covers straightforward medical decision making, typically a stable patient with no significant changes. CPT 99232 covers moderate complexity, a patient whose condition is being actively managed, whose medication is being adjusted, or whose clinical picture requires interpretation of new data. CPT 99233 covers high complexity, a patient who is critically ill or whose condition is substantially worsening and requires intensive management.
Many hospitalists default to 99232 as a habit, regardless of what the clinical picture actually supports. For patients who genuinely warrant 99233, that undercoding is real money left behind on every encounter. The fix is straightforward. Document the data reviewed, the problems being managed, and the specific decision making driving the plan. When the note reflects the actual work, the code selection follows naturally.
A few practical things that affect subsequent care billing:
- Only one subsequent care code is reported per patient per day, regardless of how many times the hospitalist sees the patient. Multiple visits to the same inpatient on the same calendar day are combined into a single claim.
- When multiple physicians from the same group practice see the same patient on the same day, only one subsequent care code is billable for the group. Coverage arrangements need to account for this in how they track and document daily encounters.
- Time-based billing for subsequent care became a legitimate option under the 2023 guidelines. If the total time spent on that patient’s care on that date, including documentation time, is used to select the level, it must be clearly documented in the note.
- A hospitalist who performs a bedside procedure on the same day as a subsequent care visit can bill the procedure separately, provided the note supports a separately identifiable E/M service and the documentation reflects decision making beyond the pre-service work for the procedure.
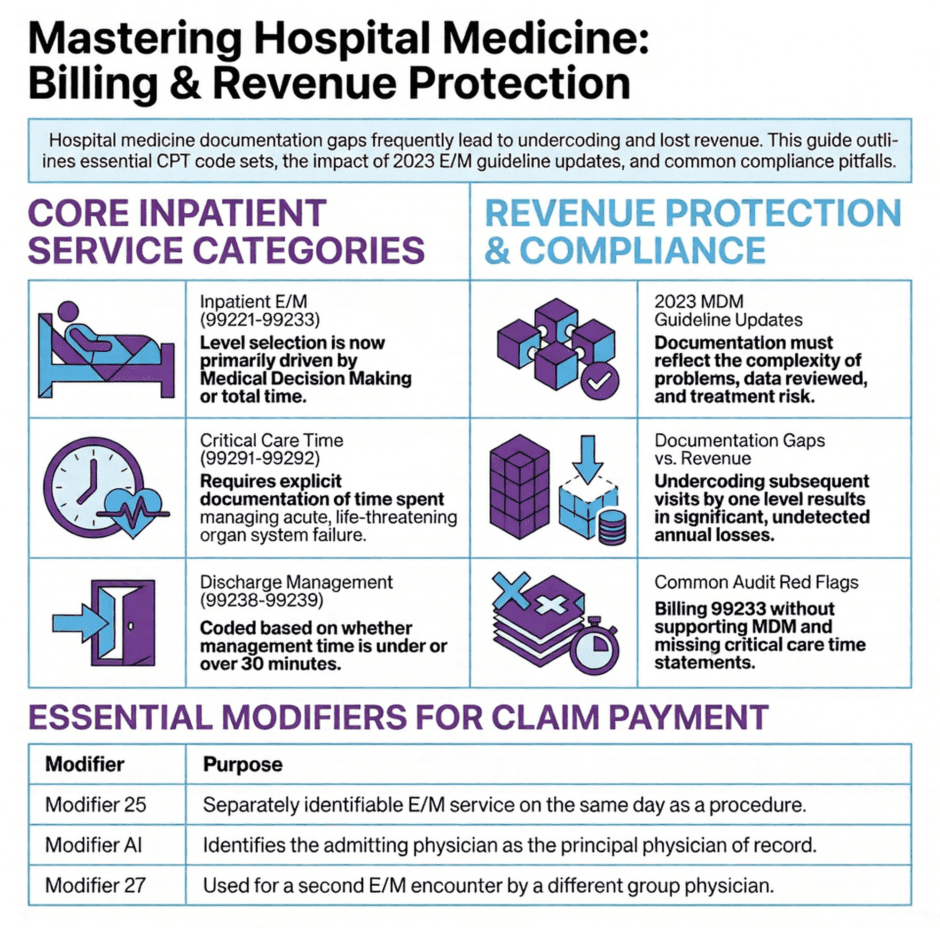
Discharge Management: Documentation That Earns Its Code
Discharge day management codes, CPT 99238 and 99239, cover the work of discharging a patient from the hospital. CPT 99238 is used when the total discharge management time is 30 minutes or less. CPT 99239 applies when that time exceeds 30 minutes.
The time threshold here is real and must be documented. The discharge management time includes face-to-face time with the patient, time spent coordinating post-discharge care, completing discharge orders, preparing the discharge summary, and communicating with the patient and family. It does not include time spent by nursing staff or other team members.
