A physician credentialing application requires documents from every stage of a provider’s career. The medical school transcripts, residency completion certificates, state licenses, DEA registration, malpractice insurance declarations, board certifications, and a gap-free work history. Gathering those documents takes longer than most providers expect. Medical schools and licensing boards that still operate on paper can take four to eight weeks to produce official copies. Starting the documentation process at least 90 days before submitting an application is the single most effective way to prevent timeline delays.
This checklist covers every document category required for physician credentialing, organized by how long each typically takes to obtain.
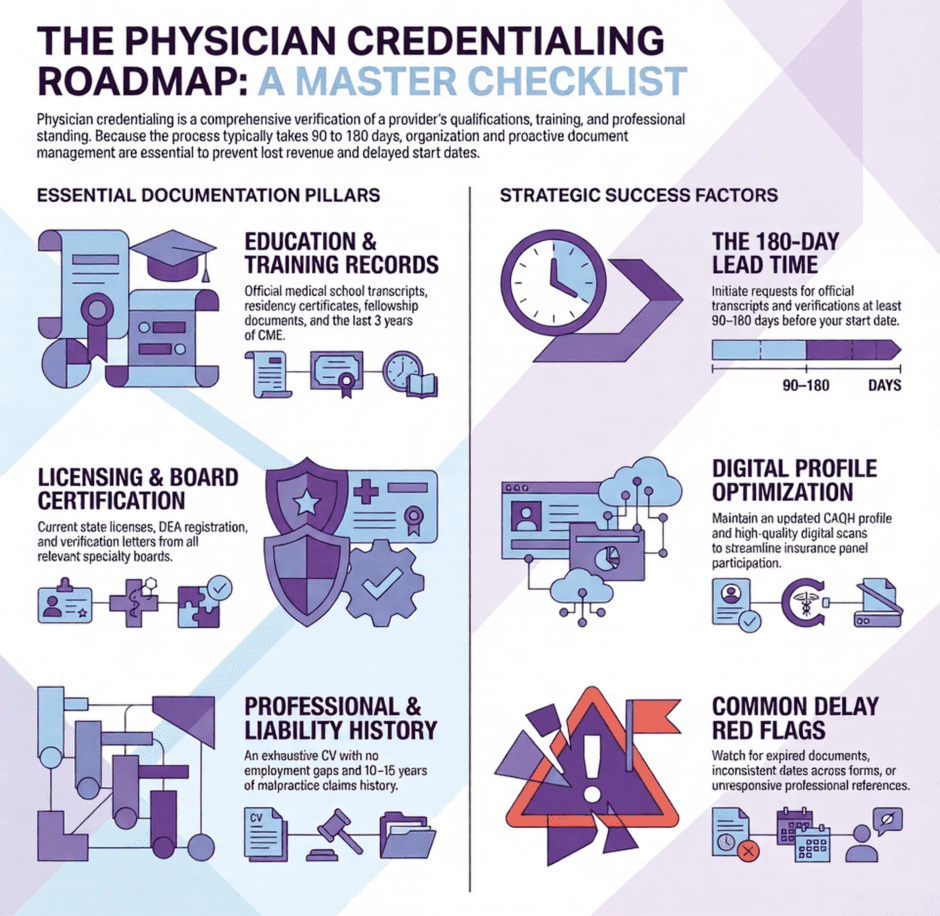
What’s Physician Credentialing?
 Physician credentialing is the process healthcare organizations and insurance payers use to verify that a provider holds the qualifications they claim, including medical school degrees, residency training, board certifications, active state licenses, malpractice coverage, and a complete professional work history. Without active credentialing, a physician cannot admit patients to most hospitals or bill insurance companies for services.
Physician credentialing is the process healthcare organizations and insurance payers use to verify that a provider holds the qualifications they claim, including medical school degrees, residency training, board certifications, active state licenses, malpractice coverage, and a complete professional work history. Without active credentialing, a physician cannot admit patients to most hospitals or bill insurance companies for services.
The process exists to protect patients, reduce liability for healthcare organizations, and ensure that only qualified physicians provide care. While it might seem tedious, credentialing serves a crucial purpose in maintaining healthcare quality standards.
The Core Documentation You’ll Need
Before diving into specific checklists, let’s talk about the fundamental documents that virtually every credentialing process requires. Having these ready from the start will dramatically speed up your application.
Personal and Professional Information:
- Current CV or resume
- Copy of driver’s license or government-issued ID
- Social Security card
- Birth certificate (certified copy)
- Immigration documentation (if applicable)
Your CV or resume deserves special attention here. Unlike a typical resume, your credentialing resume needs to be exhaustively detailed. Include every position you’ve held, every gap in employment explained, and complete contact information for all references. Any unexplained gaps will trigger follow-up questions that slow down the process.
Education and Training Documentation
This section often trips up physicians because it requires reaching back to institutions you may have attended decades ago. Start gathering these documents early because obtaining them can take weeks or even months.
- Medical school diploma and transcripts – Must be official copies sent directly from the institution
- Residency completion certificates – Include all residency programs, even if you switched
- Fellowship certificates – Don’t forget any additional subspecialty training
- Continuing Medical Education (CME) transcripts – Typically need the last two to three years
Many institutions now offer online transcript request portals, but some medical schools and licensing boards still require written requests and take four to eight weeks to respond. Requesting these documents at least 90 days before the application submission date prevents the most common documentation delay.
