At Medwave, we’ve helped dozens of healthcare organizations negotiate better payer contracts and secure fair reimbursement rates. The following use cases show how different types of practices tackled their contract challenges and what actually worked when sitting across the table from insurance companies.
These stories highlight how proper payer contracting helps healthcare organizations improve their financial stability while continuing to deliver quality patient care. Here are some of our most impactful payer contracting use cases, which demonstrate the real difference strategic negotiation makes for healthcare providers.
1. Multi-Specialty Group Practice
A 45-provider group practice in the Southeast was operating on contracts that hadn’t been renegotiated in over six years. Their reimbursement rates were stuck while operating costs had climbed steadily. The practice’s CFO estimated they were leaving approximately $750,000 on the table annually.
After working with Medwave’s contracting team, they achieved:
- 18% average rate increase across major payers
- Improved contract language on claims processing timelines
- Elimination of three problematic prior authorization requirements
- $820,000 in additional annual revenue
“We had tried negotiating on our own multiple times and gotten nowhere,” says their Operations Director. “Having experts who knew what rates were actually achievable made all the difference.”
2. Rural Primary Care Network
A network of seven primary care practices serving rural communities faced contract challenges . Their largest payer contracts included rates that barely covered costs, but the payer knew patients in their service area had limited alternatives. The network felt stuck between accepting unfair rates or potentially leaving patients without in-network options.
Medwave’s strategic approach delivered:
- 22% rate increase on primary payer contract
- New care coordination payments for chronic disease management
- Quarterly performance bonuses tied to quality metrics
- Contract language protecting against unilateral rate reductions
“The negotiation team showed us we had more leverage than we thought,” notes their Medical Director. “They documented our value to the payer’s network and made the business case for fair reimbursement.”
3. Behavioral Health Practice Group
A growing behavioral health group with 15 therapists and 3 psychiatrists discovered their reimbursement rates varied wildly between similar insurance plans. Some paid reasonably well. Others paid rates that hadn’t changed since 2019. The practice wanted to standardize their contracts and bring the low-paying ones up to acceptable levels.
With Medwave’s help, they achieved:
- 27% increase on three underperforming contracts
- Standardized session rates across similar plan types
- Removal of restrictive session limits for established patients
- New reimbursement codes for telehealth services
“We were constantly frustrated by inconsistent rates,” says the practice owner. “Now we have a much more predictable revenue model, and our providers aren’t penalized for seeing patients with certain insurance plans.”
4. Specialty Surgical Center
An orthopedic surgery center had contracts with acceptable facility fees but terrible physician reimbursement rates. The surgeons were performing the same procedures they did at nearby hospitals but getting paid 35% less through the surgery center’s contracts. This created a financial disincentive to use their own facility.
Medwave’s contracting team helped them:
- Increase physician reimbursement rates by 31% on average
- Negotiate better bundled payment structures
- Establish clear policies on out-of-network emergency cases
- Add annual rate adjustment clauses tied to Medicare fee schedule changes
“The contracts were structured in ways that made our surgery center less profitable than hospital-based procedures,” explains their Administrator. “We needed someone who could articulate why that didn’t make sense and negotiate better terms.”
5. Urgent Care Chain
A regional urgent care chain with 12 locations faced a common problem. Their contracts were negotiated location by location over several years, resulting in different rates at different clinics for identical services. This created internal accounting headaches and left money on the table at several locations.
After implementing Medwave’s strategy, they achieved:
- Consolidated contracts across all locations
- 15% average rate increase system-wide
- Uniform rates regardless of location
- Streamlined credentialing for new locations
“Having different rates at different locations was a nightmare to manage,” states their CFO. “Standardizing contracts and improving rates simultaneously was a huge operational and financial win.”
6. Physical Therapy Practice
A physical therapy practice with four locations had solid patient volume and excellent outcomes data, but their largest payer contract hadn’t been updated in eight years. When they requested rate increases on their own, the payer responded with form letters about “current market conditions” and denied the requests.
Medwave’s data-driven approach delivered:
- 24% rate increase on primary payer contract
- New reimbursement for specialized therapy modalities
- Extended authorization periods for chronic condition patients
- Reduced administrative burden on documentation requirements
“We had the data showing our outcomes were better than average, but we didn’t know how to use that in negotiations,” says the practice owner. “The contracting team turned our quality metrics into negotiating power.”
7. Cardiology Group
A seven-physician cardiology group discovered that two of their major payer contracts included reimbursement rates below Medicare levels for certain procedures. This made no sense economically, but when they questioned it, the payers insisted the rates were standard.
With Medwave’s assistance, they achieved:
- Rates brought above Medicare levels across all procedures
- Improved reimbursement for advanced imaging services
- Better payment terms for implantable device procedures
- 19% increase in revenue from the two renegotiated contracts
“We knew something was wrong when we were getting paid less by commercial insurance than by Medicare,” notes their Practice Administrator. “But we needed expertise to prove it and negotiate changes.”
8. Home Health Agency
A home health agency serving a three-county area had contracts that paid per-visit rates significantly lower than regional benchmarks. Their operating costs per visit were well-documented, but payers seemed uninterested in their cost analysis. Revenue wasn’t keeping pace with expenses, and the agency faced tough decisions about service areas.
