Payer Contracting Timelines
Average time frames from application to approval:
- Large commercial carriers: 4-6 months
- Regional insurance plans: 3-5 months
- Medicare enrollment: 2-3 months
- Medicaid: 2-6 months (varies by state)
- Managed care plans: 3-4 months
Key factors affecting timeline:
- Application completeness and accuracy
- Network capacity and demand
- Negotiation requirements
- Committee meeting schedules
How to accelerate the process:
- Submit complete applications with all documentation
- Respond to requests within 24-48 hours
- Follow up weekly on application status
- Consider professional credentialing services
Understanding the Contracting Process
 You’ve decided to expand your insurance network or you’re setting up a new practice that needs payer contracts. The next question everyone asks is “how long will this take?” If you’re hoping for a quick answer like “30 days,” prepare to be disappointed. Payer contracting is rarely fast, and the timeline varies dramatically based on multiple factors.
You’ve decided to expand your insurance network or you’re setting up a new practice that needs payer contracts. The next question everyone asks is “how long will this take?” If you’re hoping for a quick answer like “30 days,” prepare to be disappointed. Payer contracting is rarely fast, and the timeline varies dramatically based on multiple factors.
Most healthcare providers seriously underestimate how long it takes to get contracted with insurance companies. This miscalculation creates significant problems. New practices open their doors expecting to bill insurance immediately, only to discover they can’t see most patients for months. Established practices hire new providers who sit idle or see only cash-pay patients while waiting for contracts to process. The revenue impact can be devastating.
What’s Involved in Payer Contracting?
Before we get into specific timelines, let’s clarify what payer contracting actually involves. Many people confuse credentialing with contracting, but they’re related yet distinct processes.
- Credentialing is the verification process where the insurance company confirms you’re qualified to provide healthcare services. They check your medical school credentials, verify your licenses, review your malpractice history, and confirm you meet their network participation standards. This is primarily an administrative verification process.
- Contracting is the business agreement process where you and the payer negotiate and finalize the terms under which you’ll participate in their network. This includes reimbursement rates, contract language, claims submission requirements, and all the other terms that govern your business relationship.
For most commercial insurance plans, these processes happen somewhat simultaneously but aren’t identical. You might complete credentialing but still be negotiating contract terms. Or you might agree to contract terms but still be waiting for credentialing verification to finish.
Medicare works differently because it’s an enrollment process rather than traditional contracting. You enroll through PECOS and accept Medicare’s published fee schedule. There’s no negotiation of rates, so it’s generally faster than commercial payer contracting.
Detailed Timeline Breakdown by Payer Type
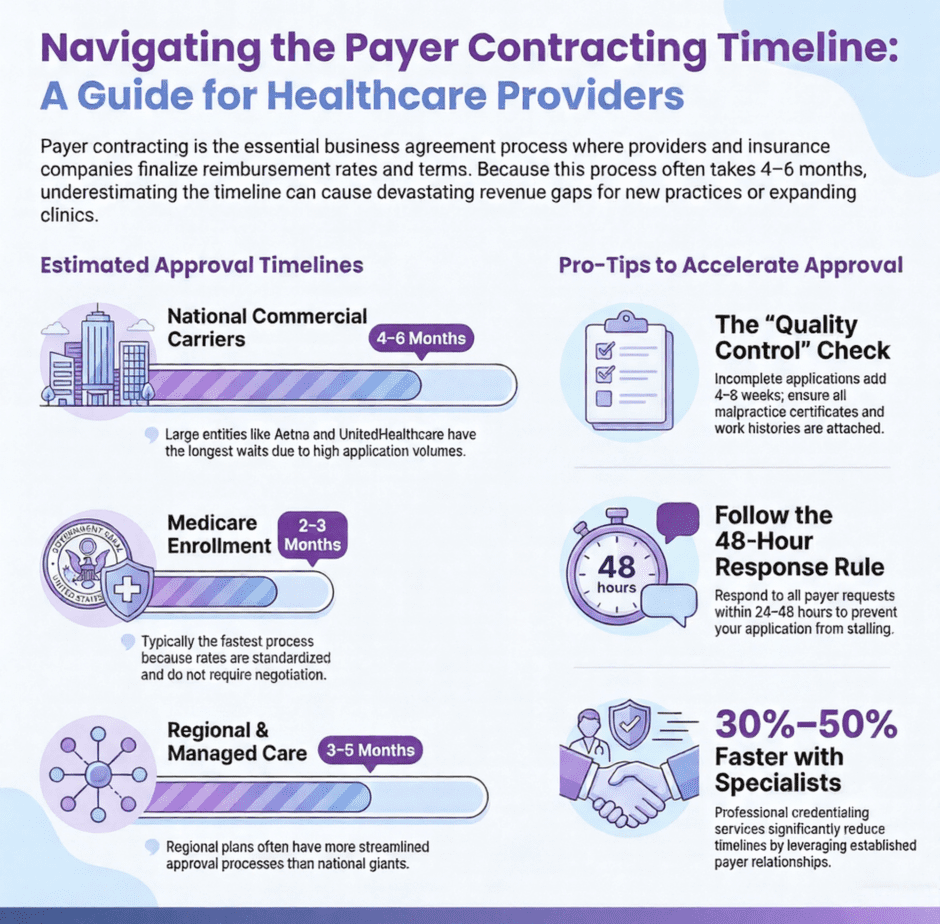
Large National Commercial Carriers: 4-6 Months
