Payer contract negotiation is governed by a layered set of federal and state laws that determine what insurance companies can and cannot do when contracting with providers. Federal frameworks include antitrust rules enforced by the FTC and DOJ, the No Surprises Act’s restrictions on balance billing and network adequacy, and Medicare and Medicaid participation requirements. State laws add a second layer, covering prompt payment timelines, any-willing-provider rules, parity requirements for behavioral health, and in some states, minimum reimbursement floors tied to Medicare rates.
Providers who know those rules before they negotiate are in a materially different position than those who do not. A payer cannot lawfully do certain things in a contract, and many of the terms that appear in standard participation agreements are negotiable or challengeable when they conflict with applicable law.
This article covers the most consequential federal and state rules affecting payer contract negotiations, what providers can use them for at the table, and where the legal boundaries sit that payers cannot cross regardless of what the contract language says.
TL;DR
- Payer contract negotiation is a regulated process governed by both federal and state law, knowing those rules gives providers real leverage at the table.
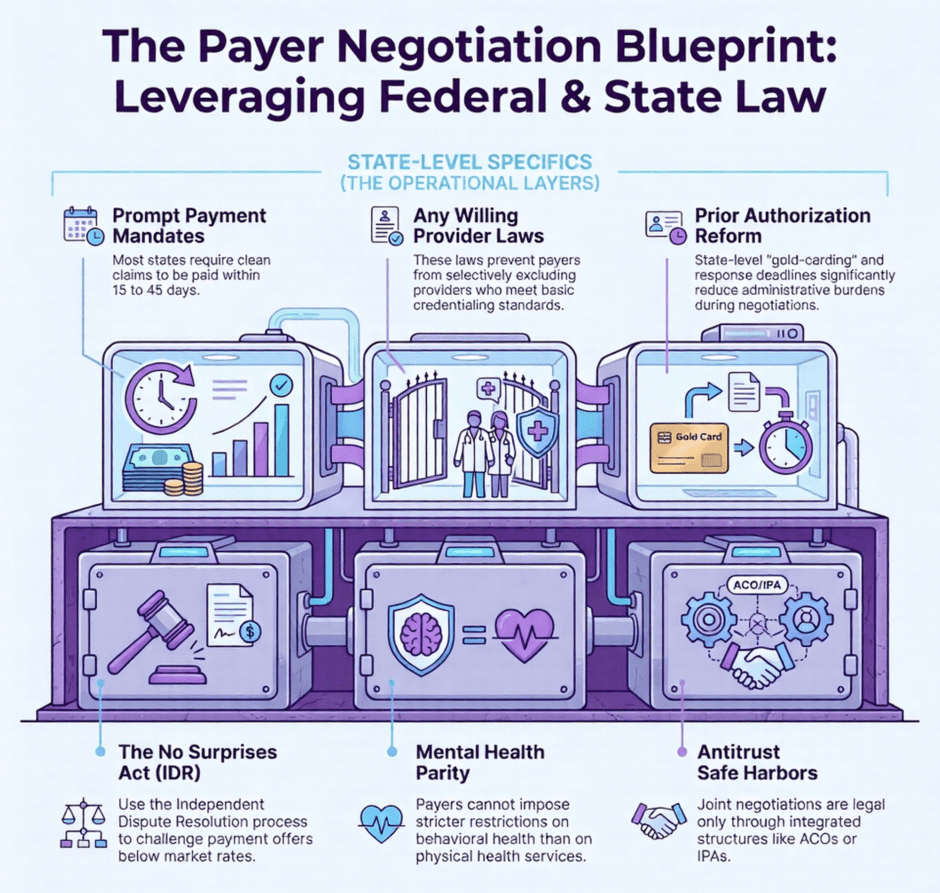
- The No Surprises Act introduced the Independent Dispute Resolution (IDR) process, giving providers a formal way to challenge low out-of-network payment offers.
- The Mental Health Parity Act requires payers to cover behavioral health services under terms no more restrictive than medical and surgical benefits, making it an underused negotiation tool for behavioral health providers.
- Federal antitrust law prohibits independent competing providers from negotiating collectively, though integrated structures like ACOs and IPAs have defined safe harbors.
- The Affordable Care Act’s network adequacy requirements create leverage for providers who fill genuine gaps in a payer’s network.
