Choosing a credentialing service shouldn’t be difficult, but somehow it is. Dozens of companies claim they can handle your provider enrollment, and on the surface, they all sound pretty similar. They promise to manage your applications, track your status, and get you enrolled with payers. The websites look professional. The sales pitches sound good. So how do you actually tell which ones will deliver and which ones will leave you frustrated?
The difference between a good credentialing service and a mediocre one often doesn’t become clear until you’re already working together. By then, you might be dealing with missed deadlines, poor communication, or application errors that set you back months. The key is knowing what to look for before you sign a contract.
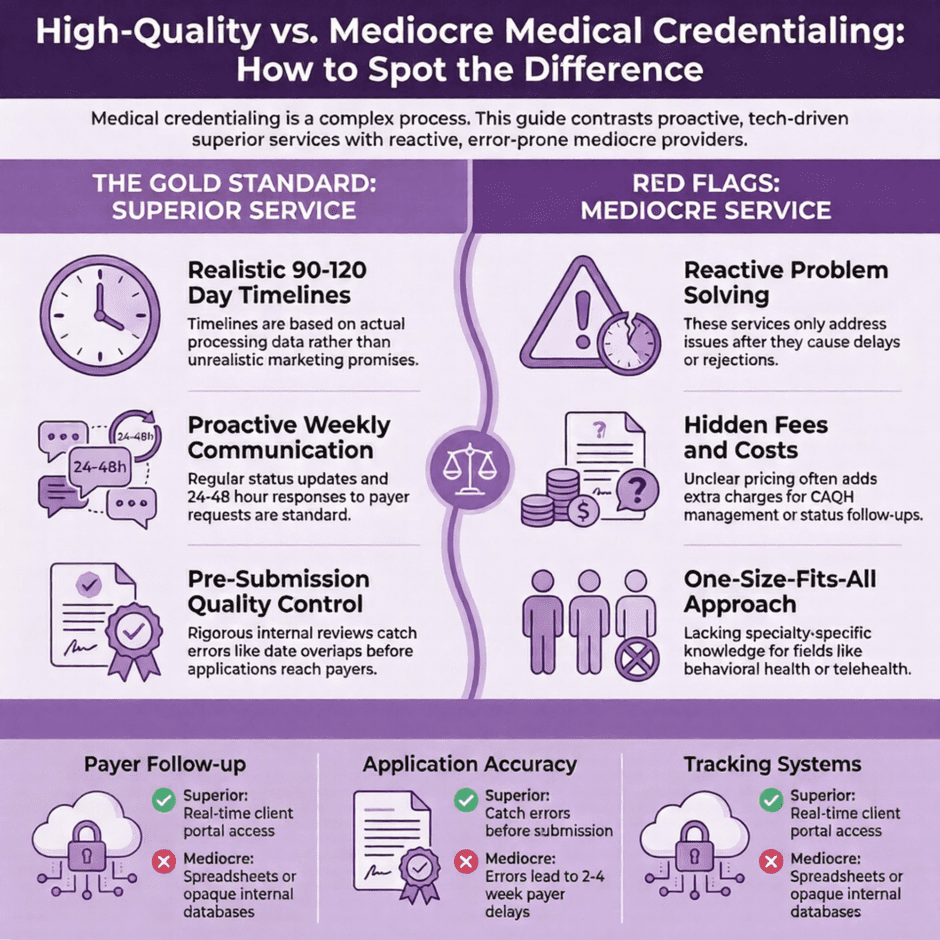
Speed That Actually Matters
 Every credentialing company talks about fast turnaround times. But there’s a big difference between how quickly they process paperwork on their end and how quickly you actually get enrolled and can start billing insurance.
Every credentialing company talks about fast turnaround times. But there’s a big difference between how quickly they process paperwork on their end and how quickly you actually get enrolled and can start billing insurance.
Good credentialing services give you realistic timelines based on actual data, not marketing promises. They’ll tell you that initial credentialing typically takes 90 to 120 days for most commercial payers, longer for some government programs, and they’ll explain what factors affect those timelines. They track their average processing times and share that information with clients.
Bad credentialing services either make unrealistic promises about 30-day credentialing or give you vague answers about timelines. They might process your application quickly on their end but then submit it with errors that cause delays on the payer’s side. The net result is that you’re not enrolled any faster, and you’ve wasted time fixing problems.