Includes: Blue Cross Blue Shield, UnitedHealthcare, Aetna, Cigna
The big national insurance companies have the most patients but often the longest processing times. Their credentialing departments handle thousands of applications, and their approval processes involve multiple committees and review stages. Even with a clean application containing no issues, expect four to six months from submission to final approval.
Some providers report getting approved in three months with these carriers, but that’s the exception rather than the rule. Plan for six months and consider anything faster a pleasant surprise.
Why they take longer:
- High application volume
- Multiple review committees
- Complex organizational structure
- Thorough verification processes
- National network coordination requirements
Regional Commercial Plans: 3-5 Months
Includes: Anthem, Highmark, Health Partners, regional Blues plans
Regional carriers typically process applications somewhat faster than the national giants, but not dramatically so. Three to five months is the standard range. These payers often have smaller networks and may be more motivated to add quality providers, which can occasionally speed things up.
Regional plans generally have more streamlined approval processes because they’re managing smaller geographic areas and fewer providers overall. However, they still conduct thorough verification and committee reviews.
Medicare Enrollment: 2-3 Months
Through PECOS (Provider Enrollment, Chain, and Ownership System)
Medicare enrollment is generally faster than commercial contracting because there’s no negotiation involved. You’re simply enrolling to accept Medicare’s published rates. The process is fairly standardized, and if your application is complete and accurate, two to three months is typical.
The Medicare enrollment process includes:
- PECOS online application submission
- Background verification
- License and credential checks
- Database updates
- Approval and effective date assignment
However, certain situations can extend Medicare enrollment. If you’re revalidating after a period of inactivity, or if there are issues with your background check, the timeline can stretch to four or five months.
Medicaid: 2-6 Months (State Dependent)
Medicaid timelines vary wildly depending on which state you’re in. Some states have streamlined enrollment processes and can get providers enrolled in two to three months. Other states have notoriously slow Medicaid programs where six months or more is common.
- Fastest processing states: Typically 2-3 months
- Average processing states: 3-4 months
- Slowest processing states: 5-6 months or longer
Additionally, many states have moved to Medicaid managed care, where you’re actually contracting with private companies that manage Medicaid benefits. In those cases, you might be dealing with timelines similar to commercial payers.
Managed Care Plans: 3-4 Months
Includes: HMOs, narrow network plans, Medicaid managed care organizations
Managed care organizations often process applications in the three to four month range. Because these plans typically have smaller, more tightly managed networks, they may review applications more carefully, but they also may be more motivated to fill network gaps.
If you’re applying to fill a clear network need (for example, you’re the only pediatric cardiologist within 50 miles), the process may move faster as the plan prioritizes your application.