Discharge documentation is one of the most inconsistent areas in hospital medicine billing. A lot of hospitalists treat the discharge summary as an administrative formality rather than a clinical document that supports the billing code. When the note does not record the time spent or the work performed, the practice ends up defaulting to 99238 on every discharge regardless of what actually happened. For complex patients with lengthy discharges, that is a consistent undercoding pattern.
When a patient is admitted and discharged on the same calendar day, neither the initial hospital care codes nor the discharge codes apply. Observation or inpatient same-day codes are used instead, specifically CPT 99234 through 99236, depending on the level of medical decision making.
Critical Care Billing
 Critical care is billed differently from every other inpatient service, and it trips up even experienced hospitalists. CPT 99291 covers the first 30 to 74 minutes of critical care time for a given patient on a given date. CPT 99292 is used for each additional 30-minute block beyond 74 minutes. Both codes are time-based, which means the time must be documented explicitly.
Critical care is billed differently from every other inpatient service, and it trips up even experienced hospitalists. CPT 99291 covers the first 30 to 74 minutes of critical care time for a given patient on a given date. CPT 99292 is used for each additional 30-minute block beyond 74 minutes. Both codes are time-based, which means the time must be documented explicitly.
The definition of critical care under CPT guidelines is specific. The patient must have a critical illness or injury that acutely impairs one or more vital organ systems, and there must be a high probability of imminent or life-threatening deterioration. Not every sick patient qualifies. A hospitalist cannot bill critical care simply because a patient is in the ICU or is medically complex. The documentation has to establish that the patient met the critical care definition on that date.
Critical care time includes direct care at the bedside, time spent on the unit or floor reviewing results and discussing the patient’s case, and time documenting the encounter. It does not include time spent performing procedures that are separately billable, time in educational activities, or time spent on other patients. The total time must be documented in the note, not inferred.
When two physicians from the same group provide critical care to the same patient on the same day, the time is not additive for billing purposes. Only one critical care claim can be submitted per patient per day from the same group.
Observation Services
Observation billing is one of the most misunderstood areas in hospital medicine. Patients placed in observation status are not technically admitted as inpatients, but they are physically in the hospital and receiving physician care, which means billing rules apply that are distinct from standard inpatient codes.
Initial observation care uses CPT 99221 through 99223, the same code set as inpatient admission. Subsequent observation care uses 99231 through 99233. Observation discharge uses 99217. When a patient is admitted to and discharged from observation on the same calendar day, CPT 99234 through 99236 apply based on the level of medical decision making.
The compliance risk in observation billing comes from two directions. Some practices incorrectly bill inpatient codes for patients who are in observation status, which creates a claim mismatch that payers will catch. Others fail to bill observation services at all because the documentation workflow is set up around inpatient care and observation encounters fall through the cracks.
Knowing which patients are in observation status versus inpatient status at the time of service is a workflow issue, not just a coding issue. Practices that get daily census information with admission status clearly identified have far fewer observation billing errors than those that rely on physicians to track it themselves.
Procedures Hospitalists Perform
 Many hospitalists perform bedside procedures that are separately billable alongside the daily E/M service. These include central line placement, thoracentesis, paracentesis, lumbar puncture, arterial line placement, and intubation, among others.
Many hospitalists perform bedside procedures that are separately billable alongside the daily E/M service. These include central line placement, thoracentesis, paracentesis, lumbar puncture, arterial line placement, and intubation, among others.
Each of these procedures has its own CPT code and can be billed in addition to the daily inpatient visit as long as the documentation supports both services as distinct. The procedure note must describe what was performed, the indication, the technique, and the outcome. A brief mention of a procedure buried in the daily progress note is not sufficient documentation to support a separately billed procedure code.
Ultrasound guidance is frequently used for central line placement, thoracentesis, and paracentesis. When imaging guidance is used, a separate imaging guidance code is billable alongside the procedure code, provided the guidance was documented and an image was stored in the medical record. Skipping that documentation step is a consistent missed revenue opportunity.
Modifier Use in Hospital Medicine Billing
Modifiers in hospital medicine billing clarify the circumstances of a service. They are not optional additions. They are often what determines whether a claim is paid or denied.
The modifiers that come up most often in hospital medicine:
- Modifier 25 is used when a significant and separately identifiable E/M service is billed on the same day as a procedure. The E/M documentation must reflect decision making beyond the routine pre-service assessment for the procedure performed. Without this modifier on the E/M code, the payer will bundle it into the procedure payment.
- Modifier 27 applies when a patient is seen in observation or as an inpatient and a second E/M service is performed later that same day by a different physician in the same group practice. This modifier signals that the second visit is a separate encounter and not a duplicate claim.
