A medical claim appeal letter is a formal written request to an insurance payer asking them to reverse a claim denial. When prepared correctly, appeals succeed at a meaningful rate. Industry data consistently shows that 40% to 60% of denied claims that go through a formal appeal are overturned, depending on the payer and denial reason. The problem is that most practices never file one. They write off the denial and absorb the revenue loss instead.
The outcome of an appeal depends almost entirely on preparation. A letter that restates the original billing information without adding new evidence or clinical justification is unlikely to succeed. A letter that directly addresses the denial reason, references the applicable payer policy by name, and attaches supporting documentation gives the reviewer a clear basis for reversal.
This article covers the components of an effective appeal letter, how to match your approach to the specific denial code, the documentation that most commonly tips an appeal in the provider’s favor, and the timelines you cannot miss if you want the appeal to be considered at all.
TL;DR
- Most denied claims can be appealed, and many are overturned when the appeal is thorough and timely.
- Knowing the exact denial reason before you write is non-negotiable.
- Documentation is what wins appeals, not persuasive writing alone.
- Missing the filing deadline is the most common and most avoidable reason an appeal fails before it starts.
- A first-level denial isn’t the end. Second-level appeals and external reviews are also available options.
- Medwave handles denial management, billing, credentialing, and payer contracting for practices of all sizes.
What is a Medical Claim Appeal Letter?
 A medical claim appeal letter is a formal written request asking an insurance payer to reconsider a claim it previously denied or underpaid. It’s your opportunity to present evidence, correct errors, and make the case for why the claim should be paid.
A medical claim appeal letter is a formal written request asking an insurance payer to reconsider a claim it previously denied or underpaid. It’s your opportunity to present evidence, correct errors, and make the case for why the claim should be paid.
Most payers have a multi-level appeals process. A first-level appeal goes back to the payer’s internal review team. If that’s denied, a second-level appeal escalates to a more senior review. Beyond that, an external review by an independent organization is often available, particularly for medical necessity disputes. Each level has its own deadline and submission requirements, and those vary by payer.
The appeal letter is not a complaint. It’s a business document, and it should read like one.
Why Claims Get Denied
Before you can write an effective appeal, you have to know why the claim was denied. The denial reason code on the Explanation of Benefits or remittance advice is your starting point. Generic appeals that don’t address the specific denial reason almost always fail.
The most common denial categories include:
- Missing or incorrect patient information, such as a wrong date of birth, member ID, or policy number
- Prior authorization that wasn’t obtained before the service was rendered
- Services the payer deemed not medically necessary based on its own coverage criteria
- Duplicate claim submissions where the payer believes the service was already billed
- Timely filing violations where the claim was submitted after the payer’s deadline
- Coding errors, including mismatched diagnosis and procedure codes or use of an incorrect modifier
Each of these requires a different approach in an appeal. A timely filing denial needs proof of original submission. A medical necessity denial needs clinical documentation. An authorization denial may need a retroactive authorization request alongside the appeal. Knowing which bucket your denial falls into changes everything about how you respond.
Before You Write, What to Pull Together Firstly
The most common reason appeals fail isn’t that the practice had a weak argument. It’s that the appeal was submitted without the documentation needed to back it up. Collecting the right materials before you draft the letter saves time and significantly improves your odds.
Here’s what to gather before writing a single sentence:
- The original claim and all supporting clinical documentation submitted with it
- The denial notice, including the specific reason code and any payer explanation
- The patient’s insurance card, policy documents, or relevant payer contract language
- Prior authorization records, if applicable
- Operative reports, clinical notes, lab results, or any medical records that support the service billed
- CPT and ICD-10 coding guidelines, and the payer’s own coverage policy for the service in question
That last item is particularly important. Payers publish coverage policies for specific services. If the payer denied a claim based on its own medical necessity criteria, reviewing that policy document lets you address the denial on its own terms, citing the specific language the payer used and explaining why your clinical documentation meets it.