Common Causes of Delays
1. Incomplete Applications
Impact: Adds 4-8 weeks to timeline
This is the number one cause of delays. Every payer has specific documentation requirements, and missing even one item can stall your application for weeks or months.
Most commonly missing items:
- Current malpractice insurance certificates with adequate coverage levels
- Verification of all hospital affiliations
- Professional references with complete contact information
- Documentation of board certifications
- Work history explanations for any gaps in employment
How delays compound: Payers typically won’t process incomplete applications. They’ll send a request for additional information, which might take two weeks to reach you. You provide the missing items, which takes another week or two. Then your application goes back into the queue behind all the complete applications that came in after yours. One missing document can easily add four to eight weeks to your timeline.
2. Network Capacity Limits
Impact: Can add months or result in denial
Insurance companies manage their networks strategically. They want enough providers to meet member needs without having so many providers that utilization becomes too high. If a payer determines they have adequate network coverage in your specialty and geographic area, they may not be actively accepting new providers.
When networks are closed or nearly full, applications take longer as the payer evaluates whether they really need to add you. They might tell you they’re not accepting applications. Or your application might sit in pending status for months while they decide. Some payers maintain waiting lists for certain specialties in certain areas.
This is particularly common in markets with high provider density and for primary care positions where payers typically have many options.
3. Background Check Delays
Impact: Adds 2-6 weeks on average
Every payer conducts background verification, including checking the National Practitioner Data Bank, verifying licenses with state medical boards, confirming board certifications, and reviewing your professional history. Most of this happens fairly quickly, but sometimes there are delays.
What triggers longer background reviews:
- Malpractice claims requiring explanation
- License discipline (even if resolved)
- Gaps in work history
- Multiple state licenses to verify
- Recent changes in employment
Even clean backgrounds can experience delays if the verification services are backed up or if state medical boards are slow to respond to verification requests.
4. Contract Negotiation
Impact: Adds 1-3 months
If you’re negotiating contract terms rather than simply accepting a standard agreement, expect the timeline to extend. Each round of proposal and counter-proposal adds time. The payer might take two weeks to respond to your requested changes. You take a week to review their response. This cycle can repeat several times.
Negotiation is more common when you have leverage, like being a needed specialty or having strong patient volume. Smaller or newer practices often don’t have much negotiating power and simply accept standard contracts, which processes faster.
5. Internal Approval Processes
Impact: Adds 2-8 weeks
Most insurance companies have credentialing committees that meet periodically to review and approve applications. These committees might meet monthly, meaning your completed application could wait up to a month just for the next committee meeting.
After committee approval, additional steps include:
- Final contract execution
- Provider directory updates
- Claims system setup
- Provider ID assignment
- Network file updates
Each step adds time to the overall process.
6. Committee Meeting Schedules
Impact: Can add 1-3 months
As mentioned, most payers use committees rather than individual reviewers to make credentialing decisions. If your application is completed just after a committee meeting, you’ll wait until the next one.
Committee meeting frequency varies:
- Large national payers: Usually monthly
- Regional payers: Monthly or bi-monthly
- Smaller plans: Quarterly
- Specialty networks: Quarterly or as-needed
Missing a committee meeting by a few days can add a full month or quarter to your wait.
How to Speed Up Your Contracting Timeline
1. Submit Complete, Accurate Applications
Potential time saved: 4-8 weeks
This cannot be emphasized enough. Review the payer’s requirements carefully before submitting anything. Create a checklist of every required document and piece of information.
Quality control checklist:
- Dates match across all documents
- Names are spelled consistently
- License numbers are accurate
- All signatures are present
- All required attachments included
- Forms filled out completely (no blank fields)
Have someone else review your application before submission. A second set of eyes catches errors you might miss. The few hours invested in careful review can save months of delays.
2. Respond Immediately to Payer Requests
Potential time saved: 2-4 weeks
When a payer contacts you for additional information, treat it as urgent. Respond within 24 hours if possible, and no more than 48 hours. The faster you provide what they need, the faster your application moves forward.
