Plastic surgery is one of the most billing-intensive specialties in medicine. Full stop. On any given day, a plastic surgeon might reconstruct a breast following mastectomy, repair a complex traumatic laceration, excise a skin cancer and close the defect with a flap, perform a hand surgery procedure, and see a full clinic of post-operative patients. That breadth of work is what makes plastic surgery so essential across both reconstructive and aesthetic medicine. It is also what makes plastic surgery billing one of the most technically demanding areas in the entire revenue cycle.
 The CPT codes used in plastic surgery span wound repair, skin grafting, flap reconstruction, burn treatment, breast procedures, hand surgery, craniofacial surgery, body contouring, and evaluation and management visits. Each of those categories has its own coding logic, documentation requirements, and payer rules. Add the ever-present distinction between reconstructive and cosmetic procedures, prior authorization requirements for high-cost reconstructive cases, global period management across staged surgeries, and payer-specific policies on what qualifies as medically necessary, and you end up with a billing environment where documentation gaps translate directly and quickly into lost revenue.
The CPT codes used in plastic surgery span wound repair, skin grafting, flap reconstruction, burn treatment, breast procedures, hand surgery, craniofacial surgery, body contouring, and evaluation and management visits. Each of those categories has its own coding logic, documentation requirements, and payer rules. Add the ever-present distinction between reconstructive and cosmetic procedures, prior authorization requirements for high-cost reconstructive cases, global period management across staged surgeries, and payer-specific policies on what qualifies as medically necessary, and you end up with a billing environment where documentation gaps translate directly and quickly into lost revenue.
Below, we cover how plastic surgery billing works across the major service categories, what credentialing looks like for plastic surgeons, where compliance risk tends to concentrate, and what your practice can do to protect revenue from the start.
TL;DR:
Plastic surgery billing spans reconstructive and cosmetic procedures, each governed by entirely different coverage rules:
- Reconstructive procedures require thorough medical necessity documentation, correct approach-specific CPT codes, and careful global period management
- Cosmetic procedures are not covered by insurance and must be handled through a completely separate billing workflow
- Credentialing for plastic surgeons runs through the American Board of Plastic Surgery and requires primary source verification of training, licensure, surgical privileges, and malpractice history
What Makes Plastic Surgery Billing So Demanding?
The short answer is that plastic surgery sits at the intersection of two completely different financial worlds. Reconstructive procedures are billed to insurance and subject to all the rules, documentation requirements, and prior authorization demands that come with that. Cosmetic procedures are paid directly by patients and require a separate workflow, separate fee schedules, and separate consent and financial agreement processes. Managing both simultaneously, sometimes for the same patient on the same day, requires a billing operation that is genuinely built for plastic surgery rather than adapted from a general surgical template.
Beyond that core split, plastic surgery procedures are often staged. A breast reconstruction may involve multiple surgeries over months. A burn patient may need repeated debridements and grafting sessions. A patient with a complex wound may require sequential flap revisions. Each stage has its own billing, its own global period considerations, and its own documentation requirements. A practice that does not actively track where each patient sits in a staged treatment course will consistently make billing errors that are difficult to catch and even harder to reverse after the fact.
The volume of distinct CPT codes used in plastic surgery is also significant. Repair codes alone span simple, intermediate, and complex closures, each with their own length-based thresholds and anatomical location rules. Flap codes separate by type of flap, donor site, and recipient site. Breast codes differ by whether the procedure is reconstruction, revision, or augmentation. Knowing which code applies requires both clinical knowledge and coding expertise specific to this specialty.
The Reconstructive vs. Cosmetic Distinction: Everything Flows From Here
 No concept matters more in plastic surgery billing than the line between reconstructive and cosmetic services. Get this wrong and everything else falls apart.
No concept matters more in plastic surgery billing than the line between reconstructive and cosmetic services. Get this wrong and everything else falls apart.
Reconstructive procedures are performed to correct abnormalities caused by congenital defects, developmental abnormalities, trauma, infection, tumors, or disease. They are covered by insurance when properly documented and coded. Cosmetic procedures are performed to reshape normal structures of the body to improve appearance. They are not covered by insurance, period, regardless of how they are documented or coded.
