Effective billing practices are crucial for healthcare providers, medical offices, and businesses across various industries to maintain financial stability and ensure proper compensation for services rendered. Optimizing reimbursement in billing involves implementing strategic processes, leveraging technology, and staying compliant with industry regulations.
We discuss key strategies and best practices to maximize reimbursement rates and streamline billing operations.
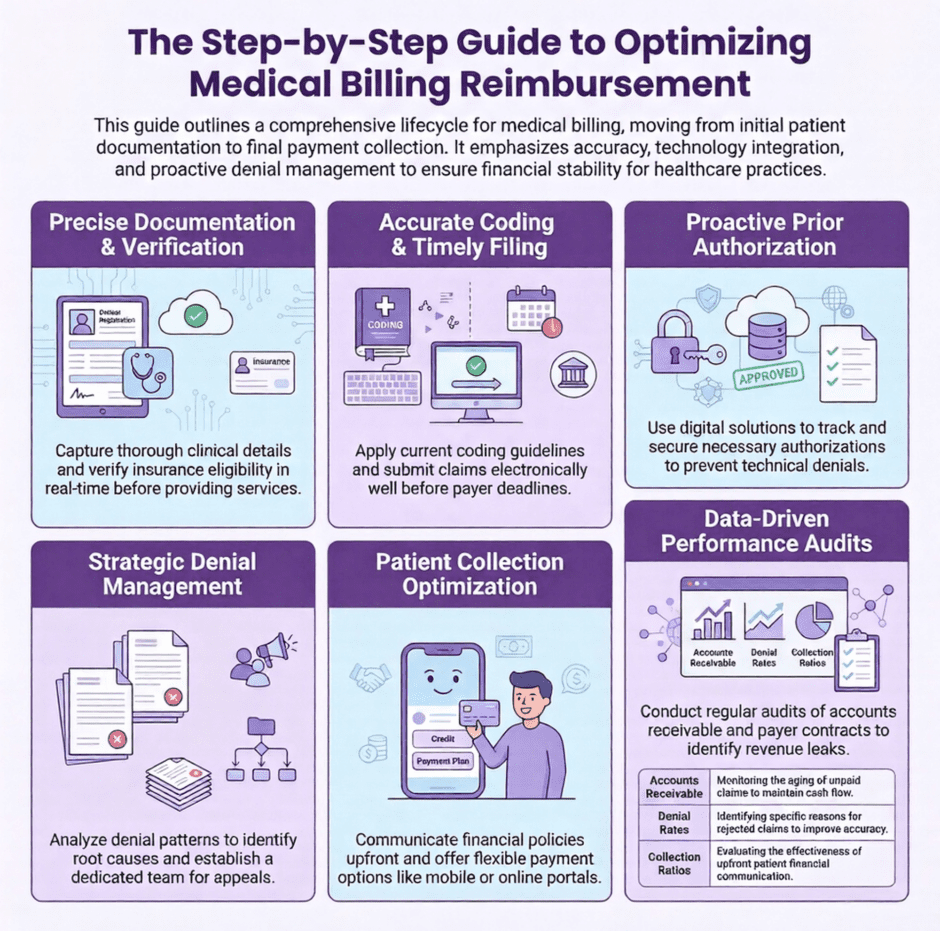
See the Following to Optimize Your Billing Reimbursement
Getting paid accurately and on time does not happen by accident. From clean documentation and proper coding to denial management and payer contract negotiation, optimizing billing reimbursement requires a deliberate, multi-layered approach. Whether you are tightening up your charge capture process or investing in better technology, the practices outlined here give healthcare providers and billing teams a practical roadmap for improving cash flow and reducing revenue loss across the board.
Accurate and Complete Documentation

The foundation of optimal reimbursement lies in thorough and precise documentation. Proper documentation not only supports the services provided but also justifies the billed amounts to payers. To improve documentation, train staff on proper techniques specific to your industry and implement standardized templates. Regularly audit documentation for completeness and accuracy, and utilize electronic health records (EHR) or digital documentation systems to ensure all relevant details are captured, including dates, times, and specific services provided.
Verify Insurance Coverage and Eligibility
One of the most common reasons for claim denials is insurance ineligibility. To mitigate this issue, implement a robust verification process for all patients or clients. Utilize real-time eligibility verification tools to confirm coverage details, including copayments, deductibles, and any pre-authorization requirements. Educate patients or clients about their insurance benefits and potential out-of-pocket expenses to avoid surprises and improve collection rates.