Set up systems to catch requests:
- Email alerts for messages from payer domains
- Daily fax checks (many payers still use fax)
- Staff training to flag insurance communications
- Dedicated email folder for credentialing correspondence
Make sure your office staff knows to flag any communication from insurance companies as high priority.
3. Maintain Complete Documentation Files
Potential time saved: 1-2 weeks per request
Don’t wait for payers to request documents. Provide everything they might need with your initial application.
Essential documents to have ready:
- Current malpractice insurance certificates (with declarations page)
- All state licenses (current and in good standing)
- Board certifications (current copies)
- DEA certificate (if applicable)
- CV formatted to payer specifications
- Professional references with complete contact information
- Work history documentation explaining any gaps
- Hospital privilege letters (if you have affiliations)
- Collaboration agreements (for APRNs, PAs)
- Immunization records (some payers require)
Having these documents organized and ready also makes it easy to respond quickly if a payer does request something additional.
4. Follow Up Weekly on Status
Impact: Prevents applications from stalling
Be proactive about checking on your application status. Call or email the payer’s provider services department weekly to ask where your application stands.
This serves two purposes:
- You’ll know immediately if there’s a problem or missing information
- Regular contact keeps your application top of mind and reduces the chance it gets overlooked
Follow-up best practices:
- Keep a log of all communications (date, person spoken to, information provided)
- Be professional and courteous
- Ask specific questions: “What stage is my application in?” “Is any additional information needed?” “When is the next committee meeting?”
- Request timeline estimates
The people processing your application are typically overwhelmed with work. Friendly persistence works better than aggressive demands.
5. Work with Credentialing Specialists
Potential time saved: 30-50% reduction in overall timeline
Professional credentialing services handle payer contracting all day, every day. They know exactly what each payer requires, have relationships with payer credentialing departments, and follow proven processes that avoid common delays.
Advantages of professional services:
- Applications submitted correctly the first time
- Established payer relationships for faster follow-up
- Systematic tracking prevents missed deadlines
- Experience troubleshooting unusual situations
- Can manage multiple applications simultaneously
In many cases, credentialing specialists can get providers contracted 30% to 50% faster than providers manage on their own. The cost of credentialing services is typically far less than the revenue lost to extended contracting delays.
6. Apply to Multiple Payers Simultaneously
Total timeline reduction: 3-5 months
Don’t contract with payers one at a time. Submit applications to all your target payers at once. This parallel processing means you’ll have multiple approvals coming through over a period of months rather than waiting for each one sequentially.
Example comparison:
- Sequential approach: 6 payers × 4 months each = 24 months total
- Parallel approach: 6 payers applied simultaneously = 4-6 months total
The paperwork burden is heavier upfront, but the overall timeline to get a full insurance panel is much shorter.
Managing Revenue During Contracting Delays
Plan Your Finances Realistically
For new practices: Budget for at least six months of operating expenses without insurance revenue. This means adequate capital reserves or credit lines to cover rent, staff salaries, supplies, and other overhead while contracts process.
For practices adding providers: Factor in that new providers will generate limited revenue for several months. Don’t hire based on the assumption of immediate full productivity.
Financial planning checklist:
- Calculate monthly operating expenses
- Multiply by 6 months for adequate runway
- Add buffer for unexpected delays (2-3 additional months)
- Identify funding sources (savings, loans, investors)
- Plan for staged hiring if capital is limited
Communicate Transparently with Patients
Be honest with patients about your insurance status. When patients call to schedule, let them know which insurance plans you’re currently contracted with and which are pending.
Sample script: “We’re currently in-network with [list plans]. We’ve applied to be in-network with [other plans] and expect approval within the next few months. I’m happy to schedule you now if you’d like to wait, or we can discuss self-pay options if you’d prefer to be seen sooner.”
Patients appreciate honesty and may be willing to wait a few weeks if they know you’re working on their insurance plan.
For established patients who want to continue seeing you but your contract with their plan hasn’t processed yet, explain the situation and work out interim arrangements.