- State laws add another layer. Any willing provider laws, prompt payment requirements, balance billing protections, and prior authorization reform rules all vary by state and directly affect contract negotiations.
- ERISA-governed self-funded employer plans are generally not subject to state insurance mandates, which changes which rules apply during negotiations with those payers.
- Payer contracts often contain unilateral amendment clauses that allow changes without provider consent, reviewing those terms before signing matters.
The Two Layers of Payer Contracting Regulation
 Payer contracting is governed at two levels, and both matter. Federal law sets the baseline rules that apply across the country. State law often goes further, adding protections and requirements that vary considerably depending on where a provider practices.
Payer contracting is governed at two levels, and both matter. Federal law sets the baseline rules that apply across the country. State law often goes further, adding protections and requirements that vary considerably depending on where a provider practices.
Federal rules tend to address the big structural issues: antitrust compliance, out-of-network billing protections, mental health parity, and network adequacy under the Affordable Care Act. State rules get more granular, covering things like how quickly payers have to pay claims, whether payers must accept any willing provider into their network, and how prior authorization requests have to be handled.
The important thing to know is that these two layers work together. A payer cannot hide behind federal law to avoid a stronger state requirement, and a state cannot grant providers rights that conflict with federal statute. Knowing both levels gives you a much clearer picture of where you actually stand.
Key Federal Laws That Affect Payer Contract Negotiations
Several federal laws come into play whenever a provider sits down to negotiate a payer contract. Some of them are well known. Others are underused simply because providers do not realize they apply.
The No Surprises Act is one of the most significant shifts in payer contracting in recent years. It took effect in 2022 and changed the rules around out-of-network billing, balance billing protections, and how payment disputes get resolved. One of its most useful provisions for providers is the Independent Dispute Resolution process, or IDR. When a provider and payer cannot agree on payment for an out-of-network service, either party can initiate the IDR process and have an independent arbitrator determine the appropriate payment amount. This process gives out-of-network providers a meaningful way to push back on low payment offers without simply absorbing the loss. It has also changed the dynamic in in-network negotiations, because payers know that providers now have a formal alternative if contract terms fall too far below market rates.
The Mental Health Parity and Addiction Equity Act requires payers to cover mental health and substance use disorder services on terms that are no more restrictive than how they cover medical and surgical services. In plain terms, payers cannot impose stricter prior authorization requirements, lower reimbursement rates, or more limiting treatment restrictions on behavioral health services than they apply to comparable physical health services. For behavioral health providers, this law is a direct tool in contract negotiations. If a payer’s contract terms for behavioral health services are out of line with how they treat other specialties, that is a parity violation, and it can be raised explicitly during negotiations.
Antitrust law deserves attention because it is frequently misunderstood. The short version: competing providers generally cannot negotiate collectively with payers unless they are part of a qualifying integrated arrangement. Independent providers who agree among themselves on the rates they will accept from a payer are engaging in price-fixing, which violates federal antitrust law and can draw scrutiny from the FTC and the DOJ. That said, there are legitimate structures, including Independent Practice Associations and Accountable Care Organizations, that allow providers to contract jointly under certain conditions. If you are considering any kind of group contracting arrangement, getting proper legal guidance before moving forward is not optional.
The Affordable Care Act reinforced network adequacy requirements, meaning payers that offer plans through the marketplace must maintain networks that include enough providers to give enrollees reasonable access to care. When a payer’s network is thin in a particular specialty or geography, that is a leverage point. A provider who fills a genuine network gap has more room to negotiate than one entering a market where the payer already has plenty of options.
ERISA affects employer-sponsored health plans in ways that sometimes limit what state laws can do. Self-funded employer plans, which are governed by ERISA rather than state insurance regulation, are generally not subject to state insurance mandates. This matters in contract negotiations because the rules that apply to a fully insured commercial plan may not apply the same way to a self-funded plan administered by the same insurer.
State Laws That Shape the Negotiating Table
State-level rules are where things get more specific, and where providers in different parts of the country can have very different experiences with the same payer.
Here are some of the most impactful categories of state regulation to be aware of:
- Any Willing Provider laws require payers to accept any provider who meets their credentialing standards into their network, rather than selectively excluding providers for competitive or administrative reasons. Not every state has these laws, and the scope varies among those that do. If your state has one, it can remove a significant barrier to network participation.