Speed also matters in how quickly the service responds to payer requests for additional information. Insurance companies often ask for clarification or extra documentation during the credentialing process. A good service monitors these requests closely and responds within 24 to 48 hours. A mediocre service might take a week or more to even notice the payer asked for something, adding weeks to your timeline.
Communication You Can Count On
The credentialing process involves a lot of waiting. Applications sit with insurance companies for weeks or months. During this time, you need to know what’s happening. Good credentialing services provide regular status updates without you having to ask for them.
This might look like weekly email updates on where each application stands, proactive notifications when payers request additional information, immediate alerts when approvals come through, and a clear point of contact who actually responds when you reach out. You should never be left wondering whether your applications are progressing or stuck somewhere in limbo.
Mediocre services go silent after submitting applications. You email asking for updates and get generic responses like “still processing” without any real information. When payers request additional documentation, you find out weeks later. When problems arise, you’re the last to know.
Communication quality also shows up in how the service explains the credentialing process to you upfront. Good services take time to walk you through what will happen, what you need to provide, what they’ll handle, and what realistic timelines look like. Mediocre services rush through onboarding, assuming you already know how everything works, then act surprised when you have questions later.
Accuracy in Application Submission
 This is where the real difference shows up. Credentialing applications are detailed. They ask for information about education, training, work history, licenses, certifications, malpractice coverage, and more. Every field needs to be filled out correctly, and all documentation needs to match what you’ve stated in the application.
This is where the real difference shows up. Credentialing applications are detailed. They ask for information about education, training, work history, licenses, certifications, malpractice coverage, and more. Every field needs to be filled out correctly, and all documentation needs to match what you’ve stated in the application.
Good credentialing services have quality control processes to catch errors before applications go out. They verify that license numbers match the licenses on file, that date ranges don’t overlap or have gaps that will raise questions, that facility affiliations are current and accurate, and that all required documentation is included and legible.
Mediocre services rush through applications and submit them with mistakes. Common credentialing errors include misspelled names, incorrect license numbers, missing documentation, date inconsistencies, and incomplete employment history. Each error means the payer kicks the application back for corrections, adding 2 to 4 weeks to your timeline.
The frustrating part is that you often don’t know applications were submitted incorrectly until the payer rejects them. By then, you’ve already lost weeks or months. A good credentialing service prevents this through careful review before submission.
Specialty-Specific Knowledge
Not all credentialing is the same. The requirements for credentialing a primary care physician are different from credentialing a physical therapist, which is different from credentialing a behavioral health provider or a home health agency.
Good credentialing services have actual experience with your specific provider type and specialty. They know which payers have special requirements for your field. They know which documentation matters most for your specialty. They know common sticking points and how to address them proactively.
For example, credentialing behavioral health providers often involves additional questions about supervision for licensed clinical social workers or counselors. Credentialing advanced practice nurses requires careful attention to collaborative practice agreements in certain states. Credentialing for telehealth across multiple states brings its own set of requirements.
Mediocre services use a one-size-fits-all approach. They might be great at credentialing one type of provider but have no real experience with your specialty. They miss specialty-specific requirements, submit incomplete applications, and create delays because they’re learning on your dime.
Proactive Problem Solving
 Problems come up during credentialing. A payer might question a gap in your employment history. A reference might not respond quickly. An old malpractice claim might need additional explanation. How the credentialing service handles these situations matters enormously.
Problems come up during credentialing. A payer might question a gap in your employment history. A reference might not respond quickly. An old malpractice claim might need additional explanation. How the credentialing service handles these situations matters enormously.
Good services anticipate common problems and address them before they become issues. If there’s a gap in your work history because you took time off for family reasons or additional training, they proactively include an explanation in the initial application. If a reference typically takes weeks to respond, they follow up early and persistently. If something in your background might raise questions, they provide context upfront.
When unexpected problems arise, good services work actively to resolve them. They don’t just forward you the payer’s request and wait for you to handle it. They tell you what the payer needs, help you gather the right information, and ensure it gets submitted properly.
Mediocre services are reactive. They only address problems after they cause delays. When payers ask questions, they simply pass the question to you without guidance on how to respond. They don’t anticipate issues or prevent them. This passive approach extends your credentialing timeline significantly.