Alternative Payment Options
Consider these approaches for seeing patients before contracts finalize:
- Self-pay pricing: Offer discounted rates for patients paying directly, often 30-40% below your planned insurance rates. This covers your costs and provides some revenue while remaining affordable for patients.
- Payment plans: Accept credit cards and offer installment payment options for higher-cost services. This removes the barrier of upfront payment for patients.
- Hold and refile: For established patient relationships and pending contracts, consider seeing patients and holding claims until contracts process. Document this agreement in writing with patients.
- Out-of-network billing: Bill patients directly with clear explanation that they can submit for out-of-network benefits from their insurance. Provide a superbill with all necessary information.
These aren’t ideal solutions, but they’re better than having new providers sitting idle or turning away patients entirely.
Start Early
Timeline recommendations:
- Opening a new practice: Start contracting process 6-9 months before your planned opening date. This gives you buffer time for delays while ensuring at least some contracts are active when you open.
- Hiring new providers: Begin credentialing the moment they accept your job offer, even if their start date is months away. Track “time-to-productivity” as a key metric for your hiring process.
- Expanding to new locations: Start location-specific credentialing applications 6 months before the new office opens. Some payers require separate credentialing for each service location.
- Adding new service lines: Apply for new procedure codes or specialty designations 3-4 months before you plan to begin offering services.
When Contracting Takes Too Long
Internal Escalation at the Payer
Most payers have escalation paths for application delays. Start with your regular contact in provider services. If they can’t resolve the issue, ask to speak with a supervisor or manager.
Escalation steps:
- Contact assigned credentialing representative (if you have one)
- Request supervisor review after 2 weeks without resolution
- Ask for manager involvement after 4 weeks
- Request executive review for applications exceeding stated timelines by 30+ days
Document all your communications, including dates, names, and what you were told. This documentation becomes important if you need to escalate further.
Be professional but firm about the need for resolution. Explain the business impact of the delay on your practice and your patients.
State Insurance Department Complaints
If escalation within the payer doesn’t work, you can file a complaint with your state’s insurance commissioner or department of insurance.
When to file a complaint:
- Application has exceeded payer’s stated timeline by 60+ days
- Payer is non-responsive to escalation attempts
- You suspect discriminatory practices
- Payer is violating state regulations
Many states have regulations about timely processing of provider applications. Filing a complaint often gets attention from payer leadership and can break logjams.
How to file:
- Visit your state insurance department website
- Complete provider complaint form
- Attach documentation of your application and follow-up attempts
- Include timeline of communications
- Specify relief requested (expedited processing)
However, use this as a last resort after exhausting other options, as you want to maintain a good working relationship with payers when possible.
Know Your State’s Laws
Some states have laws requiring payers to process credentialing applications within specific timeframes, often 60 to 90 days.
States with prompt credentialing laws include:
- California: 90 days
- Texas: 180 days
- Illinois: 90 days
- New York: 90 days
- Others vary
Check your state’s regulations. If a payer is violating statutory requirements, pointing this out in your communications can motivate faster action. Include specific statute citations in your correspondence.
Interim Billing Arrangements
In some cases, you can negotiate interim arrangements while contracting finalizes.
Possible interim solutions:
- Single case agreements: The payer agrees to cover specific patients at negotiated rates until your contract processes. You submit these on a case-by-case basis.
- Provisional status: Some payers offer provisional participation letters stating your application is approved pending final contract execution. This allows you to begin seeing patients and submitting claims.
- Retrospective credentialing: Once your contract is finalized, some payers will retroactively process claims from a certain period before your effective date (usually 30-90 days).
These arrangements aren’t always possible, but they’re worth requesting if contracting delays are significantly impacting your practice.
Planning for Long-Term Success
Build Contracting Into Practice Workflows
Create standard operating procedures for:
- New provider onboarding (including credentialing timeline)
- Contract renewal tracking (most contracts require recredentialing every 2-3 years)
- New location credentialing (when expanding)
- Provider departure notifications to payers
Assign specific staff responsibility for managing these processes, or partner with credentialing services to handle them systematically.