- Prompt payment laws set deadlines for how quickly payers must process and pay clean claims. Most states have these laws, and the required timeframes typically range from 15 to 45 days for electronic claims. When a payer consistently pays outside those windows, they are in violation of state law, and that is something that can be raised both during negotiations and through the state insurance commissioner if the problem persists.
- State balance billing protections set rules around what providers can collect from patients when there is a gap between billed charges and payer reimbursement. Some states have enacted their own balance billing laws that go beyond the federal No Surprises Act. Knowing your state’s rules here affects how you structure your contracts and what you can realistically collect.
State prior authorization reform laws are also worth watching closely. Several states have passed legislation in recent years requiring payers to respond to prior authorization requests within specific timeframes, limiting the types of services that require prior authorization, or requiring gold-carding provisions for providers with strong approval histories. These rules reduce administrative burden and can be referenced when negotiating contract terms around prior authorization requirements.
Using the No Surprises Act IDR Process as a Negotiating Tool
 The Independent Dispute Resolution process is worth a closer look because providers are not using it as much as they could be. When an out-of-network claim is disputed, either party can initiate IDR within a specific window after the payer’s initial payment offer. An independent arbitrator then selects between the provider’s offer and the payer’s offer, using the qualifying payment amount as a benchmark.
The Independent Dispute Resolution process is worth a closer look because providers are not using it as much as they could be. When an out-of-network claim is disputed, either party can initiate IDR within a specific window after the payer’s initial payment offer. An independent arbitrator then selects between the provider’s offer and the payer’s offer, using the qualifying payment amount as a benchmark.
The practical impact on rate negotiations is real. Payers are aware that providers now have a formal process for challenging low payment amounts, and that awareness has shifted some of the leverage in out-of-network payment conversations. Providers who document their costs and market rates carefully are better positioned to use IDR effectively and to reference it as an alternative when in-network negotiations stall.
Common mistakes in the IDR process include missing the filing window, submitting without adequate cost and market rate documentation, and initiating IDR for claims that do not qualify under the statute. Getting those details right before filing matters.
Antitrust Rules: What Providers Often Get Wrong
The antitrust issue comes up often enough that it deserves its own straightforward explanation. The FTC and the DOJ have both published guidance specific to healthcare, and the core rule is not hard to state. Competing providers cannot agree on prices or contract terms with payers. Doing so is price-fixing regardless of the intent behind it.
What providers sometimes get confused about is the range of legitimate structures that do allow joint contracting. Integrated arrangements where providers share financial risk, such as ACOs with shared savings agreements, can negotiate jointly under safe harbor provisions. IPAs can do the same under certain conditions. The key factors are integration, risk sharing, and proportionality of the joint arrangement to the integration involved.
If you are part of a group practice negotiating on behalf of employed or contracted providers within that practice, antitrust is generally not an issue. The concern arises when independent competing providers try to coordinate their positions without the kind of integration that justifies joint contracting.
Mental Health Parity: An Underused Negotiation Tool
 Behavioral health providers leave real leverage on the table by not raising parity issues during contract negotiations. The Mental Health Parity and Addiction Equity Act has been on the books for years, and its 2024 final rule strengthened enforcement requirements for payers. Payers are now required to conduct comparative analyses of the limitations they impose on behavioral health benefits versus medical and surgical benefits, and those analyses have to be made available upon request.
Behavioral health providers leave real leverage on the table by not raising parity issues during contract negotiations. The Mental Health Parity and Addiction Equity Act has been on the books for years, and its 2024 final rule strengthened enforcement requirements for payers. Payers are now required to conduct comparative analyses of the limitations they impose on behavioral health benefits versus medical and surgical benefits, and those analyses have to be made available upon request.
If a payer’s contract terms for behavioral health include lower reimbursement rates, more restrictive prior authorization requirements, or shorter treatment limits than what they apply to comparable medical services, that is a parity problem. Raising it during negotiations, with documentation, puts the payer on notice and opens a different kind of conversation about contract terms than a purely rate-based discussion.
FAQs: Federal and State Rules for Payer Contract Negotiation
- Are payers legally required to negotiate contracts with providers?