The challenge is that the same technical procedure can be reconstructive in one patient and cosmetic in another. A blepharoplasty performed to correct visual field obstruction caused by ptosis is reconstructive and billable to insurance with proper documentation. The same procedure performed purely to improve appearance is cosmetic and must be billed directly to the patient. A rhinoplasty following nasal trauma is reconstructive. A rhinoplasty performed for aesthetic preference is cosmetic.
The documentation is what makes the difference visible to the payer. A clinical note that describes the functional impairment, the objective findings, and the medical rationale for the procedure is what supports insurance reimbursement. A note that describes only appearance-related concerns does not. Plastic surgery practices that do not train their clinical team to document the functional and medical basis for reconstructive procedures will consistently see those claims denied, even when the procedure was genuinely reconstructive in nature.
Wound Repair and Closure Codes
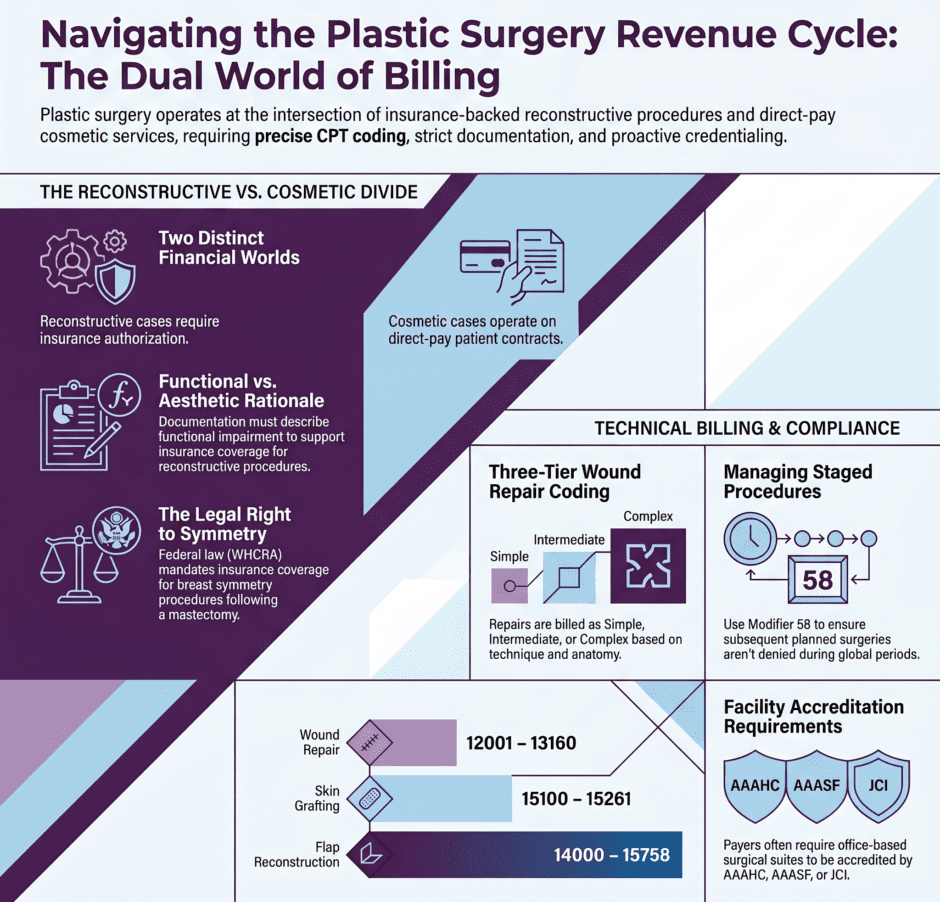
Wound repair is one of the most frequently billed categories in plastic surgery and one of the most frequently miscoded. The repair codes split into three tiers: simple (12001 to 12021), intermediate (12031 to 12057), and complex (13100 to 13160). Each tier covers a different level of closure work, and the code within each tier is selected based on the total length of the repair and the anatomical location.
