At present, medical credentialing is one of the most critical components of healthcare administration. However, it is an endeavor that comes with its own set of challenges.
From streamlining the entire process to ensure credentialing committees have adequate resources, there are a lot of challenges that need to be addressed to ensure that things run smoothly.
We’ll take a look at the 10 significant challenges in the healthcare credentialing system and what can be done to mitigate them.
The 10 Challenges in Medical Credentialing
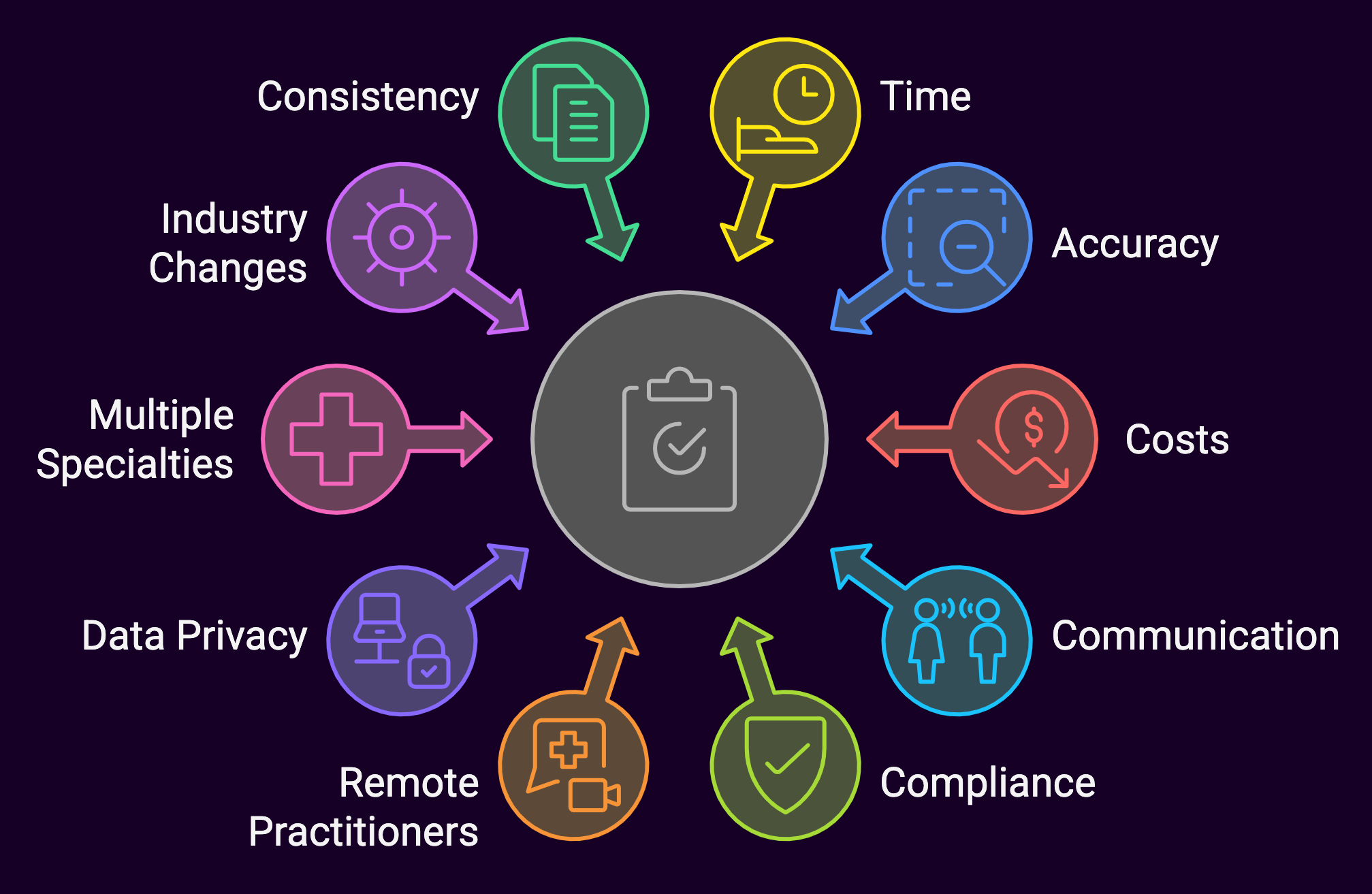
-
Time
Credentialing is a time-consuming one. It is critical to ensure that every practitioner’s credentials are verified before granting them the privilege of treating patients. This involves contacting multiple agencies and verifying multiple credentials. To make this faster, healthcare organizations need to adopt digital solutions. Automated software can streamline the process and ensure that every credential is verified before the practitioner starts treating patients.