- Modifier AI is used by the admitting physician to identify themselves as the principal physician of record for the inpatient admission. This matters because Medicare distinguishes between the admitting physician and consulting or co-managing physicians when processing inpatient claims from the same date.
- Modifier 52 covers situations where a service is partially reduced from what was originally planned. In hospital medicine, this occasionally applies when a planned procedure was started but not completed due to patient condition or other clinical circumstances.
Medical Decision Making in Hospital Medicine
 Since the 2023 AMA inpatient E/M guideline updates, medical decision making has become the primary driver of level selection for hospital medicine codes, alongside time. Getting familiar with how MDM is evaluated is not optional. It is the foundation of accurate billing across every inpatient service category.
Since the 2023 AMA inpatient E/M guideline updates, medical decision making has become the primary driver of level selection for hospital medicine codes, alongside time. Getting familiar with how MDM is evaluated is not optional. It is the foundation of accurate billing across every inpatient service category.
MDM is assessed across three elements: the number and nature of the problems being addressed, the amount and complexity of data reviewed and analyzed, and the risk level associated with the treatment plan. All three elements factor into the final level. A patient with three active chronic conditions being managed simultaneously, whose care requires review of external records and discussion with a specialist, and whose treatment involves a prescription drug with significant risk, supports high complexity MDM and a level 3 code.
The documentation trap is writing notes that describe what was done without capturing why the decision making was difficult. A hospitalist who spends 45 minutes working through a complex medication adjustment for a patient with multiple interacting conditions has done high-complexity work. If the note says “medications adjusted, will monitor,” that work is invisible to the coder and the payer. Write the note as if the reader has no clinical context. Spell out the data reviewed, the options considered, and the rationale behind the plan.
Hospital Medicine Credentialing Requirements
Credentialing for hospitalists follows the same general structure as other internal medicine physicians, with some practical details worth paying attention to. Board certification typically runs through the American Board of Internal Medicine (ABIM) or the American Board of Family Medicine (ABFM). Some hospitalists also hold subspecialty certification in areas like pulmonary or critical care medicine, which may be relevant for specific procedures or service lines.
Primary source verification for a hospitalist covers medical school education, residency training, any fellowship completed, board certification status, current state licensure, DEA registration, malpractice history, and hospital privileges at every facility where the physician practices. Each credential is verified directly from the issuing institution.
The NPDB query is required, and any adverse reports must be reviewed before credentialing is finalized. Hospital medicine groups that employ large numbers of physicians, or that use locum tenens coverage, often underestimate the administrative burden of keeping credentialing current across a rotating roster. Lapses in credentialing translate directly into unbillable encounters.
Multi-Site and Locum Tenens Considerations
 Hospital medicine groups that cover multiple facilities face credentialing requirements at each site. A physician credentialed at one hospital is not automatically credentialed at another, even within the same health system. Separate applications, separate privilege approvals, and separate payer enrollment may all be required.
Hospital medicine groups that cover multiple facilities face credentialing requirements at each site. A physician credentialed at one hospital is not automatically credentialed at another, even within the same health system. Separate applications, separate privilege approvals, and separate payer enrollment may all be required.
Locum tenens physicians add another layer. They must be credentialed and enrolled with payers before their claims can be processed. Using a locum without completing that process means submitting claims under another provider’s number, which creates compliance exposure, or not billing at all. Neither outcome is acceptable.
Starting the credentialing process early, tracking status actively, and building a defined workflow for new provider onboarding is what separates groups that bill from day one from those that absorb months of lost revenue every time a new physician joins the team.
Payer Contracting and Audit Risk
Payer contracting for hospital medicine groups is worth approaching with data behind you. Groups that cover an entire facility’s inpatient census, provide overnight and weekend coverage, or manage high-acuity populations have real leverage in contract negotiations. That leverage is often underused because groups do not go into contracting conversations with specialty-specific benchmarking data.
Audit risk in hospital medicine tends to concentrate in a few predictable areas:
- Level of care assignment without supporting documentation. Billing 99233 or 99223 without documentation that supports high complexity medical decision making is the most common audit finding in hospital medicine. The code has to be supported by the note, not just by how sick the patient was.
- Critical care time billing without documented time. Billing 99291 without a time statement in the note is a straightforward compliance problem. The time must be explicitly recorded, not estimated or inferred from the complexity of the encounter.
- Same-day billing errors. Billing both a subsequent care code and a discharge code on the same calendar day, or billing an initial care code and a subsequent care code for the same patient on the same date, are bundling errors that payers catch regularly and that auditors flag as systemic problems.
- Observation vs. inpatient status mismatches. Billing inpatient codes for patients who were in observation status is a frequent compliance finding, particularly in groups that do not have a clear real-time process for tracking admission status.