Not in most cases. Payers generally have the right to decide which providers to include in their networks, with some exceptions in states with any willing provider laws. However, payers are required to follow specific rules during the contracting process, including network adequacy standards, prompt payment obligations, and parity requirements. - Can a payer change contract terms without a provider’s consent?
This depends on the contract language. Many payer contracts include unilateral amendment clauses that allow payers to modify certain terms with advance notice, without requiring the provider’s signature. Reviewing and negotiating these clauses before signing is important, because they can significantly affect your rights after the contract is in place. - What is a prompt payment law and what happens when a payer violates it?
Prompt payment laws require payers to pay clean claims within a specific timeframe, typically ranging from 15 to 45 days for electronic submissions depending on the state. When payers violate these laws, providers can file complaints with the state insurance commissioner, and some states impose interest penalties on late payments. - How does the No Surprises Act affect in-network contract negotiations?
The No Surprises Act primarily governs out-of-network billing, but it has influenced in-network negotiations by giving providers a formal dispute resolution alternative when payment terms fall too far below market rates. Payers are more aware that providers have recourse, which has shifted some of the dynamic in negotiations. - Can providers negotiate payer contracts as a group without violating antitrust law?
It depends on the structure. Independent competing providers generally cannot negotiate collectively without violating antitrust law. However, integrated arrangements such as ACOs and IPAs that meet specific criteria can negotiate jointly under federal safe harbors. Legal guidance is strongly recommended before entering any group contracting arrangement. - How do I know if my payer contract violates mental health parity requirements?
Request the payer’s comparative analysis under the Mental Health Parity and Addiction Equity Act. Compare the limitations imposed on behavioral health benefits against the terms applied to comparable medical and surgical benefits. If behavioral health services face more restrictive requirements, that is a parity issue worth raising formally. - What should I do if a payer refuses to negotiate contract terms?
Document the refusal in writing and review what state and federal protections may apply to your situation. In some states, payers are required to participate in good-faith negotiations. Filing a complaint with your state insurance commissioner is an option when a payer is acting in bad faith or violating specific regulatory requirements.
Providers also Ask
- How often do state payer contracting laws change? State laws in this area change regularly, particularly around prior authorization reform, balance billing protections, and network adequacy requirements. Staying current means monitoring your state legislature’s activity, subscribing to state medical association updates, and reviewing contracts at least annually against any new requirements.
- What is an any willing provider law? An any willing provider law requires payers to admit any provider who meets their credentialing standards into their network, rather than closing the network selectively. These laws exist in some states and can be a significant tool for providers who have been excluded from networks without a qualification-based reason.
- Does ERISA affect my payer contract negotiations? It can. Self-funded employer health plans governed by ERISA are generally not subject to state insurance mandates, which means some state-level provider protections may not apply when you are contracting with or disputing payments from an ERISA-governed plan. Knowing whether a plan is fully insured or self-funded affects which rules apply.
- When should a provider involve a healthcare attorney in contract negotiations? Any time a contract includes unusual language around unilateral amendments, retroactive claim adjustments, or broad termination clauses, legal review is worth the investment. The same applies when a provider is considering group contracting arrangements, dealing with a payer acting in bad faith, or facing a contract termination they want to challenge.
Know the Rules Before You Negotiate
 Federal and state payer contracting rules are not just legal fine print. They are active tools that shift negotiating power when providers know how to use them. The No Surprises Act IDR process, mental health parity requirements, prompt payment laws, and antitrust safe harbors all have direct implications for what you can demand at the table and how you can respond when a payer pushes back.
Federal and state payer contracting rules are not just legal fine print. They are active tools that shift negotiating power when providers know how to use them. The No Surprises Act IDR process, mental health parity requirements, prompt payment laws, and antitrust safe harbors all have direct implications for what you can demand at the table and how you can respond when a payer pushes back.
The providers who get the best contract terms are not always the highest-volume practices. They are the ones who show up prepared, know their rights, and have support that knows the process inside and out.
At Medwave, we work with healthcare providers across the country on payer contracting, rate negotiations, medical billing, and credentialing. We know how these rules apply in real negotiations, and we know how to use them on our clients’ behalf. If your contracts have not been reviewed recently or you are heading into a negotiation and want experienced support behind you, reach out to our team today.
COO & Co-Founder. Over 30 years of experience, in areas of digital marketing, product creation, and operations.