Medwave helped them achieve:
- 29% average rate increase across major contracts
- New reimbursement for care coordination activities
- Better rates for high-acuity patient visits
- Geographic rate adjustments reflecting travel costs in rural areas
“We were seriously considering cutting service to our most rural communities because we were losing money on every visit,” says their Director. “The new contract rates made those services financially viable again.”
9. Pediatric Practice
A pediatric practice with five physicians had a particular challenge. Their payer mix included several Medicaid managed care plans with extremely low reimbursement rates. The practice was committed to serving all patients regardless of insurance, but the financial strain was real. They needed either better rates or to reduce their Medicaid patient panel.
Medwave’s negotiation approach resulted in:
- 16% rate increase with three managed care plans
- New enhanced payments for care management services
- Improved reimbursement for after-hours care
- Quarterly bonuses for meeting preventive care benchmarks
“We didn’t want to stop seeing Medicaid patients, but the economics were becoming impossible,” explains the lead physician. “Better contracts let us continue our mission while staying financially stable.”
10. Dermatology Practice
A dermatology practice had decent reimbursement rates for office visits but terrible rates for procedures and surgical services. Since procedures made up roughly 40% of their revenue, this created a significant financial gap. Previous attempts to negotiate better procedural rates had gone nowhere.
Working with Medwave, they secured:
- 33% increase on procedure reimbursement rates
- Better payment for Mohs surgery and reconstruction
- New rates for advanced dermatologic procedures
- Elimination of problematic pre-authorization requirements for common procedures
“The payers were happy to pay reasonable rates for office visits but tried to lowball us on procedures,” says the practice owner. “We needed someone who could make the case for fair procedural reimbursement and actually get it changed.”
The Medwave Approach
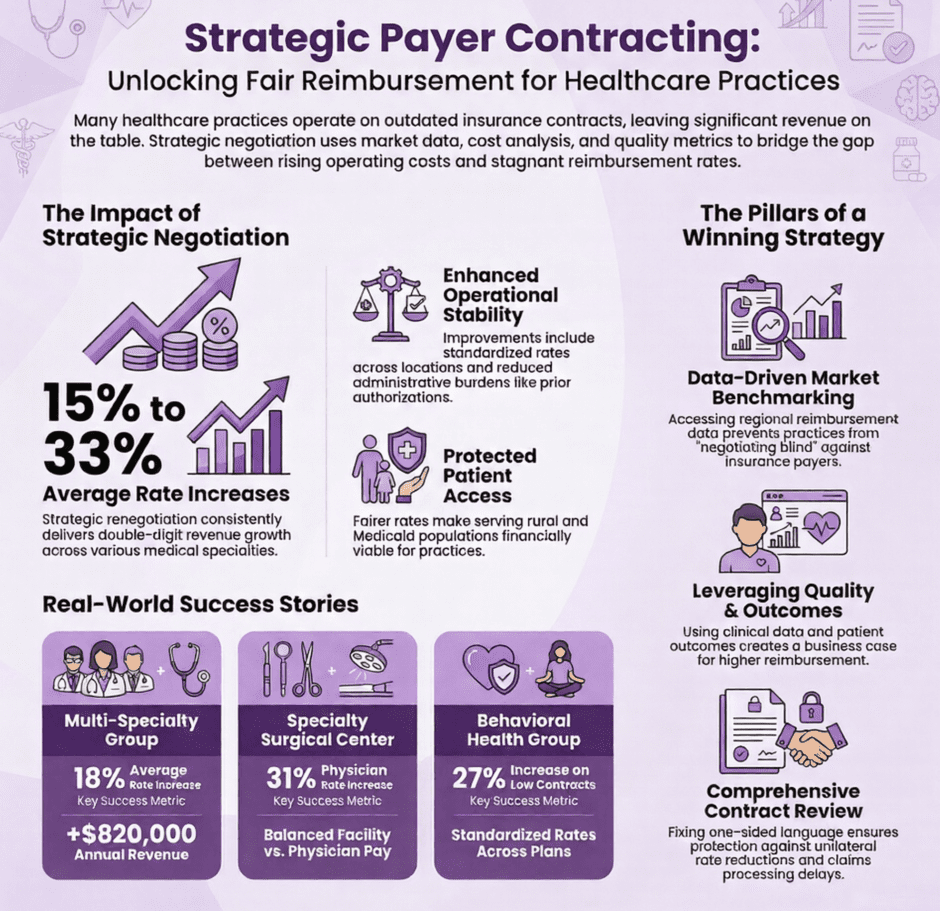
These use cases demonstrate consistent patterns in what works when negotiating with payers:
- Average rate increases of 15% to 33% across different specialties
- Improved contract terms beyond just rates
- Better alignment between reimbursement and actual care costs
- Long-term contract provisions protecting against future rate erosion
Our contracting methodology combines market data analysis with specific practice metrics to build strong negotiation positions.