Simple repairs involve single-layer closure of superficial wounds. Intermediate repairs involve layered closure of deeper tissue or wounds that require significant cleaning or debridement before closure. Complex repairs involve more involved techniques such as scar revision, debridement, extensive undermining, retention sutures, or other complex wound preparation. The technique used, not just the wound characteristics, determines which tier applies.
Length is added across wounds in the same anatomical grouping when multiple wounds are repaired during the same session. The total length is what drives code selection within the tier. Wounds in different anatomical groupings are coded separately, each with their own length calculation. The documentation must record the specific site, the wound dimensions, and the closure technique for each repair performed.
A few things worth knowing about repair coding in plastic surgery:
- Adjacent tissue transfer and rearrangement codes (14000 to 14350) apply when closure requires a local flap. These codes are selected based on the size of the defect, not the total area of tissue moved. The defect size must be clearly documented, and the flap technique described in enough detail to support the code selected.
- Repair codes and excision codes on the same day follow specific bundling rules. Simple repairs following skin excisions are included in the excision code and not separately billable. Intermediate and complex repairs following excisions can be separately reported when the documentation supports the additional complexity of the closure.
- Multiple repairs in the same tier and anatomical grouping are combined into a single code with a total length. Billing multiple separate codes for each wound rather than combining them is a common error that payers will catch and that can trigger a broader review of the practice’s billing patterns.
- Scar revision uses different codes than standard wound repair. Z-plasty, W-plasty, and geometric broken line closure each have their own CPT codes that reflect the specific technique used rather than just the length of the repair.
Skin Grafting
 Skin grafting is a core plastic surgery service with its own coding structure that trips up even experienced billing teams. The code selection depends on the type of graft, the size of the recipient site, and whether the procedure involves split-thickness or full-thickness tissue.
Skin grafting is a core plastic surgery service with its own coding structure that trips up even experienced billing teams. The code selection depends on the type of graft, the size of the recipient site, and whether the procedure involves split-thickness or full-thickness tissue.
Split-thickness skin grafting uses codes from the 15100 and 15101 series, selected by recipient site size and whether the procedure is initial or a repeat application. Full-thickness skin grafting uses codes from the 15200 through 15261 range, which are organized by both the recipient site size and the anatomical location of the donor site. The documentation needs to specify the graft type, the dimensions of the recipient site, and the donor site location for code selection to be accurate.
Donor site closure is a separate billing consideration. When a split-thickness graft donor site requires a graft to close it, that secondary grafting procedure is separately billable. When it heals by secondary intention, it is not. The operative note should describe what was done at the donor site to support whatever billing approach is used.
Acellular dermal matrix products, used in conjunction with grafting for certain reconstructive cases, have their own HCPCS codes and billing rules that are separate from the grafting procedure codes. Many payers require prior authorization for these products, and the specific product used must be documented by name and lot number to support the supply claim.
Flap Reconstruction
Flap procedures are among the most technically demanding and highest-value services in plastic surgery, and the billing for them reflects that. The code selection depends on the type of flap, the method of transfer, and the anatomical sites involved at both the donor and recipient locations.
Local flaps, including rotation, advancement, and transposition flaps, use codes from the 14000 to 14350 range based on defect size and location. Pedicle flaps use codes from the 15570 to 15738 range, organized by the anatomical location of the flap and the recipient site. Free flaps, which involve microvascular anastomosis to reconnect the blood supply at a remote recipient site, use codes from the 15756 to 15758 range for soft tissue free flaps, with separate codes for specific free flap types such as the TRAM and DIEP used in breast reconstruction.
The operative report for a flap procedure needs to describe the type of flap, the donor site, the recipient site, the dimensions of both, the vascular pedicle or anastomosis details for free flaps, and the closure performed at the donor site. Incomplete operative reports are the leading cause of flap billing errors and denials, because coders cannot select the correct code without knowing the specific technique and sites involved.
When a flap procedure is performed as part of a staged reconstruction, Modifier 58 is used to identify each subsequent stage as a planned procedure. Without that modifier, the second and subsequent stages may be incorrectly bundled into the global period of the first procedure.