Licensing and Board Certification
Your state medical licenses form the backbone of your credentialing package. You’ll need current licenses for every state where you plan to practice, plus documentation of any licenses you’ve held previously, even if they’ve expired.
Required licensing documents include:
- Current state medical license (all states)
- License verification from each state medical board
- DEA registration certificate
- Controlled substance licenses (state-specific)
Board certification adds another layer of complication. You’ll need certificates from all relevant specialty boards, verification letters, and in some cases, documentation of your board maintenance activities. If you’re board-eligible but not yet certified, make sure you have documentation of your timeline for taking the exam.
Malpractice Insurance and Claims History
Malpractice history documentation is the section that generates the most follow-up requests from credentialing committees. You’ll need to provide detailed information about your malpractice coverage and any claims history, even if cases were dismissed or settled without admission of wrongdoing.
Most credentialing applications require:
- Current malpractice insurance policy declarations page
- Claims history for the past 10-15 years (varies by organization)
- Detailed explanations for any claims, including outcomes
- Coverage amounts and policy periods for all previous insurance
When describing malpractice claims, be factual and concise. Provide the required information without over-explaining or becoming defensive. Remember, most physicians have faced some form of malpractice claim during their careers, so having claims doesn’t automatically disqualify you.
Work History and References
Your employment history needs to be complete and verifiable.
This means providing detailed information about every position you’ve held since medical school, including:
- Exact dates of employment
- Complete contact information for supervisors
- Detailed job descriptions
- Reasons for leaving each position
Reference requirements typically include:
- Department chairs or medical directors from recent positions
- Colleagues who can speak to your clinical competence
- Professional references (typically 3-5 people)
- Personal references (usually 2-3 non-family members)
Choose references strategically. Select people who know your work well and can speak enthusiastically about your skills and character. Give your references advance notice and provide them with a copy of your CV or resume so they’re prepared for reference calls.
Hospital Privileges and Peer Review
If you’ve practiced at other hospitals, you’ll need to provide documentation of your privileges and any peer review activities.
This includes:
- Copies of medical staff bylaws acknowledgments
- Privilege delineation forms
- Peer review summaries (if available)
- Disciplinary actions (if any)
- Voluntary resignations or non-renewals
Be particularly careful about explaining any situations where you resigned from a medical staff or had privileges restricted. Provide context and documentation to support your version of events.
Specialized Requirements by Practice Setting
Different healthcare settings have unique credentialing requirements that go beyond the standard documentation.
For hospital employment:
- Medical staff application
- Delineation of privileges forms
- Department-specific requirements
- Joint Commission compliance documentation
For health system positions:
- System-wide credentialing applications
- Multi-state licensing requirements
- Telemedicine credentialing (increasingly common)
For insurance panel participation:
- CAQH profile (keep this updated continuously)
- Plan-specific applications
- Fee schedule agreements
- Network participation agreements
The Technology Component
Most credentialing processes now involve online portals and digital document submission. While this can speed things up, it also creates new potential pitfalls.
Make sure your documents are high-quality scans, properly labeled, and in the correct file formats. Many systems have size limitations or specific format requirements that can cause delays if not followed precisely.
Timeline Management and Follow-Up
Physician credentialing typically takes 90-180 days, sometimes longer. Planning ahead is crucial, especially if you’re counting on a specific start date for financial reasons.
Create a tracking system for your applications.
Use a spreadsheet or project management tool to monitor:
- Application submission dates
- Document requirements and status
- Follow-up deadlines
- Contact information for credentialing coordinators
Red flags that indicate potential delays:
- Requests for additional documentation after initial submission
- Long periods without communication from credentialing staff
- References reporting they haven’t been contacted
- Technical issues with online portals
Don’t hesitate to follow up proactively. A polite check-in every two weeks shows you’re engaged without being pushy.
Common Mistakes That Cause Delays
Learning from others’ mistakes can save you significant time and frustration.
Here are the most frequent issues that slow down credentialing:
- Incomplete applications – Double-check every field before submitting. Empty required fields will bounce your application back to square one.
- Expired documents – Monitor expiration dates on licenses, certifications, and insurance policies. Some organizations require documents to be valid for a specific period beyond your start date.
- Inconsistent information – Make sure dates, names, and other details match across all documents. Discrepancies trigger verification delays.
- Poor reference management – Choose references who will respond promptly and provide thorough feedback. Brief, generic responses can raise red flags.
Making the Process Work for You
![]()
While you can’t control every aspect of credentialing, you can optimize your approach to minimize delays and stress. Treat credentialing as an ongoing career management activity rather than a one-time hurdle.
Maintain an updated credentialing file throughout your career. When you complete CME courses, update your malpractice insurance, or change addresses, update your master file immediately. This proactive approach makes future credentialing applications much easier.
Consider working with credentialing consultants or services if you’re managing multiple applications simultaneously. While there’s a cost involved, the time savings and reduced stress often justify the expense, especially for physicians establishing new practices or joining large health systems.
Stay organized, be proactive with follow-up, and don’t let the bureaucracy discourage you.
Co-Founder and COO of Medwave, bringing more than 30 years of hands-on experience in healthcare revenue cycle management, payer contracting, and medical credentialing.