Technology and Tracking Systems
How a credentialing service tracks applications and manages documentation tells you a lot about their operation. Good services use robust systems that let you see where each application stands in real time. You can log into a portal and check status, see what documentation has been submitted, view any payer requests, and track approval dates.
These systems also help prevent errors. They flag missing information before applications go out. They track expiration dates on licenses and certifications so you know when things need renewal. They maintain a complete file of all your credentialing documents in one place.
Mediocre services might use spreadsheets or basic databases that only they can access. You have to email or call to get status updates. There’s no transparency into what’s happening. Documentation gets scattered across emails and file folders. Things get lost or overlooked because there’s no systematic tracking.
The technology doesn’t have to be fancy, but it does need to be functional and accessible. You should be able to get information about your credentialing status without having to wait for someone to pull up a file and get back to you.
CAQH Management Done Right
 Most commercial payers pull provider information from CAQH ProView, a centralized database where providers enter their information once and payers can access it. Keeping your CAQH profile current and complete is critical for smooth credentialing.
Most commercial payers pull provider information from CAQH ProView, a centralized database where providers enter their information once and payers can access it. Keeping your CAQH profile current and complete is critical for smooth credentialing.
Good credentialing services actively manage your CAQH profile. They make sure it’s complete before starting any credentialing applications. They update it when anything changes. They monitor it to ensure it doesn’t lapse into inactive status. They know which fields payers pay the most attention to and make sure those are thoroughly filled out.
Mediocre services treat CAQH as an afterthought. They might help you set it up initially but don’t maintain it. They don’t catch when information becomes outdated. They don’t notice when your profile goes inactive because you haven’t attested in 120 days. Then credentialing applications stall because payers can’t pull complete information from CAQH.
Some providers try to manage CAQH themselves, which can work if you’re diligent about it. But a good credentialing service takes this off your plate entirely and ensures it’s always current.
Follow-Through on Recredentialing
Initial credentialing is only the beginning. Most payers require recredentialing every two to three years. Medicare requires revalidation every five years. Your medical licenses need renewal. Your board certifications expire. Your malpractice insurance renews annually.
Good credentialing services track all these renewal dates and start the recredentialing process with plenty of lead time. They notify you several months before credentials expire. They submit recredentialing applications early enough that approval comes through before your current credentials lapse.
Mediocre services focus on initial credentialing but drop the ball on maintenance. You get credentialed initially, everything seems fine, then two years later you suddenly can’t bill a payer because your credentials expired and no one started the recredentialing process. Now you’re scrambling to get recredentialed while losing revenue.
Ongoing credential maintenance is actually more important than initial credentialing because you’re already seeing patients and billing insurance. A lapse in credentials means lost revenue and disruption to patient care. Good services prevent this through systematic tracking and timely renewal.
Transparent Pricing
 Credentialing services use different pricing models. Some charge per application. Some charge monthly fees. Some have setup fees plus ongoing maintenance costs. The specific model matters less than whether the pricing is clear and predictable.
Credentialing services use different pricing models. Some charge per application. Some charge monthly fees. Some have setup fees plus ongoing maintenance costs. The specific model matters less than whether the pricing is clear and predictable.
Good services explain exactly what you’ll pay, what’s included, and what costs extra if anything. They’re upfront about fees before you sign a contract. If there are circumstances where additional charges apply, they explain those clearly. You know what your investment will be.
Mediocre services have confusing pricing with hidden fees. The initial quote sounds great, but then you discover extra charges for expedited processing, additional states, CAQH management, or recredentialing. The final cost ends up being much higher than what you expected.
Watch out for services that charge separately for things that should be included in standard credentialing, like following up with payers on application status or responding to requests for additional information. These are core parts of the credentialing process, not add-on services.
Real Expertise and Experience
The credentialing industry has a lot of newcomers and generalists who handle credentialing as a side service along with medical billing or practice management. While some of these are perfectly competent, there’s real value in working with a service where credentialing is a core focus.
Good credentialing services employ people who do this work full-time and have done it for years. They’ve handled thousands of applications. They know the quirks of different payers. They have established contacts at insurance companies who can help move applications along or resolve issues. They stay current on changing requirements and regulations.