Key elements include:
- Regional reimbursement benchmarking
- Cost of care analysis
- Quality metrics and outcomes data
- Patient access and network adequacy considerations
- Detailed contract language review
- Multi-year rate adjustment provisions
What Makes Payer Contracting Different
Unlike credentialing, which has relatively clear requirements and timelines, payer contracting involves actual negotiation. Insurance companies have entire teams dedicated to keeping reimbursement rates as low as possible. They use information asymmetry to their advantage. Most providers don’t know what rates are achievable, what leverage points matter, or how to structure the negotiation effectively.
Successful payer contracting requires several things most practices don’t have:
- Current market data: What are other providers in your specialty and region actually getting paid? Without this information, you’re negotiating blind.
- Cost analysis: What does it actually cost you to deliver different types of care? If you can’t document your costs, you can’t make a compelling case for rate increases.
- Quality metrics: Can you demonstrate better outcomes, higher patient satisfaction, or lower total cost of care compared to peers? These factors give you negotiating leverage.
- Contract expertise: Understanding what contract language means, what’s negotiable, and what provisions protect your interests long-term requires specialized knowledge.
- Negotiation strategy: When to push hard, when to compromise, and how to structure offers that address payer concerns while meeting your needs.
Common Contracting Challenges
The practices profiled here faced several recurring obstacles:
- Outdated contracts: Many practices discover their contracts haven’t been renegotiated in 5, 8, or even 10+ years. Costs have risen substantially, but rates haven’t budged.
- Information gaps: Practices don’t know what fair rates look like for their specialty and region. This makes it impossible to know whether current rates are acceptable or problematic.
- One-sided terms: Payer contracts are typically written to favor the insurance company. Provisions around claims processing, payment timelines, and dispute resolution often heavily favor the payer.
- Limited leverage: Individual practices feel they have little negotiating power, especially with dominant regional payers. This perception often prevents them from even trying to negotiate.
- Time and expertise: Practice administrators are already overwhelmed. Adding complex contract negotiations to their workload isn’t realistic, and they may not have the specialized knowledge needed anyway.
The Strategic Value of Better Contracts
Improved payer contracts deliver value in multiple ways:
- Direct revenue increase: Higher reimbursement rates obviously mean more revenue for the same services. For most practices, even a 10% to 15% rate increase translates to hundreds of thousands in additional annual revenue.
- Operational stability: Predictable, fair reimbursement rates make financial planning easier. Practices can budget for equipment, hire staff, and invest in improvements with more confidence.
- Provider satisfaction: When physicians and other providers know they’re being paid fairly for their work, morale improves. Compensation models tied to revenue become more sustainable.
- Patient access: Better reimbursement rates can allow practices to continue accepting insurance plans they might otherwise need to drop. This maintains patient access to care.
- Strategic flexibility: Improved revenue creates options. Practices can invest in new service lines, upgrade technology, or expand to new locations.
Why Practices Wait Too Long
Despite the clear benefits, many practices put off addressing contract issues until they reach a crisis point.
Common reasons include:
- They assume payers won’t negotiate and it’s not worth trying. This is often wrong. Payers negotiate regularly, but only when providers make a strong case.
- They worry about damaging payer relationships. In reality, payers expect periodic rate negotiations and don’t view professional negotiation as adversarial.
- They lack internal resources to handle negotiations. This is legitimate, which is why many practices work with contracting specialists.
- They don’t realize how much money they’re leaving on the table. Without benchmarking data, it’s hard to know your rates are problematic.
- They’re focused on other priorities. Payer contracting gets pushed down the list behind more immediate operational concerns.
When to Renegotiate
Several situations signal it’s time to address your payer contracts:
- Your contracts haven’t been renegotiated in more than three years. Costs rise continuously, so rates should too.
- You’re seeing more claim denials or payment delays from specific payers. This often indicates contract language problems.
- Your practice has grown or changed significantly. New service lines, different patient acuity, or practice expansion may warrant rate discussions.
- Regional competitors are getting better rates. If you have data showing other practices are paid more for similar services, that’s strong justification for negotiation.
- You’re considering dropping insurance plans because rates don’t cover costs. Before taking this step, attempt to negotiate better rates.
- Annual contracts are coming up for renewal. Contract renewal is the natural time to discuss rate improvements and term changes.
The Process Works
 The practices featured in these payer contracting use cases span different specialties, practice sizes, and geographic regions. But they all achieved measurable improvements through strategic payer contracting. Rate increases ranged from 15% to 33%. Contract terms improved across the board. Practices secured better payment provisions, reduced administrative burdens, and gained protection against future rate erosion.
The practices featured in these payer contracting use cases span different specialties, practice sizes, and geographic regions. But they all achieved measurable improvements through strategic payer contracting. Rate increases ranged from 15% to 33%. Contract terms improved across the board. Practices secured better payment provisions, reduced administrative burdens, and gained protection against future rate erosion.
At Medwave, our team handles billing, credentialing, and payer contracting for healthcare providers across specialties. We bring market data, negotiation expertise, and proven strategies to help practices secure fair reimbursement rates and favorable contract terms. The work these providers put into contract negotiations delivered returns that will continue for years to come.
The use cases above show what’s possible when you approach contract negotiations strategically with the right support and data behind you.