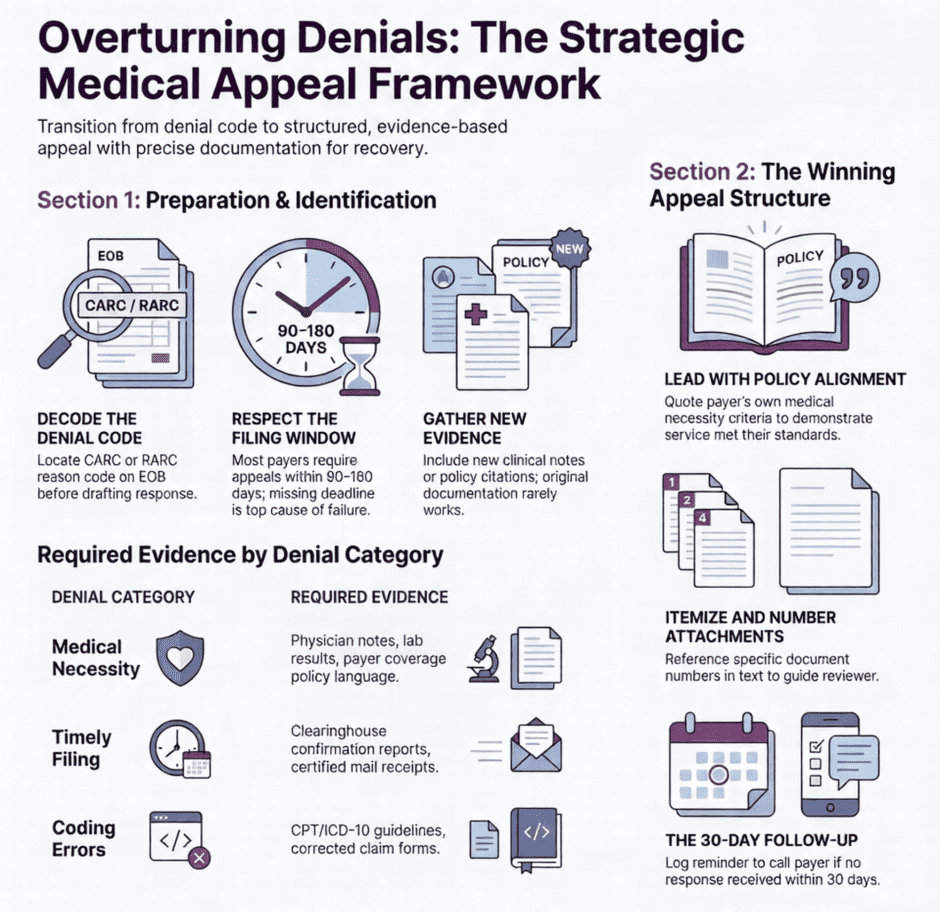
How to Structure the Appeal Letter
Structure matters. An appeal letter that buries the key argument on page three, or that reads like a stream of consciousness, is harder for a reviewer to act on. A clean, logical structure tells the reviewer exactly what happened, why the denial was incorrect, and what you’re asking them to do about it.
1. Header and Reference Information
Start with identifying information so the reviewer can locate the claim without any back-and-forth. Include the date of the letter, the provider’s name and NPI, the patient’s name, date of birth, and member ID, the claim number and date of service, and the payer’s appeals department address or fax number.
2. Opening Statement
State clearly and immediately that this is a formal appeal of a denied claim. Reference the denial date and the reason code. Keep it short. Two sentences is enough. You’re not summarizing the whole argument here. You’re establishing the purpose of the letter.
3. The Core Argument
This is where you explain what was billed, why it was medically appropriate, and why the denial was incorrect. Be specific. If the payer denied for medical necessity, cite the clinical evidence that supports the service. If the payer misapplied a billing rule, cite the applicable CPT guideline or payer policy language. Quote their own policy back to them when they’ve misread or misapplied it.
Don’t assert that the claim should be paid. Demonstrate it.
