Medical Credentialing, Payer Contracting, & Billing
Medwave provides medical credentialing, payer contracting, and medical billing services to healthcare practices across the country. We work with independent physicians, group practices, allied health providers, and multi-specialty organizations, handling the administrative infrastructure that determines how much a practice collects and how quickly it gets paid.
Most practices lose revenue not because of the care they deliver, but because of what happens after the patient leaves. Denied claims, credentialing delays, and unfavorable payer contracts quietly erode collections month after month. Medwave exists to fix that.
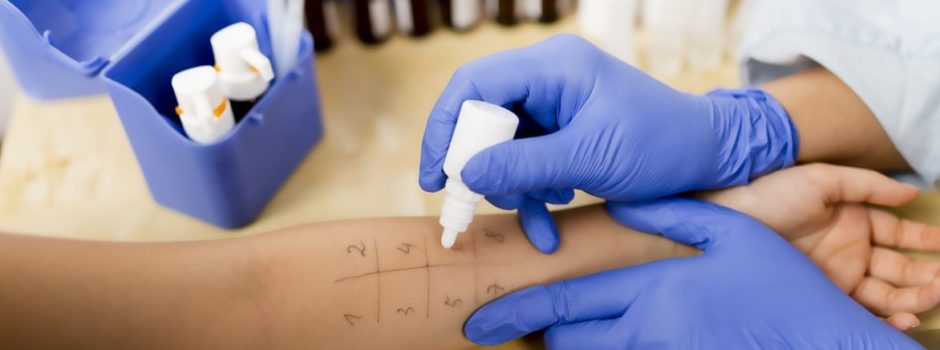
Our credentialing team manages provider enrollment with Medicare, Medicaid, and commercial payers from initial application through approval, tracking every deadline and following up on every pending status so your providers can see patients and get paid without unnecessary gaps. We also handle recredentialing cycles and CAQH profile maintenance so nothing lapses.
On the contracting side, we review your current payer agreements, identify rates that are below market, and negotiate directly with payers on your behalf. Most practices have never had their contracts systematically reviewed, which means they are collecting less than they should be on every single claim.
Our billing team handles charge capture, coding review, claim submission, payment posting, and denial management. We work across specialties and practice types, and we do not outsource the work overseas. Every account is managed by experienced billing staff who understand how to push back on payers when claims are wrongly denied.
Medical Credentialing

Medwave manages provider credentialing for healthcare practices across the country, including initial enrollment, CAQH setup, payer-specific applications, and revalidation tracking. We have credentialed providers across every major specialty for over 30 years.
Simplified CredentialingPayer Contracting

Most payer contracts are signed once and never revisited. Medwave reviews your existing contracts, identifies where you are being underpaid by CPT code, and negotiates better rates directly with payers on your behalf using your own claims data.
Payer Contracting ExpertiseMedical Billing