You can often tell the level of expertise from initial conversations. When you ask questions, do they give specific, knowledgeable answers or vague generalitie? Do they ask good questions about your situation to make sure they can handle your specific needs? Do they explain things clearly or hide behind jargon?
Mediocre services might have one person who handles credentialing among many other duties. They’re working off checklists and templates without deep knowledge of the process. When unusual situations arise, they don’t know how to handle them.
What Red Flags to Watch For
Certain warning signs suggest you’re dealing with a mediocre credentialing service:
- Promising unrealistically fast credentialing timelines
- Unwilling to provide client references or examples of their work
- Poor communication during the sales process (if they’re unresponsive now, it won’t get better)
- Unclear or constantly changing pricing
- No clear point of contact or account manager assigned to you
- Using outdated technology or no portal access for clients
- Can’t explain their quality control process for applications
- No experience with your specific provider type or specialty
- Focus on how cheap they are rather than the quality of their work
- Push you to sign quickly without giving you time to evaluate
Trust your instincts. If something feels off during the evaluation process, it probably is. Good credentialing services want you to make an informed decision and will take time to answer your questions thoroughly.
Questions to Ask Before Choosing
When evaluating credentialing services, ask specific questions that will reveal the differences between good and mediocre providers:
- What is your average timeline for initial credentialing with major commercial payers? (Look for specific numbers based on actual data)
- How often will I receive status updates, and in what format? (Weekly updates should be standard)
- What is your quality control process before submitting applications? (There should be a clear review process)
- Do you have experience credentialing providers in my specific specialty? (Ask for examples)
- What happens if an application is rejected or delayed? (Good services have clear processes for handling problems)
- How do you handle CAQH profile management? (Should be included and actively maintained)
- What is included in your pricing, and what costs extra? (Everything should be transparent)
- How do you track recredentialing dates and ensure credentials don’t lapse? (Should have systematic tracking)
- Can I speak with current clients as references? (Good services will readily provide references)
- Who will be my main point of contact, and how quickly do you typically respond to questions? (Should be clear ownership and fast response)
The answers to these questions will tell you much more than any marketing materials or sales presentations.
The Long-Term Relationship
Credentialing isn’t a one-time transaction. It’s an ongoing relationship. You need a service that will be there not just for initial credentialing but for years of maintenance, updates, and recredentialing cycles.
Good services view you as a long-term partner. They’re invested in your success because they want to keep working with you. They’re responsive to your needs, they adapt as your practice grows or changes, and they continually look for ways to make the process smoother.
Mediocre services view credentialing as transactional. They get you credentialed initially, collect their fee, and then service quality drops off. When you need help with recredentialing or updates, they’re slow to respond or try to charge additional fees for basic maintenance.
Think about where you want your practice to be in three to five years. Will this credentialing service be able to grow with you? If you add providers, expand to new locations, or start offering new services, can they handle the increased credentialing needs?
Making the Right Choice
 The difference between good and mediocre credentialing services comes down to expertise, systems, communication, and commitment to quality. Good services have deep knowledge of the credentialing process, robust systems for tracking and managing applications, proactive communication that keeps you informed, and quality control processes that prevent errors and delays.
The difference between good and mediocre credentialing services comes down to expertise, systems, communication, and commitment to quality. Good services have deep knowledge of the credentialing process, robust systems for tracking and managing applications, proactive communication that keeps you informed, and quality control processes that prevent errors and delays.
These differences directly affect your practice. Working with a good credentialing service means you get enrolled faster, avoid costly delays from application errors, maintain current credentials without gaps, and spend less time worrying about administrative processes. Working with a mediocre service means frustration, delays, lost revenue, and time wasted fixing problems.
At Medwave, we’ve been providing medical billing, credentialing, and payer contracting services to healthcare providers for years. We’ve seen what works and what doesn’t. Our credentialing team focuses on accuracy, proactive communication, and getting providers enrolled as quickly as possible while avoiding the errors that create delays. We track average timelines, maintain detailed status updates, and handle everything from initial applications through ongoing maintenance and recredentialing.
When you’re evaluating credentialing services, take the time to ask questions, check references, and really examine what you’re getting. The cheapest option often costs you more in the long run through delays and lost revenue. The right credentialing partner should make your life easier, not add to your administrative headaches.

