Verification of Benefits, commonly called VOB, is the process of checking a patient’s insurance coverage before they receive medical services. Think of it as calling ahead to confirm a reservation at a restaurant. You want to make sure everything is in order before you show up.
When healthcare providers verify benefits, they contact the insurance company to confirm what services are covered, how much the patient will need to pay, and whether any special requirements need to be met. This simple step can prevent billing headaches and surprise bills down the road.
The VOB process typically happens after a patient schedules an appointment but before they arrive at the office. Medical billing staff or front desk personnel reach out to the insurance carrier to gather critical information about the patient’s plan.
Why Does VOB Matter for Healthcare Providers?
 Getting paid for services is the backbone of any medical practice. Without proper verification, providers risk delivering care that insurance won’t cover, leaving them to chase payments or write off charges entirely.
Getting paid for services is the backbone of any medical practice. Without proper verification, providers risk delivering care that insurance won’t cover, leaving them to chase payments or write off charges entirely.
VOB protects the financial health of a practice in several ways. First, it reduces claim denials. When you know exactly what’s covered before the appointment, you can code and bill correctly the first time. Second, it speeds up payment. Clean claims that match verified benefits get processed faster by insurance companies. Third, it helps practices maintain steady cash flow by reducing the time between service and payment.
Beyond the money, VOB also builds trust with patients. When you can tell someone upfront what their visit will cost, they appreciate the transparency. Nobody likes surprise medical bills, and verification helps eliminate that unpleasant experience.
What Information Does VOB Provide?
A thorough verification of benefits gives you a detailed picture of a patient’s coverage.
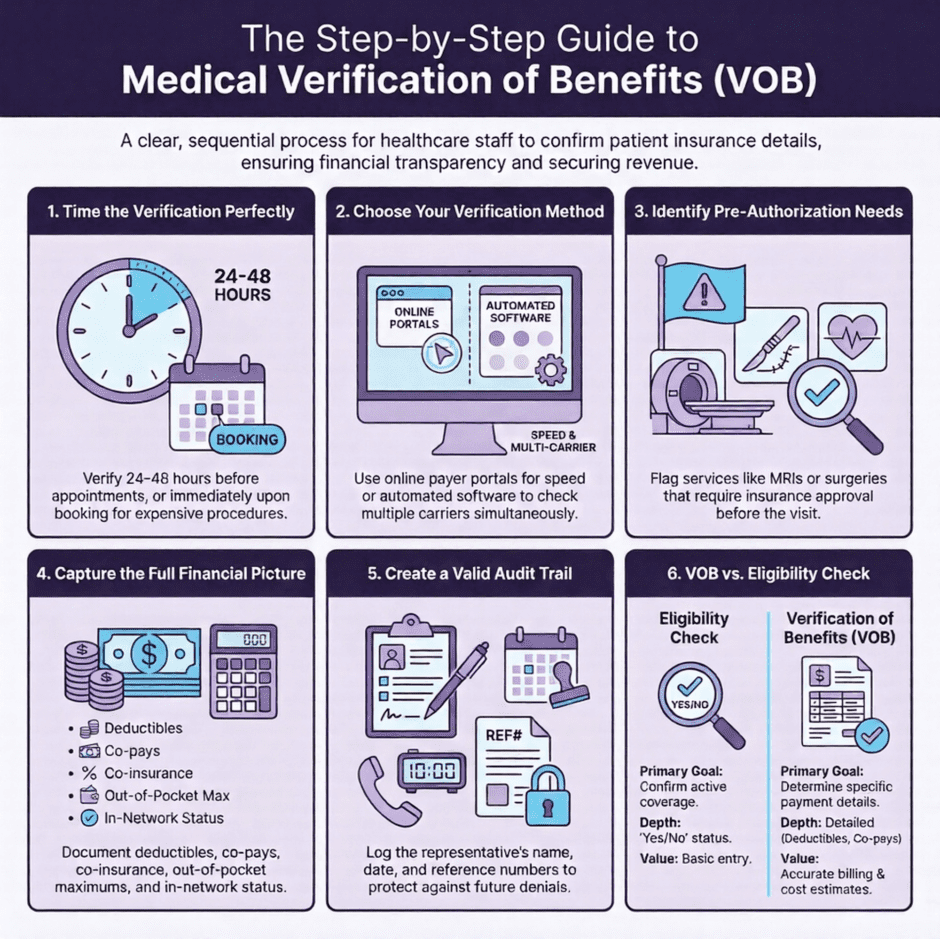
Here’s what you should gather during the process:
- Active coverage status and policy effective dates
- Deductible amounts and how much has been met
- Co-payment amounts for office visits and procedures
- Co-insurance percentages
- Out-of-pocket maximums
- Specific coverage for planned services
- Pre-authorization or referral requirements
- In-network vs. out-of-network benefits
- Limitations or exclusions on certain treatments
Each piece of information plays a role in determining what the patient owes and what the insurance will pay. The deductible tells you if the patient needs to pay in full until they reach a certain amount. Co-pays are fixed fees for visits. Co-insurance is a percentage split between the patient and insurer after the deductible is met.
