
RPA is Key to Improving Revenue Cycle Management
Robotic Process Automation (RPA) refers to the use of software robots to smartly automate repetitive and rule-based tasks. Within healthcare revenue cycle management, RPA can be used to streamline various tasks such as claims submission, payment posting, and denial management.
For example, an RPA system can be programmed to automatically retrieve patient data from electronic health records, verify insurance eligibility, submit claims to insurance companies, and follow up on any claim denials. This automation can significantly reduce the time and effort required for these tasks, improve accuracy and efficiency, and allow healthcare staff to focus on more complex tasks that require human expertise.
Additionally, robotic process automation can also help healthcare organizations reduce costs associated with medical billing by eliminating errors, reducing the need for manual labor, and improving the speed of processing claims. Overall, automation can be an effective tool to help healthcare organizations improve their revenue cycle management and ultimately provide better care to their patients.
Systematic Revenue Cycle Management
The following factors must be addressed:
- Scheduling appointments
The process of producing a methodical yet patient-centered procedure of scheduling appointments that provides the patient the time priority needed. - Insurance eligibility certification
The insurance specifics and eligibility criteria required from the patient and then confirmed through the proper procedures. - Setting up a patient account
A procedure that initiates the patient’s account within the healthcare organization and is constantly brought up to date based on subsequent services provided. - Medical history ID
The upkeep of a detailed record that looks into into the patient’s medical history and all the pertinent issues that may or may not affect the patient’s health. - Insurance coverages
Pinpointing the patient’s insurance authorizations and coverage and their impact on the processes for claims reimbursement, denial management, etc. - Patient claims history
An analysis of the history of the patient that identifies if any claims have been rejected in the past, along with a record of the denial management. - Medical billing
The process of producing accurate medical bills for the services provided.
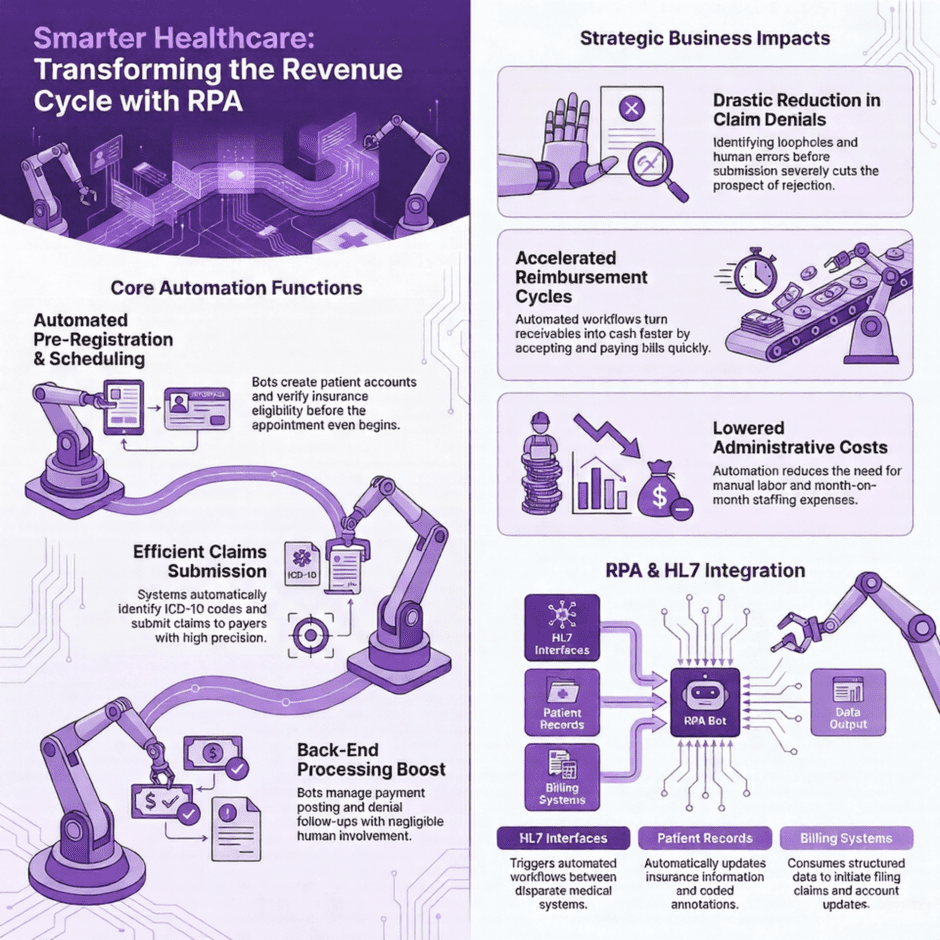
Automating the Revenue Cycle
Streamlining Patient Access and Scheduling
The foundation of a healthy revenue cycle begins with automated pre-registration and scheduling. Using an automated procedure to produce patient accounts enables your practice to ensure that medical history, insurance coverage, and vital details are captured accurately from the start. This efficiency extends to patient scheduling, which creates a seamless method for arranging both initial and follow-up appointments. These systems keep the patient as the chief concern, removing administrative friction before they even walk through your door.