Proper Coding Practices
Accurate coding is essential for correct reimbursement. Improper coding can lead to claim denials, delayed payments, or even accusations of fraud. To optimize coding, stay updated on current guidelines and regulations, and provide ongoing training for coding staff. Consider implementing computer-assisted coding (CAC) tools and conducting regular internal audits of coding practices. For complex cases or specialized fields, consider hiring certified coders or outsourcing to coding specialists.
Timely Filing of Claims
Submitting claims promptly is crucial for maintaining a healthy cash flow and avoiding missed deadlines. Establish clear workflows for claim submission and set internal deadlines that are earlier than payer deadlines. Use electronic claim submission whenever possible to speed up the process. Implement automated reminders for approaching deadlines and monitor claim status regularly to identify and address any issues quickly.
Implement a Strong Denial Management Process
Despite best efforts, claim denials can still occur. A robust denial management process can help recover lost revenue and prevent future denials. Analyze denial patterns to identify common issues and address root causes through process improvements. Develop a dedicated team for handling denials and establish clear timelines and procedures for appealing denials. Utilizing denial management software can streamline the process and improve efficiency.
Utilize Technology and Automation
Leveraging technology can significantly improve billing efficiency and accuracy. Consider implementing practice management software, automated claim scrubbing tools, and electronic remittance advice (ERA) processing. Patient portals for online bill pay and communication can improve patient engagement and collections. Business intelligence tools for financial reporting and analysis can provide valuable insights into your billing performance.
Stay Updated on Payer Policies and Industry Changes
Reimbursement policies and regulations are constantly evolving. To stay ahead, regularly review payer bulletins and updates, and attend industry conferences and workshops. Subscribe to relevant publications and newsletters, and join professional associations in your field. Establishing relationships with payer representatives for direct communication can also be beneficial in navigating policy changes.
Optimize Prior Authorization Processes
Prior authorizations can be a significant barrier to timely reimbursement. To streamline this process, implement electronic prior authorization (ePA) solutions and maintain a database of payer-specific prior authorization requirements. Train staff on proper documentation for authorization requests and follow up proactively on pending authorizations. When appropriate, appeal denied authorizations to maximize reimbursement opportunities.
Improve Patient Collections
With the rise of high-deductible health plans, patient responsibility for medical bills has increased. To optimize patient collections, clearly communicate financial policies and expectations upfront. Offer multiple payment options, including online and mobile payments, and consider implementing payment plans for large balances. Early-pay discounts or prompt-pay incentives can encourage timely payments. Utilize automated payment reminders and statements to improve collection rates.
Conduct Regular Financial Audits
Periodic audits can help identify areas for improvement in your billing processes. Key areas to review include accounts receivable aging, denial rates and reasons, collection ratios, charge capture accuracy, and payer contract performance. These audits can provide valuable insights into the effectiveness of your billing strategies and highlight areas needing improvement.
Negotiate Favorable Payer Contracts
Effective contract negotiation can lead to better reimbursement rates. Analyze your costs and desired profit margins, and benchmark your rates against industry standards. Highlight your unique value propositions or specialties when negotiating with payers. Consider value-based care models where appropriate, and negotiate for simplified administrative processes, such as reduced prior authorization requirements.
Implement a Robust Compliance Program
Ensuring compliance with healthcare regulations is crucial for avoiding penalties and maintaining proper reimbursement. Develop written policies and procedures, designate a compliance officer or committee, and provide effective training and education for staff. Implement internal monitoring and auditing processes, and establish protocols for prompt response to detected offenses and enforcement of disciplinary standards.
Optimize Revenue Cycle Management
A well-managed revenue cycle can significantly improve reimbursement rates. Focus on streamlining workflows from patient registration to payment posting. Implement key performance indicators (KPIs) to monitor revenue cycle performance and regularly analyze and optimize each stage of the revenue cycle. For some organizations, outsourcing certain revenue cycle functions may be more efficient than in-house management.
Leverage Data Analytics
Using data analytics can provide valuable insights for improving reimbursement. Implement business intelligence tools for financial reporting and analyze claim data to identify trends and opportunities for improvement. Use predictive analytics to forecast reimbursement rates and cash flow, and benchmark your performance against industry standards to identify areas for improvement.