How Do You Perform a Verification of Benefits?
 The VOB process follows a fairly standard pattern, though the details can vary by insurance company. Most providers verify benefits through one of three methods: phone calls, online portals, or electronic verification systems.
The VOB process follows a fairly standard pattern, though the details can vary by insurance company. Most providers verify benefits through one of three methods: phone calls, online portals, or electronic verification systems.
Phone verification involves calling the insurance company directly using the number on the patient’s insurance card. You’ll need to provide the patient’s member ID, date of birth, and sometimes other identifying information. The insurance representative will then share coverage details, which you should document carefully.
Online portals offered by major insurance carriers let you log in and check benefits digitally. This method is faster than phone calls and gives you written confirmation that you can save for your records. Many insurance companies now require providers to use their portals for routine verifications.
Electronic verification systems are software platforms that automatically check benefits across multiple insurance carriers. These systems can verify dozens of patients in the time it takes to make a few phone calls. Many practices use these tools to streamline their workflow.
When Should You Verify Benefits?
Timing matters when it comes to VOB. The ideal window is 24 to 48 hours before a scheduled appointment. This gives you enough time to address any issues but is recent enough that the information remains current.
Verifying too far in advance can backfire. Insurance coverage changes frequently. Patients switch jobs, lose coverage, or modify their plans. Information verified a month ahead might be outdated by the appointment date.
However, certain situations call for earlier verification. If a patient is scheduled for an expensive procedure or surgery, verify benefits as soon as the appointment is booked. This gives you time to handle pre-authorization requirements, which can take days or even weeks for some services.
New patients always need verification. You can’t assume anything about their coverage until you check. Existing patients should have their benefits re-verified at least once per calendar year, as plan details often change during open enrollment periods.
What are Pre-Authorization and Pre-Certification?
 During the VOB process, you might discover that certain services require pre-authorization or pre-certification. These terms are often used interchangeably, though some insurance companies make technical distinctions between them.
During the VOB process, you might discover that certain services require pre-authorization or pre-certification. These terms are often used interchangeably, though some insurance companies make technical distinctions between them.
Pre-authorization is approval from the insurance company before providing a service. The insurer reviews the medical necessity of the proposed treatment and decides whether to cover it. Without this approval, the insurance might deny the claim entirely, leaving the patient or provider stuck with the bill.
Common services that require pre-authorization include MRI scans, CT scans, certain surgeries, specialty medications, and durable medical equipment. Mental health services and physical therapy often need authorization after a certain number of visits.
Getting pre-authorization takes effort. You typically need to submit clinical documentation explaining why the service is medically necessary. The insurance company reviews this information and issues an approval or denial. This process can take anywhere from a few days to several weeks, which is why early verification is so important for these services.
What Happens When Benefits Aren’t Verified?
Skipping VOB creates problems for everyone involved. The most immediate issue is claim denials. If you bill for a service that wasn’t covered or required pre-authorization you didn’t obtain, the insurance company will reject the claim.
Denied claims mean delayed payment. Your practice has already provided the service and incurred the costs, but now you have to spend additional time and resources fixing the claim and resubmitting it. Many denied claims never get paid, especially if the issue is something that can’t be corrected after the fact.
Patients suffer too when benefits aren’t verified. They might receive care thinking insurance will cover it, only to get a large bill weeks later. This damages the patient-provider relationship and can lead to disputes over who is responsible for payment.
From a business perspective, poor VOB practices drain profitability. Staff spend countless hours on the phone with insurance companies trying to resolve billing issues that could have been prevented. Collections become more difficult. Patient satisfaction drops. The practice’s reputation can take a hit.
How Does VOB Differ from Eligibility Checks?
 Many people confuse eligibility checks with verification of benefits, but they’re not quite the same thing. An eligibility check simply confirms that a patient has active insurance coverage on a given date. It’s a yes or no question. Is this person insured?
Many people confuse eligibility checks with verification of benefits, but they’re not quite the same thing. An eligibility check simply confirms that a patient has active insurance coverage on a given date. It’s a yes or no question. Is this person insured?
VOB goes much deeper. It not only confirms eligibility but also reveals the specific details of what that insurance covers. You learn about deductibles, co-pays, coverage limitations, and requirements. Eligibility is the first step, but VOB provides the full picture you need for accurate billing.
An eligibility check tells you someone has a ticket to the concert. VOB tells you where their seat is located, whether they have backstage access, and what they need to do to use their ticket. Both are important, but VOB gives you the actionable information you need.
What Challenges Come with VOB?
Even with the best processes in place, VOB comes with its share of obstacles. Insurance companies don’t make it easy. Each carrier has different procedures, different portals, and different requirements. What works for one insurer might not work for another.
Hold times when calling insurance companies can eat up huge chunks of staff time. Getting through to a representative might take 20 or 30 minutes, and that’s before you even start asking questions. Some practices have staff members who spend entire days just verifying benefits.
Information accuracy is another concern. Insurance representatives sometimes provide incorrect information. Coverage details might be misunderstood or miscommunicated. When you rely on verbal information over the phone, there’s always room for error.