4. Documentation List
Itemize every document attached to the appeal. Number the attachments and reference them in the body of the letter. “As shown in Attachment 2, the operative report confirms…” is far more effective than asking the reviewer to guess which document supports which argument.
5. Closing and Request
End with a clear, specific request. Are you asking for payment in full? A partial reconsideration? A peer-to-peer review with the medical director? State it plainly. Include a deadline reference if the payer has a response obligation under state law or their own policy. Provide a direct contact name and number for follow-up questions.
Step-by-Step: Writing the Appeal
- Pull the EOB or remittance advice and identify the exact denial reason code before doing anything else.
- Look up the payer’s appeals policy. Note the filing deadline, required submission format, and the correct address or fax number for appeals. Missing any of these details can disqualify the appeal before anyone reads it.
- Gather all supporting documentation. Do not start writing until everything is in hand.
- Draft the letter in a professional, factual tone. Avoid frustration language. Words like “outrageous” or “clearly wrong” don’t help your case and can make reviewers defensive.
- Attach documentation in a logical order that mirrors the argument in the letter.
- Submit using the payer’s required method, whether that’s a portal, fax, or certified mail. Log the submission date and keep a copy of everything.
- Set a 30-day follow-up reminder. If the payer hasn’t responded within their required timeframe, you have the right to escalate.
Mistakes That Get Appeals Denied Again
 A lot of appeals fail not because the underlying claim was wrong, but because the appeal itself had avoidable problems. These are the ones we see most often.
A lot of appeals fail not because the underlying claim was wrong, but because the appeal itself had avoidable problems. These are the ones we see most often.
Missing the filing deadline is the single most common failure. Most payers require appeals within 90 to 180 days of the denial date. Some are shorter. Once that window closes, your options are extremely limited.
Submitting the same documentation that was on the original claim without adding anything new is also a frequent mistake. If the original documentation wasn’t sufficient to get the claim paid, sending it again without additional support gives the reviewer no new reason to change the decision.
Using vague language instead of citing specific policy or coding guidelines weakens the argument considerably. “This service was medically necessary” without clinical evidence to back it is not an argument. It’s a statement.
Sending to the wrong department or using the wrong submission method can result in the appeal being logged incorrectly or not logged at all. Always verify the exact submission instructions from the payer’s appeal policy before you send anything.
Not following up is the final mistake. Appeals can sit in queues for weeks. A proactive follow-up call, logged with the date and the name of the representative, demonstrates that you’re tracking the appeal and holds the payer accountable to their response timeline.
Tips for Writing a More Persuasive Appeal
Lead with your strongest piece of evidence. Don’t build to it. Reviewers process high volumes of appeals, and a letter that opens with the most compelling argument is more effective than one that saves it for the third paragraph.
For medical necessity denials, clinical documentation does the heavy lifting. Physician notes that directly address the payer’s coverage criteria, written in specific terms rather than general ones, are far more persuasive than a summary statement.
For high-dollar denials, consider requesting a peer-to-peer review between your treating physician and the payer’s medical director. This is a separate step from the formal written appeal, but it can be particularly effective for complex procedures or off-label treatment decisions where the clinical rationale benefits from a direct conversation.
Keep the letter focused. A well-argued two-page appeal is more effective than a five-page letter that covers every possible angle. Make your case, support it with documentation, and ask for what you need.
What to Know About Second-Level Appeals and External Reviews
 If a first-level appeal is denied, the process isn’t over. Most payers offer a second-level internal appeal that goes to a more senior review panel. Beyond that, external reviews conducted by an independent organization are available for many denial types, particularly medical necessity disputes.
If a first-level appeal is denied, the process isn’t over. Most payers offer a second-level internal appeal that goes to a more senior review panel. Beyond that, external reviews conducted by an independent organization are available for many denial types, particularly medical necessity disputes.
External reviews are governed by state law and, for self-funded employer plans, by federal rules under the ACA. The payer is generally required to abide by the external reviewer’s decision. For significant denials where the internal process has been exhausted, external review is worth pursuing.
Denied Claim Appeal FAQ
- How long do I have to appeal a denied insurance claim?