Invest in Staff Training and Development
Well-trained staff are essential for optimizing reimbursement. Provide ongoing education on billing best practices and cross-train staff to improve efficiency and coverage. Offer certifications and professional development opportunities to keep skills current. Cultivate a culture of continuous improvement and learning to ensure your team stays at the forefront of industry best practices.
Implement Charge Capture Best Practices
Ensuring all billable services are accurately captured is crucial for maximizing reimbursement. Implement electronic charge capture systems and conduct regular audits to identify any missed charges. Train clinical staff on the importance of accurate charge documentation and establish clear workflows for communicating billable services between clinical and billing staff.
Frequently Asked Questions on Billing Reimbursement Optimization
- What is the most common reason medical claims get denied?
Insurance ineligibility tops the list. When a patient’s coverage is not verified before a claim is submitted, payers have an easy reason to reject it. Running real-time eligibility checks before every visit, including confirming copayments, deductibles, and prior authorization requirements, eliminates a large share of preventable denials before they ever happen. - How does documentation affect reimbursement rates?
Documentation is essentially your evidence. If a service is not properly documented, payers have no reason to pay for it. Thorough, accurate documentation justifies the billed amounts, supports the codes used, and protects the practice in the event of an audit. Standardized templates and regular documentation audits go a long way toward keeping reimbursement rates where they should be. - What is the difference between a claim denial and a claim rejection?
A rejection means the claim never made it into the payer’s system, usually due to a formatting or data error. A denial means the claim was received and processed, but payment was refused for a specific reason. Both require action, but they go through different resolution paths. Rejections need to be corrected and resubmitted quickly. Denials typically require a formal appeal with supporting documentation. - How often should a practice audit its coding practices?
At a minimum, quarterly. Regular internal coding audits catch patterns of undercoding, overcoding, or mismatched diagnosis and procedure codes before they turn into larger compliance or revenue problems. For high-volume practices or those in specialties with frequent guideline updates, more frequent reviews are worth the investment. - Does submitting claims electronically really make a difference?
It does. Electronic claim submission is faster, reduces manual entry errors, and gives you immediate confirmation that the claim was received. Most payers also process electronic claims significantly faster than paper ones, which improves cash flow. If a practice is still submitting paper claims for any portion of its billing, switching to electronic is one of the quickest wins available. - What should a practice do when a payer repeatedly denies the same type of claim?
That is a pattern worth investigating, not just appealing claim by claim. Look at the denial reason codes across those claims. Is it a coding issue? A documentation gap? A payer policy change that was not communicated clearly? Identifying the root cause and fixing it upstream saves far more time than fighting individual denials after the fact. - How can technology help improve billing reimbursement?
Practice management software, automated claim scrubbing, electronic remittance advice processing, and denial management tools all reduce the manual workload and catch errors before claims go out the door. Patient portals that allow online bill pay also improve collection rates by making it easier for patients to pay quickly. The technology does not replace good billing practices, but it makes executing them much more efficient. - Is it worth outsourcing medical billing to improve reimbursement?
For many practices, yes. Outsourcing to an experienced billing company means having a dedicated team focused entirely on claims accuracy, denial follow-up, and reimbursement optimization. It also removes the burden of keeping up with constantly changing payer policies and coding guidelines in-house. The key is finding a billing partner with a track record in your specialty.
Summary: Optimizing Reimbursement
 Optimizing reimbursement in billing requires a multifaceted approach that combines technology, process improvement, staff training, and a commitment to compliance and accuracy. By implementing these strategies, healthcare providers and businesses can improve their financial performance, reduce denied claims, and ensure they are properly compensated for the services they provide.
Optimizing reimbursement in billing requires a multifaceted approach that combines technology, process improvement, staff training, and a commitment to compliance and accuracy. By implementing these strategies, healthcare providers and businesses can improve their financial performance, reduce denied claims, and ensure they are properly compensated for the services they provide.
Remember that optimization is an ongoing process. Regularly review and refine your billing practices, stay informed about industry changes, and be willing to adapt to new technologies and methodologies. With a dedicated approach to reimbursement optimization, you can achieve greater financial stability and focus more resources on providing quality services to your patients or clients.