Insurance plans themselves keep getting more complicated. High-deductible plans, tiered networks, and varying coverage levels make it harder to give patients clear answers about what they’ll owe. A patient might be in-network for some services but out-of-network for others, even within the same practice.
How Can Technology Help with VOB?
 Modern technology has made the VOB process significantly easier and more reliable. Automated verification systems can check benefits across dozens of insurance carriers simultaneously, pulling data directly from payer databases.
Modern technology has made the VOB process significantly easier and more reliable. Automated verification systems can check benefits across dozens of insurance carriers simultaneously, pulling data directly from payer databases.
These systems reduce human error and save enormous amounts of time. What once took 15 minutes per patient now takes seconds. The software typically integrates with practice management systems, so verified benefits flow directly into patient records.
Real-time eligibility tools allow front desk staff to check coverage while the patient is on the phone scheduling an appointment. This immediate feedback helps practices set proper expectations and collect accurate demographic information from the start.
Some advanced platforms even provide cost estimates based on verified benefits. They can tell patients approximately what they’ll owe before they arrive for their appointment, which improves collections and reduces surprise bills.
What Role Does VOB Play in Patient Collections?
Verified benefits give you the information you need to collect from patients at the time of service. When you know exactly what someone owes, you can request payment upfront rather than billing them later.
Point-of-service collections are far more efficient than chasing payments after the fact. Patients are already at your office, they’re expecting to pay something, and you have all the information you need to calculate the correct amount. Collection rates are much higher when you ask for payment on the day of service.
VOB also helps you develop payment plans for patients who can’t afford to pay their entire portion upfront. When you know a procedure will cost a patient $1,500 after insurance, you can discuss payment options before the service rather than surprising them with a large bill afterward.
Transparency builds trust. Patients who know what to expect financially are more likely to keep appointments, comply with treatment plans, and maintain a positive relationship with your practice.
How Often Should Benefits Be Re-verified?
 Insurance coverage isn’t static. People change jobs, add or drop dependents, switch plans during open enrollment, and experience life events that affect their coverage. Regular re-verification catches these changes before they cause billing problems.
Insurance coverage isn’t static. People change jobs, add or drop dependents, switch plans during open enrollment, and experience life events that affect their coverage. Regular re-verification catches these changes before they cause billing problems.
At minimum, verify benefits annually for established patients. Many practices choose to verify at the beginning of each calendar year when insurance plans typically renew and change. This catches the updates that happen during open enrollment season.
More frequent verification makes sense for patients with certain types of coverage. Medicaid recipients might experience coverage changes monthly based on income or other factors. Patients with employer-sponsored insurance should be re-verified if you know their company is changing carriers.
Red flags should trigger immediate re-verification. If a claim gets denied due to coverage issues, verify benefits right away before the next appointment. If a patient mentions they’ve changed jobs or insurance, verify before providing services.
What Documentation Should You Keep?
Proper documentation protects your practice if disputes arise about coverage or billing. Every time you verify benefits, document who you spoke with, when you called, what information you received, and any reference numbers provided.
Keep this documentation in the patient’s file for at least as long as you keep other medical records. If an insurance company later denies a claim saying the service wasn’t covered, you can point to your verification notes showing what you were told.
Many practices use standardized forms to record VOB information. This ensures staff members collect all the necessary details and creates consistent records. Digital forms that integrate with your practice management system are even better, as they reduce paperwork and make information easier to retrieve.
Screenshot confirmations from online portals or save PDFs of benefit details. These provide visual proof of what the insurance company’s own system showed at the time of verification.
How Medwave Can Help
 Managing VOB alongside all your other practice responsibilities can feel overwhelming. Between seeing patients, handling administrative tasks, and keeping up with changing regulations, adding thorough benefit verification to your plate might seem impossible.
Managing VOB alongside all your other practice responsibilities can feel overwhelming. Between seeing patients, handling administrative tasks, and keeping up with changing regulations, adding thorough benefit verification to your plate might seem impossible.
Medwave specializes in medical billing, credentialing, and payer contracting. Our team handles the VOB process for practices like yours, ensuring benefits are verified accurately and on time. We stay current with insurance company requirements, navigate their systems efficiently, and document everything properly.
By partnering with a dedicated billing service, you free up your staff to focus on patient care rather than spending hours on hold with insurance companies. You reduce claim denials, speed up payments, and improve your practice’s financial performance.
Summary: What is VOB?
Verification of Benefits isn’t the most exciting part of running a medical practice, but it’s one of the most important. This simple process of checking insurance coverage before appointments prevents denials, speeds up payments, and creates better experiences for patients.
Whether you handle VOB in-house or partner with a billing service, making it a priority pays dividends. Fewer denied claims mean steadier cash flow. Better patient communication means higher satisfaction and collection rates. More accurate billing means less time spent on corrections and appeals.
The key is consistency. Verify every patient, verify thoroughly, document carefully, and stay current with each insurance company’s requirements. When VOB becomes a standard part of your workflow rather than an afterthought, you’ll see the benefits in both your bottom line and your patients’ peace of mind.