Breast Reconstruction Billing
 Breast reconstruction is one of the most clinically and administratively involved areas of plastic surgery billing. Federal law under the Women’s Health and Cancer Rights Act requires most group health plans to cover breast reconstruction following mastectomy, which means these services are covered by insurance when properly documented. But the coding and documentation requirements are specific enough that errors are common.
Breast reconstruction is one of the most clinically and administratively involved areas of plastic surgery billing. Federal law under the Women’s Health and Cancer Rights Act requires most group health plans to cover breast reconstruction following mastectomy, which means these services are covered by insurance when properly documented. But the coding and documentation requirements are specific enough that errors are common.
Implant-based reconstruction uses CPT 19340 for immediate placement and 19342 for delayed placement. Tissue expander placement, which is often the first stage in a two-stage implant reconstruction, uses CPT 19357. Tissue expander exchange for a permanent implant uses CPT 11970. Each of those stages is a separate procedure with its own code and its own documentation requirements.
Autologous reconstruction using the patient’s own tissue involves a separate set of codes based on the flap technique used. TRAM flap reconstruction uses CPT 19367 for a unipedicle TRAM. DIEP flap and other perforator-based free flaps use 19364. Latissimus dorsi flap reconstruction uses 19361. When implant placement accompanies an autologous flap in the same session, both the flap code and the implant code may be separately reportable depending on the payer.
Contralateral breast procedures performed to achieve symmetry, including augmentation, mastopexy, or reduction of the opposite breast, are also covered under the Women’s Health and Cancer Rights Act when performed in conjunction with post-mastectomy reconstruction. These are frequently under-billed because clinical teams assume the symmetry procedure is cosmetic. When properly documented as part of a reconstructive plan following mastectomy, they are covered services.
Hand Surgery Billing
Many plastic surgeons perform a significant volume of hand surgery, which falls under a dedicated CPT code range and carries its own specific coding rules. Hand surgery codes cover fracture care, tendon repair, nerve repair, Dupuytren’s contracture release, carpal tunnel release, trigger finger release, ganglion cyst removal, and replantation procedures.
Tendon repair codes differ based on whether the repair is primary or secondary, the anatomical zone of the hand where the repair occurs, and whether flexor or extensor tendons are involved. Zone-specific coding for flexor tendon repairs is a common source of errors because the zones are not always described in operative reports with the specificity needed for accurate coding.
Carpal tunnel release uses CPT 64721 for an open release and a different code for endoscopic release. Both are commonly performed, and the approach must be clearly stated in the operative report. Billing the wrong approach code is a documentation-to-code mismatch that auditors specifically look for in hand surgery claims.
When multiple hand procedures are performed in the same session, NCCI bundling rules apply and must be reviewed before submitting the claim. Some combinations of hand procedures are bundled under CCI edits, while others are legitimately separately billable with the correct modifier and documentation.
Burn Treatment Billing
 Burn care billing is a specialty within a specialty. The codes used for burn treatment cover initial assessment, debridement, grafting, and dressing changes, each with their own rules and documentation requirements.
Burn care billing is a specialty within a specialty. The codes used for burn treatment cover initial assessment, debridement, grafting, and dressing changes, each with their own rules and documentation requirements.
Burn debridement uses codes from the 16020 to 16030 range for non-surgical dressing changes and debridement, selected based on the size of the burn area. Surgical debridement of burn tissue uses separate codes that reflect the more involved nature of the procedure. The surface area involved, expressed as a percentage of total body surface area, must be documented in the clinical record for virtually every burn-related billing code.
Repeat debridements during an ongoing burn treatment course are separately billable when performed on different dates of service, or when performed under anesthesia on the same date as another procedure. The distinction between what is included in a global period and what can be separately billed requires careful tracking in burn patients who undergo multiple procedures over an extended course of care.
Cosmetic Procedure Billing
Cosmetic procedures deserve their own section because they operate under completely different rules than reconstructive work. There is no insurance claim. There is no medical necessity requirement. There is no global period in the traditional payer sense. It is a direct pay transaction between the practice and the patient, and it needs to be treated that way administratively from the start.