Track Your Metrics
Monitor these key performance indicators:
- Average time from application to approval by payer
- Percentage of applications requiring additional information
- Number of applications currently pending
- Time-to-first-billing for new providers
- Revenue impact of credentialing delays
Use this data to identify problems and improve your processes over time. If certain payers consistently take longer or request more information, adjust your approach for those payers.
Maintain Good Payer Relationships
Your credentialing experience sets the tone for your ongoing relationship with payers. Providers who are organized, responsive, and professional during credentialing often receive better service throughout the contract relationship.
Relationship-building practices:
- Keep accurate records of all payer contacts
- Maintain professional communication
- Meet all payer requirements promptly
- Notify payers of practice changes quickly
- Attend payer provider meetings when invited
These relationships can help when you need assistance with claims issues, contract questions, or future credentialing needs.
Getting Professional Help
When to Consider Credentialing Services
You should consider professional credentialing support if:
- You’re opening a new practice and need multiple contracts quickly
- You’re expanding to multiple locations
- You’re hiring multiple providers simultaneously
- Your staff is overwhelmed with credentialing work
- Your contracting timelines consistently exceed norms
- You’re experiencing frequent application rejections or delays
- You lack expertise in payer-specific requirements
What Credentialing Services Provide
Core services include:
- Complete application preparation and submission
- Documentation organization and verification
- Weekly follow-up with payers on application status
- Problem resolution and escalation when needed
- Recredentialing timeline tracking and management
- Provider communication and status updates
Additional services may include:
- Payer contract negotiation support
- Rate benchmarking and analysis
- Contract language review
- Multi-state credentialing coordination
- Telehealth credentialing across state lines
Return on Investment
The cost of credentialing services is typically far less than the revenue lost to extended contracting delays.
Example calculation:
- Provider generates $40,000 monthly in insurance collections
- Professional credentialing reduces timeline from 6 months to 4 months
- Revenue gained from 2-month acceleration: $80,000
- Credentialing service cost: $3,000-5,000
- Net benefit: $75,000-77,000
Even without acceleration, credentialing services free your staff time for higher-value activities and reduce the stress and errors associated with managing the process internally.
Summary: The Wait for Payer Contracting
Payer contracting is a necessary but time-consuming part of running a healthcare practice. The key is to plan for realistic timelines rather than hoping for best-case scenarios.
Remember these key points:
- Commercial payer contracting takes 4-6 months on average
- Medicare enrollment typically takes 2-3 months
- Medicaid varies by state but plan for 3-6 months
- Incomplete applications are the main cause of delays
- Starting early prevents revenue gaps
- Professional credentialing services can reduce timelines by 30-50%
Start the process as early as possible. Submit complete, accurate applications. Respond immediately to requests for additional information. Follow up regularly on application status.
Most importantly, plan your practice finances around realistic contracting timelines. Don’t open a new practice, hire new providers, or expand to new locations based on the assumption that insurance contracts will process quickly. Build in adequate financial runway to sustain operations during the contracting period.
 At Medwave, we specialize in medical billing, credentialing, and payer contracting for healthcare practices. Our team manages the entire contracting process, from initial applications through final approval, using proven systems that minimize delays and maximize efficiency. We track applications systematically, maintain relationships with payer credentialing departments, and follow up persistently to keep your applications moving forward.
At Medwave, we specialize in medical billing, credentialing, and payer contracting for healthcare practices. Our team manages the entire contracting process, from initial applications through final approval, using proven systems that minimize delays and maximize efficiency. We track applications systematically, maintain relationships with payer credentialing departments, and follow up persistently to keep your applications moving forward.
Our clients typically see 30% to 50% faster contracting times compared to handling the process internally. We handle the administrative burden so you can focus on patient care while we ensure your insurance relationships are in place when you need them.
If your practice is facing contracting delays or you’re planning expansion that requires new payer relationships, contact us to discuss how we can help accelerate your timeline and get you billing insurance sooner.