-
Accuracy
The accuracy of the data in the credentialing effort is crucial. Every credential needs to be verified, and any discrepancy can cause issues. To mitigate this challenge, healthcare organizations can implement real-time monitoring solutions that can track any changes to the practitioner’s credentials. This will ensure that any changes are immediately flagged, and the credentialing committee can take the necessary action.
-
Costs
Credentialing can be an expensive effort. Healthcare organizations need to ensure that they have adequate resources to streamline the entire operation. One way to do this is to outsource credentialing to a third-party vendor. This can significantly reduce the costs associated with credentialing and ensure things are being completed accurately and efficiently.
-
Communication
This involves multiple parties, including the practitioner, the healthcare organization, and the credentialing committee. Communication can be a challenge, and any delay in communication can cause a delay in positive outcomes. One way to mitigate this challenge is to implement a communication system that allows all parties to communicate in real-time. This will ensure that any issues or changes are communicated quickly and efficiently.
-
Compliance
The healthcare industry is heavily regulated, and compliance is critical. Healthcare organizations need to ensure that their credentialing exercise is compliant with all state and federal regulations. This can be a challenge, but by implementing a compliance management system, healthcare organizations can ensure that their processes (including credentialing) is compliant with all regulations.
-
Credentialing Remote Practitioners
With the rise of telemedicine, healthcare organizations need to ensure that they can credential remote practitioners. Credentialing a remote practitioner can be challenging, as the healthcare organization needs to verify credentials from multiple states. To mitigate this challenge, healthcare organizations need to adopt a remote credentialing operation that can streamline the protocol and ensure that every credential is verified before the practitioner starts treating patients.
-
Data Privacy
The healthcare industry is highly regulated, and patient data privacy is critical. Credentialing involves accessing sensitive patient data, and healthcare organizations need to ensure that the data is kept confidential. To mitigate this challenge, healthcare organizations need to implement data security measures such as encryption and access control.
-
Credentialing Across Multiple Specialties
Credentialing involves verifying multiple credentials across multiple specialties. This can be a time-consuming and challenging venture. To mitigate this challenge, healthcare organizations need to implement a comprehensive credentialing undertaking that can verify credentials across multiple specialties.
-
Keeping Up with Industry Changes
The healthcare industry is constantly evolving, and healthcare organizations need to ensure that their credentialing effort keeps up with industry changes. To mitigate this challenge, healthcare organizations need to implement a continuous improvement process that can adapt to changes in the industry and ensure that everything is up to date.
-
Ensuring Consistency
Credentialing involves multiple parties, and ensuring consistency can be challenging. Healthcare organizations need to ensure that the credentialing is consistent across all practitioners and specialties. To mitigate this challenge, healthcare organizations need to implement a standardized credentialing that can ensure consistency across all practitioners and specialties.
Summary
There are multiple credentialing challenges that need to be addressed to ensure that the credentialing runs smoothly. By adopting digital solutions, outsourcing the credentialing process, implementing real-time monitoring solutions, and communication systems, and ensuring compliance with all regulations, healthcare organizations can mitigate these challenges and ensure that their credentialing is accurate, efficient, and cost-effective. With a streamlined and efficient credentialing procedure in place, healthcare organizations can provide patients with the best possible care while maintaining the integrity of the credentialing.
Contact Medwave for assistance with medical credentialing. We have decades of experience navigating the credentialing waters with both private and public networks.