That means clear written financial agreements before the procedure is performed, upfront collection of fees, and a fee schedule that is set by the practice rather than dictated by payer contracts. It also means that no CPT code submitted to an insurance company should reflect a procedure performed for cosmetic reasons. Submitting a cosmetic procedure to insurance, even under a technically correct CPT code, and receiving payment for it is fraudulent billing regardless of intent.
The most common compliance risk in plastic surgery is not intentional fraud. It is documentation that blurs the line between reconstructive and cosmetic indications. A practice that routinely documents functional concerns for procedures that are primarily cosmetic, or that bills insurance for procedures without a clearly documented reconstructive rationale, is creating significant compliance exposure. Regular internal audits of cosmetic vs. reconstructive documentation patterns are one of the most important risk management tools available to plastic surgery practices.
Modifier Use in Plastic Surgery Billing
Modifiers do a lot of work in plastic surgery claims. They clarify the circumstances of a service, explain why a code that looks unusual is actually correct, and prevent legitimate claims from being incorrectly denied as duplicates or bundles.
The modifiers that come up most often in plastic surgery billing:
- Modifier 25 applies when a significant and separately identifiable E/M service is performed on the same day as a procedure. In plastic surgery, this is common when a patient is seen for a wound check or a clinical evaluation and a minor procedure is also performed at the same visit. The E/M documentation must reflect work beyond the routine pre-service assessment for the procedure.
- Modifier 58 identifies a staged procedure performed during the postoperative global period of a prior procedure, when that second stage was planned as part of a defined treatment course. Breast reconstruction stages, sequential burn grafting procedures, and planned flap revisions all typically require this modifier on the subsequent procedure claim.
- Modifier 59 is used to identify a distinct procedural service that would otherwise be bundled with another code, when the procedures were performed at clearly separate anatomical sites or under clinically distinct circumstances. It should be used precisely. Using it broadly to override bundles without clear documentation support is a compliance risk.
- Modifier 22 applies when a procedure required significantly more work than the standard description covers. Extensive scar tissue, prior failed repairs, or unusual anatomical variations that meaningfully increased the operative time and difficulty can support this modifier. The operative report must describe in specific terms why the case was more demanding than typical, and the claim should include a brief narrative supporting the additional work.
Prior Authorization in Plastic Surgery
 Prior authorization requirements in plastic surgery are significant and getting more extensive. Reconstructive procedures that involve high implant costs, advanced flap techniques, or staged surgical plans often require detailed pre-authorization before the payer will commit to covering the service.
Prior authorization requirements in plastic surgery are significant and getting more extensive. Reconstructive procedures that involve high implant costs, advanced flap techniques, or staged surgical plans often require detailed pre-authorization before the payer will commit to covering the service.
Breast reconstruction prior authorization typically requires documentation of the mastectomy, the reconstruction plan, the specific technique to be used, and the expected staging. Some payers also require documentation of why a particular technique was chosen over alternatives. Submitting an incomplete authorization request and receiving a denial means starting the process over, which delays the patient’s care and the practice’s revenue.
Hand surgery procedures increasingly require prior authorization, particularly for procedures like tendon reconstruction, nerve repair, and Dupuytren’s release. Some payers want conservative treatment documentation showing that non-surgical options were tried before approving a surgical approach.
The most practical approach is to assign dedicated staff to manage prior authorization as a defined workflow, with clear timelines, a tracking system for authorization status and expiration dates, and a defined escalation process when initial requests are denied. Practices that manage authorization reactively, checking only when a denial comes back, consistently lose more revenue to authorization failures than those with a proactive process in place.
Plastic Surgery Credentialing Requirements
Credentialing for plastic surgeons follows the same general structure as other surgical specialties but carries some specific requirements worth knowing. Board certification runs through the American Board of Plastic Surgery (ABPS), which requires completion of an accredited plastic surgery residency, passage of both written and oral examinations, and documentation of a defined case volume. Some plastic surgeons also hold certification from the American Board of Surgery prior to their plastic surgery training, and some hold additional credentials in subspecialty areas such as hand surgery or craniofacial surgery.