It depends on the payer. Most commercial payers require appeals within 90 to 180 days of the denial date. Medicare has specific timelines that vary by appeal level. Always check the payer’s appeal policy before you assume you still have time. - Can I appeal a claim that was denied for timely filing?
Yes, but the bar is higher. Timely filing appeals typically require proof that the original claim was submitted on time, such as a clearinghouse confirmation report, a certified mail receipt, or a payer portal submission log. Without that evidence, timely filing denials are very difficult to overturn. - What should I do if my first appeal is denied?
File a second-level appeal if the payer offers one, and request the specific reason the first appeal was denied. You may also be eligible for an external review, depending on the denial type and the payer. Don’t treat a first-level denial as the final answer. - Does every denied claim need an appeal letter?
Not necessarily. Some denials are better resolved through a corrected claim submission, a billing correction, or a retroactive authorization request. Read the denial reason carefully. If the claim was denied due to a data entry error, correcting and resubmitting is typically faster than filing a formal appeal. - Should I request a peer-to-peer review before filing a formal appeal?
For medical necessity denials, yes, it’s worth considering. A peer-to-peer review allows your physician to speak directly with the payer’s medical director and explain the clinical rationale. This step sometimes resolves the denial faster than going through the formal written appeal process. - How long does the payer have to respond to an appeal?
This varies by state law and payer policy. Most commercial payers are required to respond to standard appeals within 30 to 60 days. Urgent or expedited appeals generally require a faster response. Check your state’s insurance regulations for specific timelines that apply in your market.
Providers also Ask
- What is the success rate for medical claim appeals?
Industry estimates vary, but many sources suggest that 40% to 60% of appealed claims are ultimately paid when the appeal is properly documented and submitted on time. The rate is significantly lower for appeals that rely only on the original documentation without adding new supporting evidence. - Can a provider file an appeal on behalf of a patient?
Yes. Providers file appeals on behalf of patients routinely, particularly when the denial affects the provider’s reimbursement for services already rendered. The authorization process varies by payer, and some require a signed authorization from the patient. - What happens if an insurance company ignores an appeal?
Most payers are bound by state law or federal regulations to respond within a set timeframe. If a payer doesn’t respond, you can escalate by filing a complaint with your state’s department of insurance, contacting your provider relations representative, or requesting external review. - What is the difference between a reconsideration and a formal appeal?
A reconsideration is an informal request to review a claim again, often used when the denial resulted from a minor error or missing information. A formal appeal is a structured process governed by the payer’s appeal policy, with specific deadlines, documentation requirements, and escalation rights. Formal appeals carry more protections for the provider. - How do I find out exactly why my claim was denied?
Start with the Explanation of Benefits or the remittance advice. The denial reason code, along with the Claim Adjustment Reason Code (CARC) and Remittance Advice Remark Code (RARC), tells you specifically why the claim was rejected. If the code isn’t clear, calling the payer’s provider services line for an explanation is a reasonable next step before drafting an appeal.
Summary: Denial Management Process (Medical Claim Appeals )
 Denial management is one of the most time-consuming parts of running a medical practice, and it’s an area where having experienced support makes a measurable difference. Denial management is a core part of what our billing team does on behalf of our clients.
Denial management is one of the most time-consuming parts of running a medical practice, and it’s an area where having experienced support makes a measurable difference. Denial management is a core part of what our billing team does on behalf of our clients.
We track denial patterns by payer, identify root causes, handle appeal submissions, and follow up until claims are resolved. If your practice is spending hours on denied claims each month or writing off denials that should be overturned, that’s worth a conversation.
Practices that outsource denial management to a dedicated billing partner typically see faster resolution times, higher overturn rates, and a clearer picture of which payers are causing the most friction. Over time, that data becomes just as valuable as the recovered revenue itself. It reveals where your billing process needs to be tightened and where payers may need to be held more accountable. Getting ahead of denials is always more efficient than chasing them.
COO & Co-Founder. Over 30 years of experience, in areas of digital marketing, product creation, and operations.