Hospital Medicine Billing FAQ
- What CPT codes do hospitalists use most often?
The core code set includes initial hospital care codes 99221 through 99223, subsequent care codes 99231 through 99233, discharge management codes 99238 and 99239, observation codes 99217 and 99234 through 99236, and critical care codes 99291 and 99292. Procedure codes for bedside procedures like central line placement and thoracentesis are added when those services are performed. The right code within each range depends on what the documentation supports. - How is medical decision making determined for inpatient visits?
MDM is evaluated across three areas: the problems being addressed, the data reviewed, and the risk level of the treatment. High complexity in any one area does not automatically mean high complexity overall. All three elements factor into the determination. The documentation needs to capture enough detail in each area to support the level selected. - Can a hospitalist bill for a procedure and an E/M visit on the same day?
Yes, when the documentation supports both as distinct services. The E/M note must reflect decision making beyond the pre-procedural assessment, and Modifier 25 must be appended to the E/M code. Without that modifier, the payer will bundle the E/M into the procedure payment. - What happens if a patient is admitted and discharged on the same day?
Same-day admission and discharge uses CPT 99234 through 99236, not the standard admission or discharge codes. Code selection within that range is based on the level of medical decision making. - How does critical care billing work when multiple physicians see the same patient?
When two physicians from the same group provide critical care to the same patient on the same calendar day, the time is not combined for billing purposes. Only one critical care claim per patient per day is billable by the group. The claim should reflect the total time that can be attributed to a single billing provider. - What documentation is required for discharge codes?
The discharge note must document the time spent on discharge management. CPT 99238 covers 30 minutes or less, and 99239 covers more than 30 minutes. The time documented should include face-to-face time with the patient, coordination of post-discharge care, and preparation of discharge instructions and summary. Time spent by nursing or other clinical staff is not included.
Hospitalists also Ask
- Is it acceptable to bill the same level of subsequent care every day for a long-stay patient?
It depends entirely on what the documentation supports each day. A long-stay patient who is medically stable and requires minimal management may genuinely warrant a 99231 consistently. A patient whose condition is actively changing and whose care requires daily data review and clinical decision making may support 99232 or 99233 repeatedly. The code should reflect what happened that day, not what is easiest to document. - What is the difference between observation and inpatient status for billing purposes?
Observation is a billing and utilization status, not a physical location. Patients in observation are technically outpatients even though they are in a hospital bed. This affects which codes apply, how cost-sharing is calculated for the patient, and how Medicare processes the claim. The physician billing codes are similar but not identical between the two statuses, and submitting inpatient codes for an observation patient creates a claim mismatch. - Can a hospitalist bill for a family meeting as a standalone service?
In most cases, no. Time spent communicating with a patient’s family is generally included in the overall time used for E/M level selection on that day’s encounter. It is not separately billable as a standalone service unless specific care coordination codes or advance care planning codes apply, which have their own documentation requirements. - What are the most common reasons hospital medicine claims get denied?
Missing or insufficient documentation for the level of care billed, critical care claims without documented time, same-day billing errors involving duplicate codes for the same patient, observation status mismatches, and procedures billed without a supporting procedure note are the most frequent denial causes in hospital medicine. Most of these are preventable with a structured pre-billing documentation review process.
How Medwave Supports Hospital Medicine Groups
 Hospital medicine billing requires sustained attention at every step of the revenue cycle. Getting the right level of care assigned based on documented medical decision making, managing critical care time accurately, keeping observation and inpatient billing separated, and tracking credentialing across a rotating provider roster all require people who know hospital medicine billing specifically, not just general inpatient coding.
Hospital medicine billing requires sustained attention at every step of the revenue cycle. Getting the right level of care assigned based on documented medical decision making, managing critical care time accurately, keeping observation and inpatient billing separated, and tracking credentialing across a rotating provider roster all require people who know hospital medicine billing specifically, not just general inpatient coding.
At Medwave, we provide medical billing, provider credentialing, and payer contracting services to hospital medicine groups across the country. Our billing team works directly with inpatient E/M code sets, critical care documentation standards, and the payer-specific policies that affect how your claims get processed. Our credentialing team manages the full physician credentialing process for hospitalists, including ABIM and ABFM certification verification, multi-site privilege coordination, locum tenens onboarding, and PECOS enrollment. Our payer contracting work helps hospital medicine groups negotiate rates and contract terms that reflect the value of full inpatient coverage, including nights, weekends, and high-acuity patient management.
If your group has not recently reviewed its coding patterns, level of care distribution, or credentialing timelines, that review is worth having before a denial trend or payer audit forces the issue.
Contact Medwave today to schedule a hospital medicine billing and credentialing review.