Primary source verification for a plastic surgeon covers medical school education, residency and any fellowship training, ABPS certification status, current state licensure in every state where the provider practices, DEA registration, malpractice history, and surgical privileges at every facility where the physician operates. Each credential is verified from the issuing institution, not from copies provided by the physician.
The NPDB query is required, and any adverse history must be reviewed and addressed before credentialing is complete. Plastic surgery practices that add new surgeons frequently underestimate the credentialing timeline, and the gap between a physician’s clinical start date and their payer enrollment completion date can represent weeks or months of delayed billing.
Facility Accreditation for Office-Based Surgery
Plastic surgeons who perform procedures in an office-based surgical suite rather than a hospital or ambulatory surgery center face an additional credentialing layer. Most payers require that office-based surgical facilities meet specific accreditation standards, typically through organizations such as AAAHC, AAASF, or The Joint Commission.
If a plastic surgeon performs procedures in an unaccredited office suite, payers may refuse to reimburse those services even when the physician’s individual credentials are in order. Verifying that the surgical facility holds the required accreditation, and that accreditation is current, is an often-overlooked step in the credentialing process for plastic surgery groups.
Payer Contracting and Audit Risk in Plastic Surgery
Payer contracting for plastic surgery groups is worth approaching with procedure-specific data and a clear understanding of the reconstructive services your group provides. Groups that deliver post-mastectomy reconstruction, complex trauma reconstruction, burn care, or pediatric craniofacial surgery have real leverage in contracting conversations that practices focused primarily on cosmetic work do not.
Audit risk in plastic surgery tends to concentrate in these areas:
- Reconstructive vs. cosmetic documentation failures. Billing insurance for procedures without clearly documented reconstructive medical necessity is the highest-priority audit target in plastic surgery. The clinical indication must be explicit in the chart note, not implied or inferrable from the diagnosis code alone.
- Repair code bundling errors. Billing separate repair codes for wounds that should be combined into a single code by total length and anatomical grouping, or billing intermediate and complex repair codes alongside excision codes when the repair is included, are frequent errors in plastic surgery claims.
- Staged procedure billing without Modifier 58. Billing subsequent stages of a reconstructive procedure during the global period of the first stage without the correct modifier results in the claim being denied as included in the prior surgery payment.
- Flap and graft documentation gaps. Operative reports that do not specify the flap type, donor site dimensions, and recipient site characteristics prevent accurate code selection and create both undercoding and audit risk when the wrong code is selected by default.
Plastic Surgery Billing FAQ
- What CPT codes are most commonly used in plastic surgery billing?
The core code set spans repair codes from 12001 through 13160, adjacent tissue transfer codes from 14000 to 14350, skin graft codes from 15100 to 15261, flap codes from 15570 to 15758, breast reconstruction codes from 19340 to 19369, hand surgery codes across the 26000s, burn treatment codes from 16020 to 16036, and E/M codes 99202 through 99215 for clinic visits. The right code within each range depends on the technique used, the anatomical sites involved, and the specific details documented in the operative report. - How do you document medical necessity for reconstructive plastic surgery?
The clinical note needs to explicitly describe the functional impairment or medical condition being treated, the objective findings on examination, the patient’s relevant history, and the clinical rationale for the procedure being performed. Vague language about appearance or patient preference does not support a reconstructive claim. Specific descriptions of functional limitation, wound characteristics, tumor involvement, or congenital abnormality do. When in doubt, more documentation is better than less. - Is breast symmetry surgery covered by insurance after mastectomy?
Yes, when performed as part of post-mastectomy reconstruction. The Women’s Health and Cancer Rights Act requires most group health plans to cover procedures on the contralateral breast to achieve symmetry following mastectomy reconstruction. The documentation should clearly connect the symmetry procedure to the reconstructive plan, and prior authorization is typically required before the procedure is performed. - How does the global surgery period affect staged plastic surgery procedures?
Major surgical procedures carry a 90-day global period during which routine post-operative care is bundled into the original payment. When a subsequent stage of a planned reconstructive procedure is performed during that global period, Modifier 58 is used to identify it as a planned staged procedure rather than a complication or unrelated service. Without that modifier, the second stage claim will typically be denied as included in the first procedure’s global payment. - What accreditation does an office-based surgical suite need for plastic surgery?