Precision Billing and Claims Management
Automated billing transforms the way invoices are generated and managed. Through basic data entries, the system pinpoints claims, carries out verification, and submits medical bills in the most efficient manner possible. This technology is especially effective at reducing claims rejections and returns. By recognizing loopholes and human errors that typically lead to denials, the prospect of a rejected claim is severely cut. Furthermore, the system automates ICD-10 code identification and treatment descriptions, leading to more effective claims submission and much quicker reimbursement.
Optimizing Financial Performance and Workflow
Automation ensures that no revenue is left behind by identifying every service that converts into a billable charge. These charge capture duties are documented through automatic significance, ensuring total accuracy. The software also boosts back-end processes by managing payment posting, statement handling, and collections with negligible human involvement. This leads to a much faster turnaround for receivables, as claims are accepted and bills are paid at an accelerated rate.
Operational Efficiency and Cost Savings
Beyond speed, these automated processes offer a significant reduction in monthly costs. Leaning on automated systems to handle repetitive tasks lessens the need for a large administrative staff. This saves your practice the recurring expense of extra personnel while maintaining a high level of accuracy. The result is a leaner, more disciplined office environment where technology handles the paperwork so your team can stay focused on the patients.
Healthcare Revenue Cycle Workflow Automation in Practice
The objective of workflow automation is to make best use of a healthcare facility’s revenue cycle and make sure claims are paid swiftly. This is a win-win. The healthcare provider collects timely payment, while patients go through a effortless, error-free visit to the doctor.
To realize these two goals (an enhanced revenue cycle and claims paid swiftly) it’s important to gather correct information from the very start, when a patient account is initiated.
In a recent case study, it was found that employees at a hospital in New York were obliged to accomplish tiresome tasks and enter relative data. Repetitive work can clearly lead to weariness and unintended mistakes. As a result, the hospital team realized the need to modernize these procedures and instigate workflows and systems to enhance accuracy and make sure the best exercise of personal time.
Since workflow is a cycle, each step flows into the ensuing step. If the original information is recorded with mistakes or essential information is missing, small errors can result in major problems in later steps.
Workflow Automation Subsists to Rid These Errors
Healthcare revenue cycle workflow automation systems achieve the following tasks:
- Concentrate on front-end tasks to push claims along
- Migrate patient files and produce non-patient files
- Proactively confirm and revise patient information
- Automatically add coded annotations
- Substantiate insurance information before a patient’s visit
- Revise obsolete or missing policies prior to an appointment
Why Workflow Automation Should Matter
As a decision-maker at a healthcare facility, you’re devoted to boosting revenue and reducing the costs of your facility. Automation helps make this stress-free. When healthcare facilities invest in workflow automation software, they benefit it two main ways: reducing expenses and improving workflow.
Making an investment in a system to proactively double-check patient information allows healthcare facilities to reduce human error, enhance the organization’s revenue cycle workflow, curtail expenses and devote more time on revenue-generating, value-added efforts.
Medical Billing Robotic Process Automation is not only a shrewd investment, but a healthy one.
HL7 and FHIR: The Data Standards Powering Smarter RPA

Most healthcare organizations run on a mix of systems that were never designed to talk to each other. Electronic health records, billing platforms, practice management software, and imaging systems all hold pieces of the same patient’s information, but getting that data to flow cleanly between them has historically required a lot of manual work. That is where HL7 and FHIR come in, and why they matter so much to RPA.
HL7, which stands for Health Level Seven, is a set of messaging standards that defines how clinical and administrative data is formatted and exchanged between healthcare systems. When your EHR sends patient information to your billing system, or when a lab result needs to trigger a follow-up workflow, HL7 is typically the framework making that exchange possible. RPA bots can read and act on HL7 messages in real time, automatically triggering downstream tasks like creating patient accounts, updating insurance records, filing claims, and flagging discrepancies, all without a person having to touch the data manually.
FHIR, which stands for Fast Healthcare Interoperability Resources, takes this a step further. Developed by the same standards body, FHIR uses modern web-based technology to make data sharing faster, more flexible, and far easier to work with than older HL7 formats. Where traditional HL7 messages can be dense and difficult to parse, FHIR organizes clinical data into modular, standardized building blocks called resources, covering everything from patient demographics and medications to claims and coverage information. That structure makes FHIR-based data exceptionally well-suited for RPA, because bots can reliably locate, extract, and act on specific data points without the kind of error-prone workarounds that unstructured data requires.
Together, HL7 and FHIR create the data foundation that allows RPA to work at scale. When a patient’s insurance information updates in the EHR, an HL7 or FHIR message can automatically trigger a bot to verify eligibility, update the billing record, and flag any coverage gaps before the next appointment. When a claim is ready to submit, bots can pull the relevant FHIR resources, confirm that all required data fields are populated correctly, and route the claim to the appropriate payer without manual intervention.
Federal interoperability requirements continue to push healthcare organizations toward FHIR adoption. The connection between these standards and RPA will only grow stronger. Practices that invest in HL7, FHIR integration now are not just improving today’s workflows. They’re building the infrastructure that makes broader automation possible as their systems and data needs grow.
Reach out to us today, in order to hear about our RPA solutions and whether it’s a good fit against your claim volume, etc,. We can tackle all of your revenue cycle automation needs.