Most payers require accreditation through AAAHC, AAASF, or The Joint Commission for office-based surgical facilities. The specific requirement varies by payer. Performing procedures in an unaccredited facility can result in those claims being denied at the payer level regardless of the surgeon’s individual credentials. Verifying facility accreditation status and keeping it current is an important part of the overall credentialing picture for plastic surgery practices. - What prior authorization is typically required for breast reconstruction?
Most payers require documentation of the mastectomy, the planned reconstruction technique, the staging plan, and clinical justification for the approach selected. Some payers also require documentation that the patient was offered reconstruction and information about their options, as required under federal law. Submitting a complete and detailed authorization request from the start reduces the rate of initial denials and gets the patient’s treatment on track faster.
Plastic Surgeons Also Ask
- Can a plastic surgeon bill for both a flap and a graft in the same operative session?
It depends on the clinical circumstances and the NCCI bundling rules for the specific codes involved. When a flap and a graft are performed at clearly distinct anatomical sites for distinct clinical indications, separate billing may be supported with appropriate modifier use and documentation. When they are performed as part of a single reconstructive effort at the same site, bundling rules may apply. The operative report needs to clearly describe the distinct indication and site for each procedure to support separate billing. - What is the most common reason plastic surgery claims get denied?
Insufficient documentation of medical necessity for reconstructive procedures is the leading denial cause in plastic surgery. After that, repair code bundling errors, global period billing without the correct modifier, and prior authorization failures for elective reconstructive cases are the most frequent problems. Nearly all of these are preventable with strong clinical documentation and a defined pre-billing review process. - How are cosmetic procedure fees structured without insurance?
Cosmetic procedure fees are set by the practice based on the surgeon’s time, the facility costs, and market factors. They are collected directly from the patient through upfront payment or a defined payment plan established before the procedure. Written financial agreements signed by the patient before the procedure is scheduled are standard practice and important from both a business and a compliance standpoint. - Does hand surgery performed by a plastic surgeon require separate credentialing?
The hand surgery privileges are credentialed through the facility where the procedures are performed, based on the surgeon’s documented training and case volume. A plastic surgeon who completed hand surgery fellowship training or who has significant documented hand surgery volume will typically have fewer barriers to privilege approval than one who did not, regardless of their overall plastic surgery credentials. Starting the privilege application process early and providing thorough documentation of training and case volume is the most practical approach.
How Medwave Supports Plastic Surgery Practices
 Plastic surgery billing requires precision, specialty-specific expertise, and a billing team that knows the difference between a reconstructive indication and a cosmetic one before a claim ever goes out the door. Managing repair code combinations, flap and graft documentation requirements, staged procedure modifiers, and prior authorization across a reconstructive case load takes more than general surgical billing knowledge.
Plastic surgery billing requires precision, specialty-specific expertise, and a billing team that knows the difference between a reconstructive indication and a cosmetic one before a claim ever goes out the door. Managing repair code combinations, flap and graft documentation requirements, staged procedure modifiers, and prior authorization across a reconstructive case load takes more than general surgical billing knowledge.
At Medwave, we provide medical billing, provider credentialing, and payer contracting services to plastic surgery practices and surgical groups across the country. Our billing team works directly with plastic surgery CPT code sets, operative report documentation standards, and the payer-specific policies that govern reconstructive versus cosmetic coverage determinations. Our credentialing team manages the full physician credentialing process for plastic surgeons, including ABPS certification verification, office-based surgical facility accreditation review, multi-state licensure tracking, and PECOS enrollment. Our payer contracting work helps plastic surgery practices negotiate rates and contract terms that reflect the true value of reconstructive services, particularly for high-complexity cases like free flap reconstruction, burn care, and post-mastectomy breast reconstruction.
If your plastic surgery practice has not recently reviewed its coding patterns, reconstructive documentation standards, or credentialing timelines, that review is worth scheduling before a denial trend or payer audit forces the conversation.
Contact Medwave today to schedule a plastic surgery billing and credentialing review.
